
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free Guide
Written by Matt Mauney | Edited by Walter Pacheco
Historically, mesothelioma cancer mostly affects older men exposed to asbestos while they served in the military or worked certain blue-collar jobs. But women now comprise nearly one-fourth of all cases, and mesothelioma incidence rates among women are on the rise, showing the gender gap is closing.
Raeleen Minchuk has inspirational sayings and mementos displayed throughout her new home in Calgary, Alberta.
One of those sayings, “A child is a mother’s anchor to life,” best defines the Canadian.
My kids are my anchors to this life. They are what make me fight so hard and never give up.
Minchuk was only 36 when she received her devastating stage III peritoneal mesothelioma diagnosis in October 2014. She marks her two-year anniversary of remission on February 19.
Although she continues to deal with physical and mental hardships, Minchuk is once again able to focus on her true passion in life: Motherhood.
Minchuk is one of a growing number of women living with mesothelioma.
Mesothelioma is a rare cancer diagnosed in roughly 3,000 people in the U.S. annually. Women now represent a quarter of those diagnoses, according to the Surveillance, Epidemiology and End Results (SEER) database, which has tracked mesothelioma incidence rates since 1975.
Incidence rates among women are up 8% compared to SEER’s average male-to-female ratio.

Doctors are diagnosing many of these women at a younger age than men, too. And as more women develop the incurable asbestos-related disease, they face numerous challenges their male counterparts will likely not experience during their cancer journey.
“Many people don’t know what it’s like when someone looks you in the eyes and tells you you’re going to die,” Minchuk said. “You’ve got a fear you’ve never felt inside of you, but you try to remain positive, and I have to because I have children.”

Exposure to asbestos, a naturally occurring mineral, is the primary cause of mesothelioma.
Until the 1980s, asbestos was the go-to material for construction and manufacturing products. Because of its versatility and fire-resistant properties, it was added to insulation, floor tile adhesives and drywall. It was mixed into cement and woven into fabric.
The military also used asbestos extensively. It seemed to be an ideal answer for insulating boiler rooms on U.S. Navy ships and proved useful when added to brake pads and clutch pads found in jeeps, tanks and aircraft.

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideUnfortunately, it is also highly toxic. When asbestos products are cut, ground, worn down or otherwise disturbed, microscopic fibers can become airborne. Inhaling or ingesting these fibers can lead to serious health issues such as mesothelioma cancer, asbestosis and asbestos-related lung cancer.
No amount of asbestos exposure is considered safe, but heavy, repeated exposures generally lead to asbestos-related diseases. When asbestos use was at its peak, men were the primary workforce in high-risk occupations such as construction, shipyard work, other industrial jobs and roles within the U.S. military.
Many of these veterans are now getting sick. It can take 20-50 years after first exposure until the onset of symptoms.
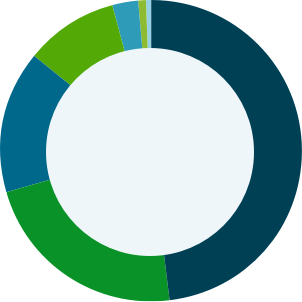
Percentage of Women in High-Risk Occupations
While more women are now employed in blue-collar occupations, current jobs that put workers at the highest risk for asbestos exposure are still dominated by men. According to a 2010 report from the U.S. Department of Labor, women are more than a quarter of the workforce in only one of these high-risk jobs (manufacturing) and these percentages were much lower at the height of asbestos use.
So why then do the latest SEER stats show women account for nearly 1 in 4 new mesothelioma cases?
The answer may lie outside of traditional occupational asbestos exposures.
Judy Goodson, 62, is a perfect example that asbestos exposure doesn’t only occur in mines, factories or the shipbuilding industry.
After returning home from receiving her mesothelioma diagnosis in March 2013, she racked her brain thinking when and where her exposure could have occurred.
“I knew mesothelioma came from asbestos, so the first thing I asked myself was where the hell was I?” Goodson told Asbestos.com.
Her father worked in steel mills, which were notorious for using asbestos as an insulation material. She would regularly wash his work clothes, which were often covered in dust.
Asbestos fibers inadvertently brought home from the workplace can lead to what is known as secondary or secondhand exposure. Steel mill workers and those in other occupations have accidentally put their family at risk by unknowingly bringing home asbestos fibers on their clothes, shoes, hair or skin.
For a long time, I felt so guilty. I thought where was I and what did I do wrong? I was blaming myself, but it’s not my fault.
Occupational asbestos exposures can also occur in seemingly unlikely places such as schools and office buildings. Although the use of asbestos has dropped significantly in recent decades, asbestos-containing building materials remain prevalent in older infrastructure.
“I worked in offices for years where there were ceiling tiles and tile floors being torn down and torn apart,” Goodson recalls.

