
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideLymphohistiocytoid mesothelioma is a rare subtype of asbestos cancer that makes up less than 1% of all asbestos-related cancer cases. Tumors are made up of a dense bundle of inflammatory immune cells, including lymphocytes (a type of white blood cell), plasma cells and immobile immune cells called histiocytes or macrophages.
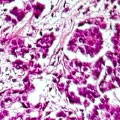
Lymphohistoicytoid mesothelioma is an aggressive sarcomatoid cell type. These tumors tend to have a mix of epithelioid cells and inflammatory cells. Some patients with this subtype may have an optimistic prognosis, like an epithelial cell diagnosis.
There are few reported cases of this subtype. Doctors often misdiagnose it as another condition, which is often non-Hodgkin’s lymphoma. Symptoms and treatment options mirror those of other pleural mesothelioma types.
Its rarity leaves researchers few opportunities to study it, and there is little information for review. Pathologists have identified specific tumor characteristics that can aid in an accurate diagnosis.
Facts About Lymphohistiocytoid Mesothelioma
First, surgeons take a sample of the tumor during a biopsy. Then, they send it to a lab for a pathological study. Many of the immune cells found in this subtype mimic other cancers. This can lead to misdiagnosis.
Under a microscope, histological studies reveal large, atypical polygonal to spindle-shaped histiocytoid cells. Mixed with these cells are white blood cells. Other signs of this tumor type include Diffuse pleural thickening, small nodules throughout the lining of the lung, and pleural effusion.
In immunohistochemistry, pathologists add antibodies to tumor tissue. These stain the tissue when there is a positive reaction. Each cancer has certain positive markers. Seeing them under a microscope can help make a more accurate diagnosis.
To prepare a sample, the pathologist fixes tumor tissue in a paraffin block. They then trim the block into thin slices and mount them on a slide. In studies, these tumor cells expressed cytokeratin, vimentin, calretinin and CH5/6. They were negative for lymphoid and macrophage markers. AE1/AE3 and calretinin antibodies are the most reliable for staining tissue samples.

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideThe symptoms of lymphohistoicytoid mesothelioma include chest pain, breathing problems, weight loss and fatigue. Symptoms of mesothelioma depend on the primary location of the tumors rather than the cell type. Symptoms of this type remain the same as other types of pleural mesothelioma.
If you’re experiencing symptoms, it’s important to consult with a specialist. For those with a history of asbestos exposure, discussing cancer screening with your doctor may help. Early detection can open up more treatment avenues, potentially offering better outcomes.
Treatment information is limited for this type because of its rarity. Doctors may recommend immunotherapy, chemotherapy and radiation therapy. In general, surgery may not be recommended because lymphohistoicytoid mesothelioma is considered part of the sarcomatoid cell type, which tends to recur quickly.
A 2007 study evaluated 22 cases. This study showed improvement and a positive response to treatment. Patients had extended life spans. Their survival ranged between 32 and 40 months after diagnosis. Early cases in a 1988 report showed no positive response to chemotherapy or radiation. The three patients in the report survived between four and eight months.
One encouraging case study showed a spontaneous regression of the tumor. Doctors removed tumors from the patient via surgery. The patients remained alive and without symptoms for 12 years after the initial presentation. In limited studies, some patients survived as much as six years after diagnosis. Doctors suggest that immune cells in this tumor may contribute to spontaneous regression.
Recommended ReadingYour web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, February 13). Lymphohistiocytoid Mesothelioma. Asbestos.com. Retrieved May 22, 2026, from https://www.asbestos.com/mesothelioma/lymphohistiocytoid/
Selby, Karen. "Lymphohistiocytoid Mesothelioma." Asbestos.com, 13 Feb 2026, https://www.asbestos.com/mesothelioma/lymphohistiocytoid/.
Selby, Karen. "Lymphohistiocytoid Mesothelioma." Asbestos.com. Last modified February 13, 2026. https://www.asbestos.com/mesothelioma/lymphohistiocytoid/.

Dr. Rupesh Kotecha is a renowned radiation oncologist in leadership roles at Miami Cancer Institute. He is an associate professor at Florida International University's college of medicine and an adjunct faculty member at Memorial Sloan Kettering.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
