Based on Your Reading:
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Studies have shown that people who were exposed to asbestos have an increased risk of lung cancer. Each year, 6,000 people in the U.S. die from lung cancer linked to asbestos exposure. Asbestos-related lung cancer may develop 15 to 35 years after asbestos exposure.
Written by Suzanne Dixon, MPH, MS, RDN • Edited By Walter Pacheco • Medically Reviewed By Dr. Jacques Fontaine
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Dixon, S. (2024, April 18). Asbestos-Related Lung Cancer. Asbestos.com. Retrieved April 18, 2024, from https://www.asbestos.com/cancer/lung-cancer/
Dixon, Suzanne. "Asbestos-Related Lung Cancer." Asbestos.com, 18 Apr 2024, https://www.asbestos.com/cancer/lung-cancer/.
Dixon, Suzanne. "Asbestos-Related Lung Cancer." Asbestos.com. Last modified April 18, 2024. https://www.asbestos.com/cancer/lung-cancer/.
Only a small percentage of lung cancer cases are primarily linked to asbestos. Tobacco smoking accounts for about 80% of lung cancer deaths in the United States. Exposure to asbestos increases the risk of lung cancer in smokers and non-smokers.
Lung cancer is the leading cause of cancer death in the United States. It kills more Americans each year than breast, prostate and colon cancer combined. Lung cancer caused by asbestos is responsible for an estimated 6,000 deaths in the U.S. each year.
Quick Facts About Asbestos Lung Cancer
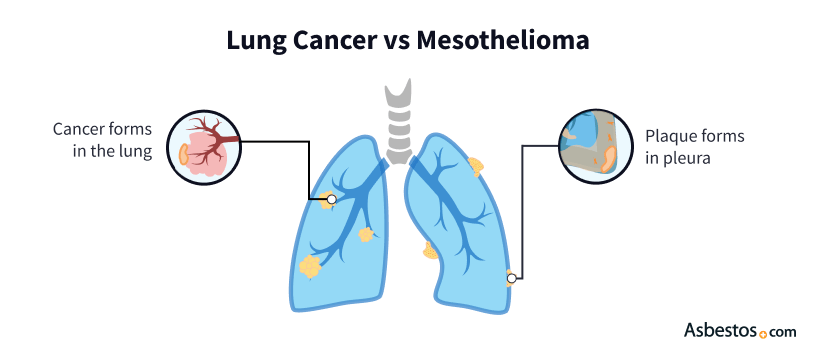
Asbestos lung cancer and pleural mesothelioma are two different diseases caused by asbestos exposure. Lung cancer caused by asbestos develops inside the lung, while pleural mesothelioma develops in the lining of the lungs. Both diseases take decades to develop, but can spread or metastasize within months.
Pleural mesothelioma and asbestos lung cancer involve similar diagnostic procedures and symptoms, but they differ in physical characteristics and treatment techniques. Asbestos exposure is the primary cause of mesothelioma, while smoking is by far the leading cause of lung cancer.
But asbestos exposure causes six times more cases of lung cancer than mesothelioma. Lung cancer claims the most lives of all asbestos-related diseases.
When a person inhales asbestos, microscopic fibers can become lodged in their lung tissue. Researchers have been studying just how these asbestos fibers cause cancer and found evidence that asbestos may spark changes within DNA itself.
The International Agency for Research on Cancer is the specialized cancer agency of the World Health Organization. In 2017, IARC conducted an extensive research study that provided new evidence to connect asbestos and a chemical reaction that changes specific genes in the body.
This chemical reaction – DNA methylation – impacts biological processes. IARC researchers explained that “epigenetic mechanisms such as DNA methylation are fundamental in the regulation of gene expression and carcinogenesis.” Carcinogenesis is the beginning of cancer formation.
Significantly impacted biological processes include:
While the asbestos can trigger the body’s nervous system to fuel tumor development and spread, the process itself may take decades from the point of exposure until the onset of symptoms. Asbestos-related lung cancer typically takes between 15 and 35 years to develop.
Because of this long latency period, most cases diagnosed today began with occupational asbestos exposure that occurred decades ago. Veterans and others connected with military service are at high risk because asbestos use in the military was extensive. Mining, construction, heavy industry, shipbuilding and firefighting are also high-risk groups.
While not all people exposed to asbestos will develop lung cancer, those exposed to large amounts of asbestos for long periods of time are at the most risk.
Risk factors for asbestos lung cancer include:
According to an international study published in 2020, no substance causes more cases of lung cancer linked to occupation than asbestos. The study found that asbestos is responsible for 37.5% of all occupational lung cancer cases.