When she was in the ninth grade, Goodson’s junior high school was remodeled. Huge plastic sheets separated the renovation areas from teachers and students — nowhere near the proper amount of protection needed during asbestos abatement.
Asbestos removal is a delicate process and should only be performed by certified asbestos abatement professionals. When asbestos-containing materials are disturbed during renovations and construction, toxic fibers can easily travel through the air, ventilation and irrigation systems.
As more offices, homes and schools built before the 1980s are renovated, the possibility of exposing unsuspecting occupants of these buildings to asbestos remains high.
“All this stuff now comes to you,” Goodson said. “Nobody thought about it back then.
Minchuk represents an uncommonly young demographic of mesothelioma patients diagnosed with the asbestos-related cancer before age 40.
But that demographic — especially among women — is growing.
From 2009 to 2013, more women between ages 35-39 were diagnosed with mesothelioma than men in that age range, according to SEER’s age-adjusted and age-specific incidence rates. The latest SEER data (2010-2014) shows women have nearly the same chance of developing the cancer than men before age 50.
This is the main reason why the majority of mesothelioma cases — among men and women — are diagnosed at ages 75-84.
A 2022 CDC report indicated that the annual number of mesothelioma deaths among women increased significantly over the past twenty years, from 489 in 1999 to 614 in 2020. However, the age-adjusted death rate per 1 million women declined significantly, from 4.83 in 1999 to 4.15 in 2020.
Secondhand and other non-occupational exposures may be the answer to the increasing number of women diagnosed with mesothelioma at a younger age.
Minchuk believes she was first exposed to asbestos as an infant.
Her father renovated her grandparents’ home in 1979, when dangers of the toxic mineral were not as well known as they are today.
Through her story, she hopes to raise awareness that mesothelioma can happen to anyone, regardless of age, gender or work history.
I always try to stress to people that it’s real and can happen. My life was predetermined at 1 year old that I was going to get sick and going to die.
She now lives every day focusing on the positives in life, not knowing if or when the cancer will return.
“Today there is much more awareness, but still, people push the limits on it and think that it won’t happen to them,” she said. “They don’t want to pay for that abatement, and there are so many contractors that go into government buildings and don’t even know that there’s asbestos in there.”
Kasie Coleman, 41, vividly remembers her diagnosis in July 2010.

