HIPEC Surgery: Exhausting, but Worth It, Says Mesothelioma Survivor
Peritoneal mesothelioma can be two of the most frightening words you will ever hear.
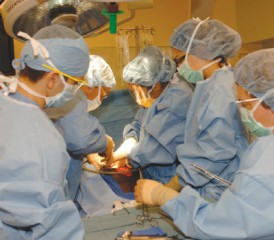
The only thing worse than the disease itself: Coming to grips with the fact that there are few treatment options. One of the most common procedures for mesothelioma patients is cytoreductive surgery with HIPEC treatment to follow.
During this procedure, all visible tumors are removed. Once that step is complete, a chemo solution is poured directly into the abdomen, and heated to kill any remaining cells that can go unseen.
After choosing my surgeon, it was time to prepare myself for the biggest, most invasive procedure I would ever have. I spent an entire day drinking Miralax cocktails. It was a grueling, nauseating and exhausting day. The next day was operation day. After saying goodbye to my husband, I was off to surgery. I received an IV in my left hand and two nerve blocks.
Eight hours later, I remember waking up to various beeps and monitors all around. I couldn’t speak or move my body, just my eyes. My first thought: “I’m still alive!” I was informed that I was in ICU.
I survived part one of the ordeal.
Hunger Pains
I remember being hungry, and all I could eat was a piece of crushed ice every four hours. The following morning, still in a medically induced fog, my physical therapist came to get me out of bed. Once I knew she was serious and not joking, I didn’t know whether I would cry or curse.
I was catheterized, couldn’t move and this lady wanted me out of bed? She managed to get me out of bed with the help of a walker. I think I made it from my bed, to the door and then back again.
I had a love-hate relationship with my physical therapist. I loved that she was helping me recover, but I absolutely hated that my recovery depended on me getting out of bed. I was amazed at how exhausted I felt after walking 10 feet. Here I was, a 34-year-old woman with tubes everywhere, walking with a walker. I couldn’t believe that this was my life.
On the second day after the operation, I was moved into a regular room. I had graduated to a shot glass of water every couple of hours instead of ice, but I was still in starvation mode. At this point, I was fighting for anything with flavor.
Day 4 was finally here. I recovered enough to eat half of a Popsicle. I was so excited. As I bit into it, tears began to fall. That was the worst Popsicle I’d ever eaten. It could have been frozen Robitussin on a stick, that’s how bad it was.
From Hospital Bed to Preparing a Birthday Party
Another tube came out each day, and my walks were longer. After a week, I no longer needed the walker. Two and a half weeks later and I was at home, preparing for my son’s second birthday party.
Sounds like a cake walk, right? It was emotionally hard to be hundreds of miles away from home for three weeks. My body is scarred for life, and I have HIPEC memories that will last forever. Having two HIPEC procedures under my belt, I would say that I’m a pro. The second time around was definitely easier than the first because I knew what to expect. My recovery also was faster this time.
There is no easy way to prepare for a HIPEC procedure. It’s a matter of survival: Do or die. For me, it was a no-brainer that I must undergo the procedure. If I needed a third HIPEC, I would do it in a heartbeat, but ask for a better tasting Popsicle.