The risk of lung cancer is much higher among asbestos-exposed smokers because smoking impairs the lungs’ ability to remove asbestos fibers. Smokers who have been exposed to asbestos should stop smoking immediately and seek annual screenings for lung cancer.
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Whether lung cancer is associated with asbestos exposure, smoking or another cause, it presents the same general symptoms:
These symptoms typically only arise once lung cancer reaches a late stage of development, when the cancer is tougher to treat. People with a history of asbestos exposure should seek regular screening for asbestos-related diseases.
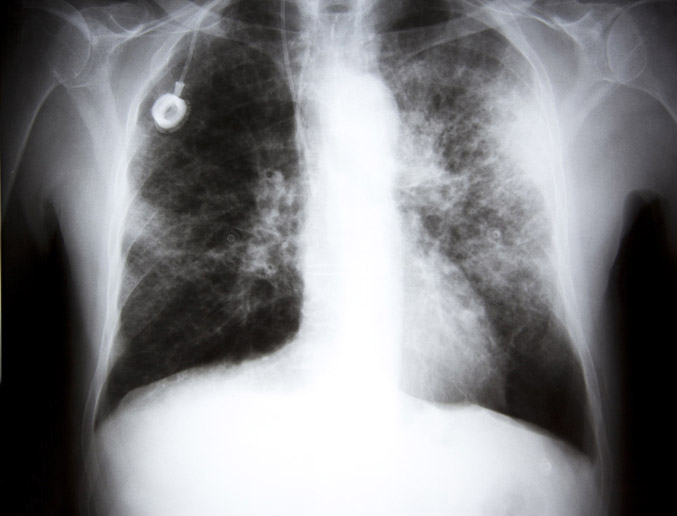
The diagnostic process begins with imaging scans such as X-rays and CT scans. A 2021 clinical research study noted that PET-CT scans of patients with asbestos-related lung cancer showed comparable sensitivity and specificity to similar scans of patients with conventional lung cancer.
A pathologist must examine a biopsy sample of suspicious tissue to confirm a lung cancer diagnosis.
A biopsy may be extracted through a long needle or with a bronchoscope, which is passed down the throat and into the airways of the lungs.
Treatment options for asbestos-related lung cancer include surgery, chemotherapy, radiation therapy and immunotherapy.
Aggressive treatments aim to remove or kill cancer cells to prevent the spread of cells and tumors. Palliative therapies help ease pain and other symptoms to improve quality of life.
The prognosis for lung cancer depends on the type and subtype of the disease. It also depends on the patient’s overall health and how far the cancer has spread by the time it has been diagnosed (the stage of the cancer).
About 18% of lung cancer patients survive more than five years after diagnosis, according to the American Lung Association. This is significantly lower than other leading cancers such as breast (89.6%) and prostate (98.2%).
More than half of lung cancer patients die within one year of being diagnosed.
There are two primary forms of lung cancer: Small cell and non-small cell. Asbestos exposure can cause any of the various types and subtypes of lung cancer.
Non-small cell lung cancer (NSCLC) accounts for about 85% of all lung cancer cases. There are three subtypes of non-small cell: Squamous cell carcinoma, adenocarcinoma and large cell carcinoma.
Small cell lung cancer (SCLC) makes up 10% to 15% of cases and is more difficult to treat. The cancer can spread to other parts of the body before presenting any symptoms.
Unfortunately, surgery is rarely an option with SCLC because of this factor. Doctors instead rely on chemotherapy that attacks cancer cells throughout the body.
The Helsinki Criteria were established in 1997. These standards help doctors determine if asbestos is the primary cause of respiratory diseases.
Asbestosis and lung cancer are commonly associated. This is because the risk for both rises as asbestos fibers accumulate in lung tissue.
The presence of asbestosis is a reliable diagnostic marker that a patient was exposed to asbestos enough to develop lung cancer.
Asbestos exposure can cause any type of lung cancer. The two broad classifications of lung cancer are non-small cell and small cell, which are subcategorized by cell type. People with a smoking history are more susceptible to asbestos-related lung cancer. Asbestos is also the primary cause of pleural mesothelioma, which forms in the lining outside the lungs and is not considered lung cancer.
Not every person exposed to asbestos will develop lung cancer or other asbestos-related diseases. A person’s risk of illness will increase relative to their level of exposure to asbestos. Frequent and extended periods of concentrated asbestos exposure present the highest risk.
All forms of lung cancer originate inside the lungs. Mesothelioma is also cancer, but it develops in the tissue that lines the outside of the lungs, chest cavity and abdomen. Asbestos exposure can cause both types of illness.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