“It was like someone took every breath out of my body,” Coleman told Asbestos.com. “You just want to collapse. Then you start reading prognoses and all this stuff and you just think oh my God, I can’t.”
The 7-year survivor was just 34, and it took 18 months of recurring symptoms before doctors finally determined she had peritoneal mesothelioma.
Coleman’s history of asbestos exposure dates to her teenage years. Her high school was demolished because of exposed asbestos. It was something she never gave much thought until that day in 2010.
She urges women to not become complacent and to “keep digging” if they feel a diagnosis is inaccurate.
“This disease is so rare; it’s not like people are looking for it,” she said. “I would tell women to definitely pay attention to their bodies. I was persistent, and it took a year and a half. I had it the whole entire time.”
Because it is such a rare disease, there are few mesothelioma specialists and top cancer centers that treat it effectively.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your DoctorColeman had to travel nearly 1,200 miles from her home in Baton Rouge, Louisiana, to be treated at UPMC Hillman Cancer Center in Pittsburgh.
After a series of surgeries and chemotherapy treatments, Coleman has been in remission since June 2012. She now lives her life 180 days at a time, going in for checkups every six months at the Cancer Treatment Centers of America in Tulsa, Oklahoma.
For me, I never focused on the statistics and all that stuff because that’s depressing in itself. Now, I’ve been healthy for so long that I don’t think about it like that anymore. I take it as I was cured, and I’m living my life as such.
There are four types of malignant mesothelioma. The pleural type, which develops on the protective lining of the lungs, accounts for approximately 75% of all cases.
Peritoneal is the second-most-common type and forms on the peritoneum, the membrane that lines the abdominal cavity. While it only accounts for about 20% of all cases, twice as many U.S. women die of peritoneal mesothelioma each year compared to pleural.
According to CDC data, there were four years between 2001 and 2010 where more women died of pleural mesothelioma than peritoneal. Since 2011, peritoneal has held the majority, and the ratio is widening.
In cases of peritoneal mesothelioma, patients often swallowed asbestos fibers at some point in their lives. These fibers travel from the digestive system to the peritoneum, where they can become lodged and remain there for decades, potentially leading to the formation of malignant tumors that place pressure on the organs.
Asbestos fibers can also reach the peritoneum through the lymphatic system.
Beginning symptoms of peritoneal mesothelioma include abdominal pain, swelling or tenderness around the abdomen, diarrhea and constipation.
Generally, patients diagnosed with peritoneal mesothelioma have a better prognosis and longer life expectancy compared to patients with the pleural type.
However, because the number of overall peritoneal cases is low, the cancer is often misdiagnosed. A diagnosis in the later stages after tumors have spread can make treatment more difficult and result in a less favorable prognosis.
The amount of clinical trials and oncologists specializing in treating peritoneal mesothelioma is also small.
One of the most promising treatment options for peritoneal mesothelioma is a multimodal therapy exclusive to patients with abdominal cancers.
Cytoreductive surgery — which removes as much cancerous growth as possible from the abdomen — is followed by hyperthermic intraperitoneal chemotherapy (HIPEC). Goodson calls it “shake and bake.”
“They heat the chemo, pour it in there, and they rock you,” Goodson said. “After your surgery, they can rock you for like eight hours.”
Goodson said she’s medically blessed with a team of primary care doctors and local oncologists who were persistent after discovering “mystery spots” around her bladder.

That persistence eventually led her to Dr. Sophie Dessureault, a gastrointestinal oncologist at the multidisciplinary Moffitt Cancer Center in Tampa.
In 2013, Dessureault was the lead surgeon involved with Moffitt’s groundbreaking study detailing the benefits of the cytoreductive surgery and HIPEC combination as a treatment for peritoneal mesothelioma.
Dessureault noted that HIPEC is limited for peritoneal mesothelioma patients, depending on the amount of tumor growth.
“Even if the tumor is responsive to the chemotherapy regimen, the systemic toxicity ultimately reaches a level at which further chemotherapy can no longer be administered,” Dessureault told Asbestos.com.
The role and potential benefits of heated chemotherapy for pleural patients is less clear.
HIPEC has shown promising results for peritoneal patients. Doctors perform the multimodal therapy on a case-by-case basis.
It worked for Goodson, who is nearing four years of remission.
Coleman went through two cytoreductive surgeries and a pair of HIPEC procedures. It was a long, expensive and painstaking process, but she is in remission for five years and counting.

An extensive cytoreductive surgery removed nearly everything from Minchuk’s abdominal cavity, including all but seven feet of her intestines. She suffers from severe malnutrition because of her gastrostomy — an opening (ostomy) into the stomach from the abdominal wall — and peripheral neuropathy from chemotherapy.
She works out 3-4 times a week with her youngest son, Tyce, who constantly pushes her to get stronger.
With only seven feet of intestines, Minchuk is limited when it comes to exercising. She focuses on light cardio and extensive leg work, including 140-pound squats and leg pressing 240 pounds.
I have this goal to be the first woman to have a six-pack with an ostomy. That’s the goal I have in my head — to get back the athleticism from when I did sports and what not.
Because women don’t fit the traditional mesothelioma patient profile of older men who work in high-risk jobs, they are often misdiagnosed with female-related conditions when mesothelioma symptoms begin to emerge.
When a woman presents with symptoms, mesothelioma is not something the physician is suspecting to find.
Karen Selby, a registered nurse, has seen an increase in mesothelioma cases among women since she joined The Mesothelioma Center in 2009.
“Because of the potential delay in diagnosis, this may mean the diagnosis will be discovered at a more advanced stage,” Selby said. “This may impact the treatment path and overall prognosis.”
Dessureault has seen many instances where mesothelioma was misdiagnosed.
“We even had a patient who had undergone HIPEC in the past, and when she underwent a ventral hernia repair at an outside institution, she was told that the hernia sac had evidence of metastatic adenocarcinoma,” she said.
After reviewing the biopsies at Moffitt, oncologists confirmed the woman had peritoneal mesothelioma and not a new cancer diagnosis.

