
Discover financial assistance programs, insurance guidance, and veteran benefits to help cover your mesothelioma treatment expenses.
Get Financial HelpWritten by Sean Marchese | Edited by Walter Pacheco

Seniors are living longer and having to face more challenges than before. A healthy lifestyle can help you deal with aging, protect you from cancer and keep you at your best.
As average life expectancies increase, older adults are learning more about the cancers and other health risks that might affect them. In fact, age is the most significant risk factor for developing cancer.
People 65 and older comprise 60% of all cancer patients.
While age is the primary factor affecting your cancer or treatment, your physical lifestyle, treatment decisions and mental fitness determine your overall health.
As the senior population rapidly grows across the U.S. and around the world, researchers are developing new methods for treating the older population.
Cancers of the prostate, lung and colon represent half of all diagnosed malignancies among men 65 and older. Studies show prostate cancer is 22 times more likely in elderly men than in younger men.
Breast, colon, stomach and lung cancers are the most prevalent cancers affecting women 65 and older, making up nearly half of all malignancies in this population.
In younger age groups, cancers are almost evenly divided between men and women. However, in seniors, men have almost double the cancer incidence rate of women.
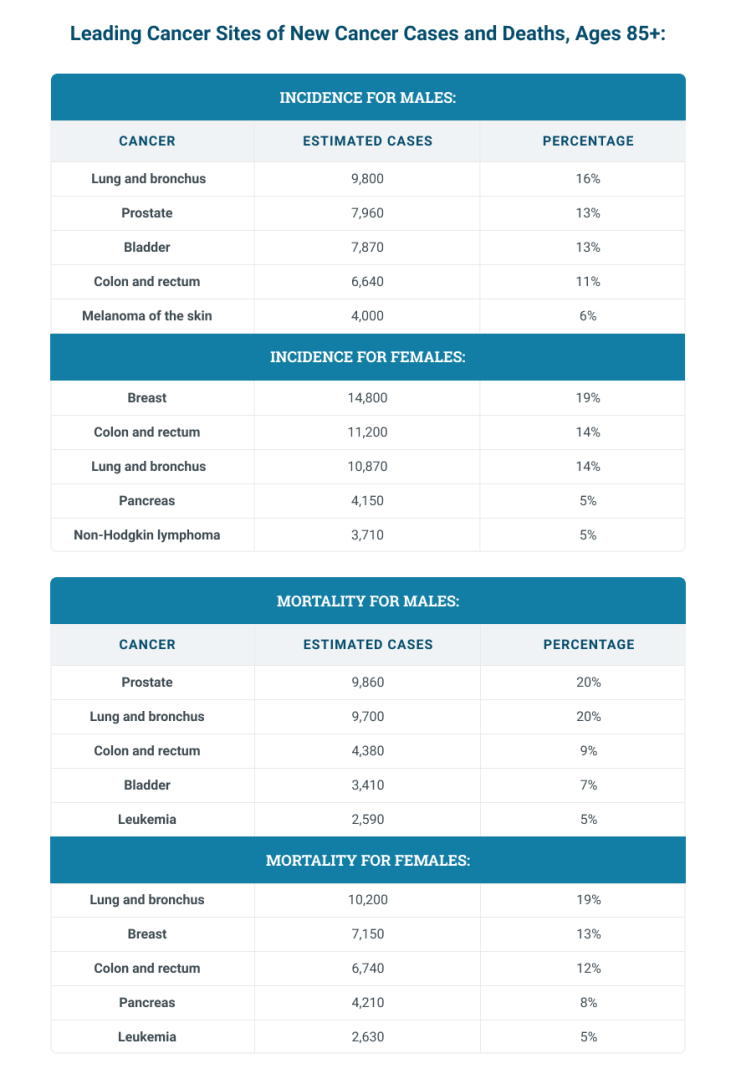
The top 10 cancers in older men and women are similar to those for all ages combined. Unfortunately, the cancer incidence and mortality rate have not declined in the senior population, highlighting the need for research into potential causes and future prevention.
It’s important to note the mortality rate for cancer among women, in general, is declining. Meanwhile, incidence rate is increasing more sharply than mortality among men. Simply put, the number of seniors living with cancer is projected to increase in coming years.
That’s why more cancer treatment research in the senior population is crucial.
Primary prevention remains the most valuable approach to decrease cancer incidence, and this is especially true for cancers caused by exposure to harmful substances.
Cancers with Exposure Risks

Many cancers caused by toxic substances can be avoided through certain changes in lifestyle.
Studies show the most effective behavioral changes include:
With certain cancers, however, prevention is more straightforward.
Limiting and ending the use of tobacco is an obvious way to stave off lung cancer and throat cancer but preventing exposure to other cancer-causing substances can be just as direct.
For example, malignant mesothelioma, a cancer that affects the linings of the chest and abdominal cavities, is caused by inhaling or ingesting asbestos fibers over long periods. Understanding your risk of asbestos exposure and knowing how to avoid the carcinogen can prevent mesothelioma as effectively as smoking cessation can lessen a lung cancer diagnosis.

