
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideAsbestos exposure doesn’t cause immediate symptoms. Signs of exposure often appear years later. They may point to early asbestos-related conditions like asbestosis, lung cancer and mesothelioma. It's crucial to spot these early signs. They can help you seek timely medical care and improve long-term health.
Early signs of asbestos exposure include shortness of breath, a constant cough and chest pain. These signs are often mistaken for common respiratory issues, delaying diagnosis. Watch for early asbestos exposure signs, which can take decades to develop, if you’ve handled asbestos. Monitoring for early signs can mean diagnosing asbestos-related diseases such as mesothelioma sooner.
Most Common Symptoms
These early symptoms overlap with other more common health issues like flu or pneumonia. But if you experienced prolonged asbestos exposure, it could lead to serious conditions like pleural mesothelioma or lung cancer. Speaking to your doctor as soon as possible about a history of working in high-risk areas or occupations can also allow your doctor to arrange regular screenings for you for asbestos-related cancers.
Symptoms vary depending on the asbestos-related disease. Asbestos exposure most often causes conditions that affect the respiratory system. Some fibers travel through the bloodstream, where they may damage other parts of the body.
The first signs of asbestos-related disease are usually shortness of breath during light physical activity and a persistent dry cough. These symptoms often appear 10 to 50 years after initial exposure, long after the original asbestos contact.
Symptoms by Type of Disease
Symptoms often overlap with those of other diseases, contributing to misdiagnosis. For example, pleural mesothelioma symptoms can resemble COPD. Peritoneal mesothelioma shares symptoms like fluid buildup, called ascites, and belly pain with conditions like pancreatitis. These overlaps can delay proper diagnosis, while early detection improves outcomes.
Peritoneal mesothelioma survivor Epifanio Figueroa tells us that his first symptom was abdominal swelling. The swelling led him to a hospital visit where he says, “They told us they weren’t sure.” At a second hospital, a biopsy confirmed his asbestos-related disease in 2016. Epifanio shares that at the time of his diagnosis, “I didn’t know that mesothelioma existed.”

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideAsbestos fibers can remain in the body for decades, causing chronic inflammation. Inhaled fibers lodge in the tissue that lines the lungs (pleura), where they can cause damage over time. The long latency period of 20 to 60 years means symptoms may not appear until the disease advances.
Effects of Asbestos Exposure
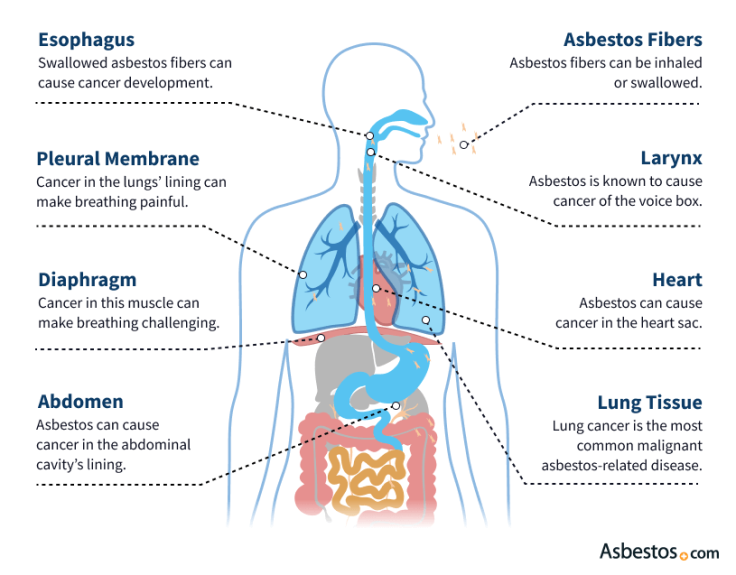
Inhaling asbestos fibers is the primary cause of mesothelioma. Ingesting asbestos may cause peritoneal mesothelioma. Asbestos can also cause diseases in other body parts. Signs of these conditions primarily arise in the throat, stomach, colon or pelvic region.
The time from when asbestos-related diseases and their symptoms develop, or the latency period, can range from 10 to 60 years. Asbestosis usually develops within 10 to 30 years, while mesothelioma can take 20 to 60 years.
Latency Periods of Asbestos-Diseases
The delay can make it hard initially for people to associate their current health issues to their past asbestos exposure. Health care providers might not ask about asbestos exposure that happened long ago. This can contribute to misdiagnosis. This long delay happens because inhaled asbestos fibers stay lodged in lung or abdominal tissue for decades, slowly triggering inflammation and cellular changes that only produce measurable symptoms once enough scarring or tumor growth has built up. Learn more about short-term asbestos exposure.