Discover financial assistance programs, insurance guidance, and veteran benefits to help cover your mesothelioma treatment expenses.
Explore Your OptionsIt took Coleman a year and a half and five misdiagnoses before she received her peritoneal mesothelioma diagnosis.
“First it was bruised ribs; second was chlamydia. Then it was irritable bowel syndrome, then gallstones and finally ovarian cancer,” Coleman recalled. “I can’t tell you the amount of people I’ve talked to that are no longer here because they just accept the first thing their doctor tells them.”
The misdiagnoses were frustrating, costly and even put a strain on her relationship. Coleman recalls being furious with her husband for several days following her chlamydia misdiagnosis.
Women, in particular, are misdiagnosed or ignored because of the stereotype of where it comes from — steel mills, industrial plants and so on. No, it comes from old buildings, too. I went to a school with exposed asbestos in the gym every day.
Doctors at the University of Texas MD Anderson Cancer Center ran a variety of scans and tests on Coleman. They found tumors, but they tested benign. She was told the tumors were likely the result of multiple childbirths. Fluid drained from her liver also came back benign and was chalked up to a random buildup.
But the symptoms returned.

“I had doctors ask me if I wanted cancer because I just kept pushing,” Coleman said. “People will look at you like you are crazy, but I knew something wasn’t right.”
Even following her mesothelioma diagnosis, Coleman kept digging and getting second opinions. When one doctor would tell her there’s nothing more they can do to treat her cancer, she would find another specialist.
Her persistence paid off.
“You’re only as clear as your last prognosis,” she said.
For years, manufacturers of asbestos products failed to properly warn employees of the dangers of the toxic mineral. Thousands of U.S. military veterans were never warned of the deadly long-term effects of asbestos, and now they battle mesothelioma and other related diseases.
These people may qualify for compensation, including bankruptcy trusts, settlements, VA claims and trial verdicts.
But women who developed mesothelioma from secondhand exposure, like Goodson, or from exposure as a high school student, like Coleman, usually cannot easily identify the products that led to their mesothelioma diagnosis because they didn’t directly work with the products as their male counterparts.
Filing an asbestos-related lawsuit or trust fund claim is a complicated process. Having a documented work history of asbestos exposure greatly helps a person’s case.
The inability to pinpoint exactly where the exposure happened or what manufacturers to file a claim against can significantly hurt a patient’s case.
Still, women such as Goodson, Coleman and Minchuk are just as much victims as construction workers, pipefitters and veterans exposed on job sites.
Because of the lack of available compensation, Coleman and many other women living with mesothelioma face mounting medical bills.
She constantly fights with her insurance company about flying to Tulsa every six months for checkups because it’s not an in-network treatment.
Honestly, I’m more afraid of insurance than I am of my own body. I think insurance companies need to be more educated. They treat all cancers as the same, and they’re not. Mesothelioma is not breast cancer. They’re paying it the same, but it’s not the same.
Current law prohibits health insurance plans from putting annual or lifetime limits on most benefits, but some policymakers under the Trump administration pushed to change that rule.
“When you think about lifetime max, I’ve met that already,” Coleman said. “I told my husband that if [the cancer returns], I’m screwed because the costs of the treatments are so ridiculous.”
While common female-related conditions can result in misdiagnoses, preventative care specific to women can sometimes reveal mesothelioma in the early stages.
Dessureault believes the higher incidence rate of peritoneal mesothelioma in women may be related to what she calls “incidental mesothelioma,” noting many cases are found “during laparoscopic exams for OB-GYN exams due to endometriosis or infertility or other ‘pelvic’ disease, before the mesothelioma causes any symptomatology.”
This may also explain why women often have a better prognosis than men. An early diagnosis allows for more treatment options to fight the tumors before they metastasize, or spread.
She also noted that she treats more women with papillary mesothelioma, which has a better prognosis than epithelioid mesothelioma, the most common mesothelioma cell type.
It’s been nearly four years since Sallie Morton’s pleural mesothelioma diagnosis.
Doctors gave her six months.
The 91-year-old moves a little slower than she did a year ago, but she still drives, shops and stays busy with clubs and activities at her California retirement community, where she’s still a social butterfly.
Morton was 87 when diagnosed with cancer — too old, she felt, to bother with mesothelioma treatment options.
“I’ve seen too many people on chemo,” Morton told Asbestos.com. “I said I wasn’t interested and didn’t want to spend my time between doctors and hospitals for that.”