Asbestos is found in construction materials such as roofing and flooring tiles. Prolonged inhalation and exposure to asbestos dust can cause pleural mesothelioma, peritoneal mesothelioma, lung cancer and asbestosis. Older blue-collar construction workers, contractors and veterans are at greatest risk for exposure to asbestos.

Arsenic is present in some herbicides, fungicides and contaminated water sources. This substance has been linked to lung, bladder and skin cancers. It has also caused occupational exposure risk in wood, glass and metal manufacturing industries.

Cadmium is present in batteries, solders and certain pigments and has been shown to cause prostate cancer. Nickel from ceramics, batteries and a byproduct of refineries can cause nose and lung cancer.
You should know the risks of your occupation or career and any potential carcinogens present in your home, school or workplace. Prevention is the best medicine and arming yourself with the knowledge to identify and avoid potential cancer-causing agents will improve your quality of life in later years.
There are unique challenges associated with treating cancer in the senior population. Chronic health conditions are more common in older adults and can incur complications during chemotherapy, surgery, radiation and other cancer therapies.
While the risks with these treatments can be higher, it does not mean you will have a shortage of options.
The decisions you make about your treatment will be based on your overall health, age and your emotional, mental and financial well-being.
The main therapies for treating cancer remain the same for all populations: Surgery, chemotherapy, radiation or multimodal therapies, which is a combination of treatments. As you consider your options, discuss with your oncologist any medical conditions you have that may put you at a higher risk.
Surgery can have major effects on organ function, and it is important to consider what the burden will be on your heart, lungs, liver and kidneys. Based on your medical history, surgery may cause or worsen irregular heartbeats, respiratory infections or blood toxicity from poor metabolism.
Chemotherapy is difficult for older adults for a variety of reasons. Most notably, it takes a long time. Doctors may provide you with frequent breaks in treatment or spread appointments out over a longer period.
Side effects of chemotherapy may be more pronounced in seniors than in younger patients. You may experience lower levels of blood cells leading to anemia or increased risk of infection. Chemotherapy can also cause dehydration, gastrointestinal issues and mental symptoms, also known as “chemo brain.”
Radiation therapy is generally considered a safer option for older adults and may be given alone or in combination with other treatments. Side effects will depend on the dosage of radiation and the location of the cancer. Radiation for bladder cancer can cause urinary side effects, while radiation treatment for lung cancer may result in chest pain.
Unfortunately, side effects are not the only concern when taking age into account for cancer treatment. Societal and social effects such as ageism cause hesitance in patients to disclose certain symptoms thinking “it’s natural with getting older,” or “just me getting old.”
These are dangerous and unnecessary thoughts that stress the importance of being treated by a doctor you can trust. Some doctors may overvalue age as a factor and rule out options such as surgery. A trusted oncologist can spend time getting to know you and your medical history.
Communication is key in establishing a fair and trusting doctor-patient relationship. A good doctor will listen to your concerns and ask questions to find the answers you need.
Some older patients may withhold information or concerns from their doctors because they’re embarrassed that those worries are associated with old age. This behavior is unsafe and can prevent your doctor from diagnosing an unknown condition.
It’s possible you may also need to see a specialist for your cancer. Some malignancies, such as mesothelioma and pancreatic cancer, are difficult to diagnose and treat. Having a strong relationship with your doctor can open the door to accessing the specialized treatments you need in critical early stages.
You can’t make an informed decision if you don’t have the information. Do the research, get a second opinion from a specialist and don’t be afraid to ask questions. That’s the only way to make the best choices with your health.Emily Warddiagnosed with pleural mesothelioma in 2012
Some treatments for cancer are still considered experimental and, in some cases, may provide better outcomes than other widely available therapies. These experimental medications and procedures are available only through sponsored clinical research trials.
While seniors remain the highest-risk population for developing cancer, many studies have shown that senior adults are largely underrepresented in clinical research trials.
One example reported patients age 65 and older made up 25% of the enrolled population for all active clinical trials. In contrast, this age group encompasses 63% of the U.S. cancer population.
Since 1983, the Food and Drug Administration has had guidelines and recommendations in place for not excluding older patients from clinical trials, so differences in treatment effects between age groups could be detected.
Notions of projected life expectancy or poor quality of life may dissuade physicians from recommending investigational treatments for many older patients. However, the need to advance new cancer treatments is paramount as the senior population continues to grow.
This puts the onus on patients to increase representation of seniors in clinical research trials.
Seniors have a right to take part in the advancement of medicine. The long-term effects of underrepresentation in clinical trials means less appropriate cancer treatments in the older population.
If you are not offered clinical trials from your oncologist, begin a discussion with them to determine what the obstacles might be and how you can overcome them.