Carla Fasolo
Symptoms Started Decades After Asbestos Exposure
“It started with me going down to the Oneida County Courthouse in Utica, New York, with my dad,” she told The Mesothelioma Center. “I would go down there with him, and it was very dusty in the boiler room. There would be chunks of gray, fibrous stuff down there. I didn’t know what it was, but I’d pick it up and play with it.”
Carla Fasolo
If you have a history of asbestos exposure and start showing any signs or symptoms, it’s important to see a doctor right away. Don’t wait, even if your symptoms don’t seem severe. Consulting a doctor early can lead to better treatment options and improve your chances of a positive outcome.

There isn’t a single test that confirms past asbestos exposure, but doctors use 4 standard tools to detect changes asbestos fibers can cause in the body: chest X-rays, low-dose CT scans, pulmonary function tests and spirometry. These tests are typically ordered when a person with known exposure history begins to develop respiratory symptoms.
Standard Diagnostic Tools
Routine screening can play a key role in finding asbestos-related illnesses early. This is especially important for people with a strong history of asbestos exposure.
Some tests can find asbestos fibers in lung tissue, lung fluid, stool, mucus or urine. However, no current test can detect asbestos fibers in the blood. These tools help monitor lung health and identify problems before they become serious.
Prolonged or repeated asbestos exposure increases the likelihood of developing asbestos-related diseases. Those who work in construction, shipbuilding or manufacturing are at the highest risk. This is especially true if they were exposed before safety regulations.
In most cases, asbestos exposure doesn’t cause immediate symptoms. Instead, diseases linked to asbestos develop over time, with symptoms appearing decades later. But exposure to high levels of asbestos fibers can irritate the lungs. It can cause temporary symptoms like coughing and difficulty breathing.
Tests, like low-dose CT scans, can find early signs of asbestos diseases in exposed people. These tests can’t confirm asbestos fibers. They can find lung or pleura issues. These may suggest an asbestos-related condition.
Asbestos-related diseases usually affect older people. There is a long gap between exposure and symptoms. But those exposed to asbestos at a young age may face severe health issues later in life. Asbestos fibers may harm developing lungs. This raises the risk of mesothelioma and lung cancer in adults.
Most sick people worked with asbestos for most of their careers. Illness risk rises with longer asbestos exposure and higher fiber levels. Smoking and asbestos exposure together greatly raise lung cancer risk, but not mesothelioma.
The first signs of asbestos poisoning are shortness of breath during physical activity and a persistent dry cough. As asbestos-related disease progresses, patients may also notice chest tightness, crackling sounds in the lungs when inhaling, unexplained weight loss and fatigue. Because these early symptoms resemble bronchitis or seasonal allergies, many people don’t connect them to past asbestos exposure for years. Anyone with a known exposure history who develops these symptoms should share that history with their doctor.
People with known or suspected asbestos exposure should discuss screening with their doctor, especially those who worked in construction, shipbuilding, manufacturing, asbestos mining, automotive repair or military occupations before the late 1980s. Family members of asbestos workers and people who lived near asbestos mines or factories are also candidates for screening, even without current respiratory symptoms.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2026, May 7). Signs of Asbestos Exposure. Retrieved June 4, 2026, from https://www.asbestos.com/exposure/signs/
"Signs of Asbestos Exposure." Asbestos.com, 7 May 2026, https://www.asbestos.com/exposure/signs/.
Asbestos.com. "Signs of Asbestos Exposure." Last modified May 7, 2026. https://www.asbestos.com/exposure/signs/.

Dr. Andrea Wolf is the Director of the New York Mesothelioma Program at Mount Sinai in New York City. She focuses on multidisciplinary treatment, clinical research, community outreach and education.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