There are more pressing issues. She has severe lymphedema in her leg and battles arthritis. Her eye doctor urged her recently to have cataract surgery.
“I said no thank you,” she recalled.
Morton sometimes has chest pain or other symptoms she believes may be related to her pleural mesothelioma, but she doesn’t pay it much attention.
“Everything else hurts a lot more than that,” she said.
These women break the mold of the stereotypical mesothelioma survivor.
It’s a small but tightly knit community. Coleman calls it a “strange sorority” that no one wants to be a part of, but you make the best of it with the shared connection.
Because the cancer is rare, Dessureault said many physicians do not realize the differences between the four types of mesothelioma. Pleural mesothelioma is often aggressive and rapidly progressive, while peritoneal mesothelioma can be more indolent and chronic.
Without being able to differentiate between types and stages, many doctors who don’t specialize in mesothelioma are unable to give patients much hope after therapy.
“As my practice grows, I see a spectrum of outcomes, from bad to good, so I can prepare new patients for the worse but also hope for the best,” Dessureault said.
Dessureault, Dr. Jacques Fontaine and other mesothelioma specialists at Moffitt never promise a cure, but they do provide care that allows patients to live a better and possibly longer life.
Patients appreciate the support we provide and the understanding that this is a disease they must learn to live with. Their courage inspires us.
Every mesothelioma survivor has their own unique story.
While Goodson, Minchuk, Coleman and Morton have varying experiences and hardships, they all share two sentiments: The importance of staying positive and the need for a strong support system.

Our free online support group helps patients and families cope with the emotional effects of mesothelioma.
Sign Up NowSupport can come in many ways. Coleman found support through her husband, who once offered to sell their home to pay the mounting medical bills.
Goodson found it through longtime neighbor and friend Polly Ball, as well as her power of attorney, Patsy Craft, who became her mentor during a difficult time.
“[Patsy’s] been with me all the way, anything that goes on, she’s always checking on me,” Goodson said of Craft. “Those two have been my rocks. They’ve been phenomenal.”
Morton sees very little of her family. Her son still lives in the remodeled house that led to her asbestos exposure. At 91, she’s lost many friends she’s made in the seven years living at her retirement community, but meeting new friends is never an issue. Her social life makes it easy to forget she’s living with pleural mesothelioma.
When I Googled my cancer, [Trina] was the first person that came up on Asbestos.com. I read her survivor story, and it resonated with me that there’s hope.
In addition to her two sons, Minchuk receives support and motivation from fellow peritoneal survivor Trina C., who was diagnosed on the same day 13 years earlier.
As a resident of Canada, where there are roughly only 50 cases of peritoneal mesothelioma diagnosed each year, Minchuk uses online support groups and communities to connect with other survivors.
Minchuk even has her own Facebook page where she shares updates about her cancer journey.
“There’s a lot of work to do in creating awareness,” she said. “There’s a hope for a cure. Everything has come a long way, but it’s hard because asbestos is everywhere, and for the next 50 years, you’re going to see more cases of it.”
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Mauney, M. (2026, February 12). Women: The New Faces of Mesothelioma. Asbestos.com. Retrieved May 19, 2026, from https://www.asbestos.com/featured-stories/women-new-faces-mesothelioma/
Mauney, Matt. "Women: The New Faces of Mesothelioma." Asbestos.com, 12 Feb 2026, https://www.asbestos.com/featured-stories/women-new-faces-mesothelioma/.
Mauney, Matt. "Women: The New Faces of Mesothelioma." Asbestos.com. Last modified February 12, 2026. https://www.asbestos.com/featured-stories/women-new-faces-mesothelioma/.

Matt Mauney is an award-winning journalist with more than a decade of professional writing and editing experience. He joined The Mesothelioma Center at Asbestos.com in 2016, and he spends much of his time reading, analyzing and reporting on mesothelioma research articles to ensure people in the mesothelioma community know the latest medical advances. Prior to joining Asbestos.com, Matt was a Community Manager at the Orlando Sentinel. Matt also edits pages, articles and other content on the website. He holds a certificate in health writing from the Centers for Disease Control and Prevention.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