Discover financial assistance programs, insurance guidance, and veteran benefits to help cover your mesothelioma treatment expenses.
Get Financial HelpAs your risk for health issues increases with age, preventive care also becomes more important. A 2022 report found that COVID-19 had a significant impact on cancer screenings for seniors. Screenings for all types of cancer fell sharply, especially in several underserved racial groups.
The U.S. Preventive Task Force, an expert federal panel, created guidelines to inform the public about needed vaccinations, screening tests and general health advice for preventing disease.
The following methods of disease prevention are especially important for older adults:

Influenza Vaccine: This vaccine is acquired yearly and helps prevent the flu. About 70% to 90% of deaths from influenza occur in patients 65 and older. Seniors undergoing cancer treatment should speak with their doctor to ensure they can receive the vaccine.
Pneumococcal Vaccine: The PPSV and the PCV13 vaccines help prevent pneumonia. For older adults, pneumonia can be a major life-threatening complication, especially in patients with cancer.

Annual Exams: Cancer screenings are one of the simplest and most affordable ways of preventing cancer. Inform your physician if you’ve been exposed to toxic substances such as asbestos or have a high incidence of cancer in your family.
Breast Cancer Screening: Over 40% of breast cancer cases are diagnosed in women 65 and older. Mammograms are recommended every two years for women between the ages of 50 and 74, but your doctor may recommend more frequent exams if you are at a higher risk due to genetic factors.
Colorectal Cancer Screening: Adults over the age of 70 make up over 60% of all new colorectal cancer cases. Recommendations for colorectal cancer screenings include various exams from fecal testing to colonoscopies performed yearly from ages 50 to 75.

Hypertension Screening: The risks and dangers of high blood pressure increase with age. Your physician will check your blood pressure levels every office visit and during your yearly wellness exam.
Diabetes Screening: Diabetes can lead to multiple complications and is common in older adults. One-fourth of people 65 and older are diagnosed with diabetes and the risk increases with obesity and genetic factors.
Cholesterol Screening: High cholesterol, called hypercholesterolemia, can lead to heart disease and stroke. Cholesterol levels in your blood should be checked during your yearly wellness exam starting at age 35.

Influenza Vaccine: This vaccine is acquired yearly and helps prevent the flu. About 70% to 90% of deaths from influenza occur in patients 65 and older. Seniors undergoing cancer treatment should speak with their doctor to ensure they can receive the vaccine.
Pneumococcal Vaccine: The PPSV and the PCV13 vaccines help prevent pneumonia. For older adults, pneumonia can be a major life-threatening complication, especially in patients with cancer.
Screenings and checkups are readily available and effective ways of preventing cancer and other life-threatening illnesses, even if you are checked only once per year. Caregivers can also make this process easier by scheduling appointments and arranging transport.
If you have difficulty making it to your doctor’s office due to health or transportation concerns, call your health care providers and ask what services are available for getting to the office. In many cases, they will contact your health insurance to establish assistance in making it to your visits.

A healthy lifestyle can provide a bounty of benefits that can’t be accomplished through regular visits to the doctor. General health and wellness have a profound impact on cancer prevention and can improve results and reduce side effects during cancer treatment.

Other general wellness habits are as simple as brushing your teeth twice daily for two minutes, taking vitamins as recommended by your physician, and cutting back on drinking or smoking.
Cancer treatments can affect your sense of smell and taste, making it difficult to ingest the proper amount of protein and carbohydrates needed to prevent weight loss. Vitamins and minerals prescribed by your doctor can offset some of these issues but altering eating habits will have a larger impact.
There are difficulties maintaining proper nutrition in later years. Changes in sense of smell or taste might alter eating habits. Gum disease and mouth infections are more prevalent with denture usage.
For adults 65 and older, the Centers for Disease Control and Prevention recommend engaging in 150 minutes of moderate-intensity activity (such as a brisk walk) or 75 minutes of vigorous-intensity aerobics (such as running in place) every week.
If you are unfamiliar with a workout routine for your level of health, talk with your doctor about what exercises would be appropriate for you.
These activities can improve mobility and endurance, allowing you to spend more time doing what you enjoy most.

Changes to muscle strength, balance and flexibility can significantly improve quality of life. Find simple routines where you have strong support and start with small weights. Beginner yoga routines primarily involve stretching movements.
The next time you’re carrying groceries, maneuvering an awkward corner or reaching for objects high in the kitchen, you’ll be glad you started exercising.
New research suggests seniors require just as much sleep as other adults. However, getting 7 to 9 hours of sleep every night can be more difficult as you age. Insomnia and exhaustion take a toll on the body and impact health in significant ways.
Senior brains actually have different physiology that alters patterns in falling asleep and maintaining sleep. Fortunately, options exist that range from creating healthy habits to products designed for seniors that ensure your health isn’t impacted by a lack of sleep.
Following a consistent sleep schedule is one of the easiest and best ways to improve your sleep hygiene. Set a time to go to sleep and wake up every day and stick to it without exception, even on weekends.

Daily exercise and exposure to sunlight can improve restfulness at night, making it easier to fall asleep and stay asleep. Avoid napping during the day and keep the bedroom conditions ideal for how you prefer to sleep.
Consider developing a bedtime routine that involves a warm bath or shower, reading a book or knitting. Avoid drinking water right before bed to avoid having to use the bathroom. With dedication and time, developing new sleep habits will improve your health and your quality of life.
Getting older brings about many emotional challenges. Relationships dissolve or change, retirement and financial concerns arise, and medical problems become more frequent. You may feel sad, uncertain or stressed about these changes, and it may be difficult to recover.
Depression is common among older adults, but it should not be considered normal. There are many symptoms of depression, some less obvious than others, that make diagnosis difficult.
If these symptoms are common for you and have persisted for several weeks, consult your physician about depression. Starting treatment may be required for you to get back to an active lifestyle and healthy routines.
Sometimes long episodes of grief after the passing of a loved one can mimic depression. Whether or not treatment is right for you will depend on how much your daily activity is affected. It’s always important to talk to your doctor if you think something is wrong with your emotional health.
There are many resources you can take advantage of to improve your emotional well-being.
Connect with friends and family through phone calls and video chat. Isolation can be harmful to older adults and with today’s technology there is no reason for it.
You may find purpose and enrichment through volunteering at your local church or hospital. These opportunities can bring joy to you and the people you serve and allow you to build relationships with many new people.

Support groups are available in person and online. Many older adults with cancer and other chronic illness use support groups to connect with other patients who share their medical journey and support one another. Your physician or health care center can provide you with a list of resources for finding a support group relevant to your condition.
An important component of brain health and overall well-being involves maintaining cognitive function. Cognition refers to your ability to think clearly, learn new concepts and remember pieces of information.
Getting older requires maintaining the health of the neurons in your brain like you would keeping an older car tuned up with oil changes.
Keeping your mind active and intellectually engaged improves your thinking ability and prevents deterioration of memory. One study found that older adults who learned a new hobby, such as digital photography or quilting, had better memory retention than those who only socialized for engagement.
Social activities and community programs also contribute to cognitive health and can help you feel less isolated. Visit with friends and family or participate in activities at a senior center.
Multiple factors influence cognitive health such as genetics, environment and lifestyle choices. As cognitive function declines, it can affect your ability to drive, cook or even take your daily medication.
Alcohol intake, falls and car accidents can cause brain injury and severely damage cognitive function. Educate yourself on fall-prevention strategies and always wear a seatbelt when driving. Protecting your brain is key to maximizing your wellness and maintaining overall health.

Between nursing homes and at-home care, senior caregiving can take many forms. The answer that is best for your situation will depend on not only what type of care is needed but also insurance eligibility and availability of senior housing.
Many tools and resources exist to help you find the solution that’s right for you. Several retirement homes and at-home care sites will work with you to figure out what’s best for your situation and your loved ones.
At-home care provides someone who cares for a senior care in their own home and assists them with activities of daily living, household tasks or errands. Assisted living provides similar benefits but in a location that caters to several other older adults.
Seniors who would feel more comfortable in their own home and can remain mostly independent benefit from at-home care. Alternatively, assisted living is a suitable option for households unable to provide a caregiver or need additional services.
The most appropriate professionals for providing care to you in your home are often health aides and certified nurse assistants or CNAs.
These workers provide basic medical care such as monitoring vital signs, assisting with medication and treating wounds. More advanced medical services are offered by registered nurses or RNs.
Following a set of guidelines as you look for a home care worker will help you make the right choice.
When choosing a retirement community, be prepared with a list of questions. Gather research beforehand and know what type of care will be required.
Senior living communities have several advantages over other retirement options, such as:
The most important facet of senior living that a facility can provide to its residents is ensuring safety and quality of care. Retirement facilities should have policies and regulations provided for residents to review and question at any time.
When you’ve narrowed down your choices, visit each facility in person to speak with managers, staff and other residents.
Make sure you get answers to all your questions and discuss them with your family before making a decision. Ask the facility about their policies on issues such as elder abuse and neglect. Reputable facilities will detail their policies to prevent these issues and provide you with peace of mind.

The AARP reports that over 34 million Americans provide unpaid care to adults age 50 or older every year. Informal caregivers make up a significant percentage of how seniors are receiving care at home. These caregivers might be family members, companions or longtime friends who provide personal support or medical care.
In some cases, remote caregiving is an option to providing companionship or counseling through phone calls and video calls. Long-distance caregivers are also able to manage recurring services such as delivery and medical appointments.
Caregivers support seniors through a great deal of responsibilities such as housecleaning, personal hygiene, basic medical care and companionship. Aging-related advance planning is also made significant easier with the help of a caregiver.
In 2015, the National Alliance for Caregiving reported that unpaid caregivers spent an average of 25 hours per week providing care. The study also reported 41% of caregivers worked unpaid for 41 or more hours per week.
Since 1993, the Family and Medical Leave Act allows a person to take 12 weeks off work to provide caregiving (26 weeks if providing care to a veteran). Unfortunately, many caregivers cannot afford to go 12 weeks without income, and paid family leave is becoming a more common option.
Several states have paid family leave or wage replacement laws in effect, but the degree of eligibility and compensation varies widely.
Caregivers may need help to cope with taking on such a demanding role. Respite care services are available through Medicaid, home care agencies and many community organizations. These services can relieve you of caregiving duties several times per week often for low cost or free.
Staying organized and documenting the caregiving process will help alleviate stress and allow you to prepare a schedule of events. Keep an organizer with appointments, contact numbers and medical notes. Journaling your own experiences and emotions may help you identify any major obstacles in caregiving.
Most importantly, remember care for yourself. Caregiving is emotional and, at times, overwhelming. Join a caregiver support group or establish a regular exercise and meditation routine that allows you time to step away from your duties.
While it may be disparaging to consider the end of your care, planning for the future will ensure your medical and personal wishes are carried out. As you become more familiar with your medical condition, you’ll also be able to decide how best to improve your quality of life.
Discussing your end-of-life choices with your family can relieve anxiety and fear of the unknown. Your family will also better understand how you’re feeling and why those choices are important to you.
Depending on your medical condition, you may choose to focus on symptom management rather than curative treatments. Consult with your physician if palliative care would improve your quality of life and achieve a satisfactory level of comfort.
You should also discuss with your family where you’d like to receive care. Some patients prefer constant medical attention in the hospital, while others would feel more comfortable at home with loved ones for support.
It’s possible you may be uncomfortable with certain medical support equipment or techniques for end-of-life care such as a ventilator, respirator or feeding tube. Discuss with your family and medical team which forms of life support are acceptable to you and include them in your advance directive.
In case a patient is unable to completely plan their end-of-life care and wishes, a durable power of attorney for health care can be appointed. This is a friend or family member you trust implicitly to make medical decisions, on your behalf, that you believe would be aligned with your best interests.
Similarly, a durable power of attorney for financial affairs has the ability to make decisions about your estate in the event a will is incomplete, invalid or challenged.
Consider your options and the choices that would provide the most fulfillment. There is always support available, and no one ever has to face these decisions alone.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Marchese, S. (2026, February 9). Seniors Guide to Cancer. Asbestos.com. Retrieved June 1, 2026, from https://www.asbestos.com/cancer/senior-cancer-guide/
Marchese, Sean. "Seniors Guide to Cancer." Asbestos.com, 9 Feb 2026, https://www.asbestos.com/cancer/senior-cancer-guide/.
Marchese, Sean. "Seniors Guide to Cancer." Asbestos.com. Last modified February 9, 2026. https://www.asbestos.com/cancer/senior-cancer-guide/.

Sean Marchese is a registered nurse with experience developing and managing respiratory oncology clinical trials and treatments. He has more than 10 years of clinical experience as a nurse in pain management, neurosurgery and clinical trials.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
