
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideInterstitial lung disease causes inflammation and scarring. Asbestos exposure, some diseases and medications can cause it. There is a clear link between asbestos exposure and asbestosis or interstitial pneumonitis, a form of ILD.
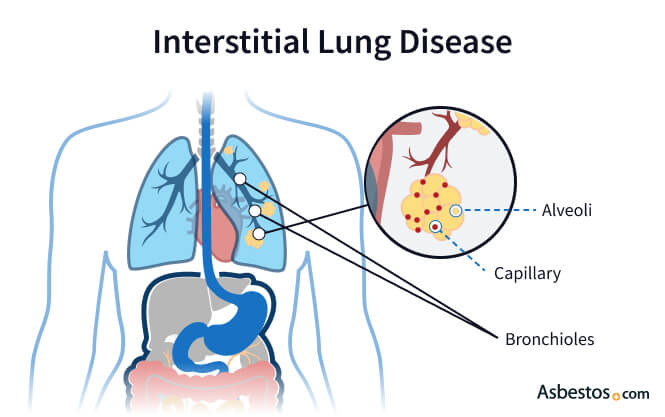
Interstitial lung disease is an umbrella term for approximately 200 relatively rare lung diseases that cause lung inflammation or scarring. Some ILD types only cause scarring (fibrosis). And some only cause inflammation while others cause both.
Key Facts About Interstitial Lung Disease
If you have inflammation without scarring, early treatment may prevent scarring from developing. Inflammation and scarring affect the interstitial lining that supports your lung’s alveoli. Your interstitium is a thin, mesh-like network of tissue that surrounds and supports the tiny air sacs in your lungs. When this tissue becomes thickened or scarred, it makes it harder for oxygen to pass into the bloodstream.
Asbestosis is an ILD linked to asbestos exposure. As the body tries to expel inhaled asbestos fibers, inflammation and scarring occurs. It’s a progressive disease that continues to worsen over time.
Doctors usually group ILDs into broad categories according to their cause. These categories include exposure to irritants, some types of medical treatment, autoimmune disorders and smoking.
The causes of some ILD cases can’t easily be identified. These are often called idiopathic pulmonary fibrosis. Idiopathic means the disease was spontaneous or the cause is unknown.
Types of ILDs
Autoimmune disorders contributing to ILD include lupus, polymyositis or dermatomyositis, rheumatoid arthritis and scleroderma. Risks include exposure to asbestos, silica dust and cotton dust. Some medical treatments may cause lung inflammation and scarring. These treatments include chemotherapy, radiation and certain medicines.

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideMany of the different forms of ILD display similar symptoms associated with decreased lung function. They usually appear after scarring develops. This means that irreversible damage has occurred.
Symptoms of asbestosis can easily be mistaken for signs of other lung conditions such as COPD or asthma. Many ILD symptoms worsen with exertion.
Interstitial Lung Disease Symptoms
Latency periods vary among the types of interstitial lung disease. Symptoms can take months to years to appear, depending on the disease. Some ILDs have a long latency period, so symptoms may not appear right away. Others advance more rapidly.
It can take 20 to 30 years for asbestosis symptoms to develop. Some people have no symptoms at all. Many people don’t know they have the condition until lung damage becomes significant many years after exposure.
People with ILD can suffer from serious complications. Many ILD complications result from decreased lung function and its impact on the body. They include fluid and calcium buildup in the lung lining, high blood pressure in the lungs and a higher risk of infection and some cancers.
Interstitial Lung Disease Complications
Lung cancer is a big concern for asbestosis patients who smoke. Quitting smoking can lower your cancer risk and boost lung function.
Additionally, acute exacerbation is a severe concern. This sudden worsening of respiratory symptoms affects a large number of patients with ILD and can occur at any time. For many patients, it can be what ultimately leads to a diagnosis.

Jerry Cochran
Navy Veteran With Asbestosis & Silicosis Has a Passion for Justice
Navy veteran Jerry Cochran was diagnosed 50 years ago with sarcoidosis. The more he read about it, the more concerned he was that his symptoms just didn’t match up. In 1991, he was given a new diagnosis – silicosis – from inhaling silica dust while scraping paint on the USS Independence. He was also later diagnosed with asbestosis, an asbestos-related interstitial lung disease.
Jerry Cochran
Doctors diagnose interstitial lung diseases using chest X-rays, CT scans and lung function tests. Because ILDs share symptoms with other lung problems, diagnosis can be challenging. Detailed testing helps rule out other conditions, allowing doctors to make an accurate diagnosis.
Sometimes, a lung biopsy is needed. Tissue samples show lung health and may uncover other issues like cancer. Doctors collect these samples through procedures such as bronchoscopy, lavage or biopsy.
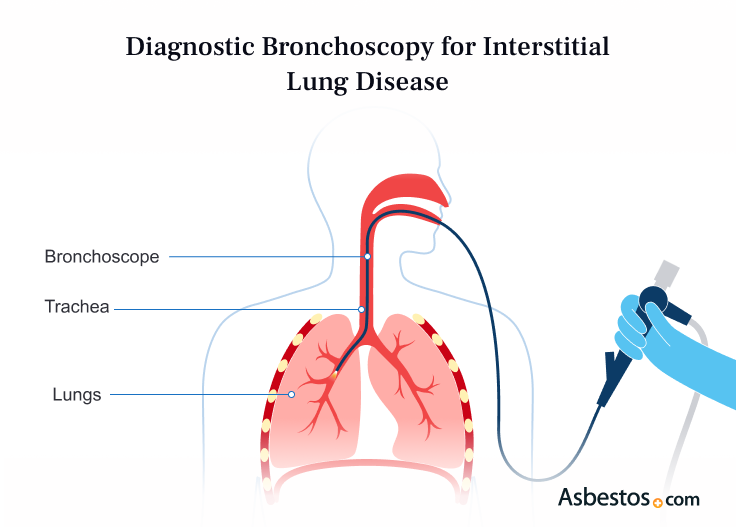
Treatment for ILD and asbestosis focuses on easing symptoms, managing complications and slowing lung scarring. Oxygen therapy can reduce shortness of breath associated with lung damage. Other medications include corticosteroids, anti-fibrotic agents and tyrosine kinase inhibitors, which may relieve symptoms and slow disease progression.
More advanced treatments include removing fluid from the lungs and respiratory therapy. Respiratory therapists teach breathing exercises to help people improve lung function. In rare cases, a lung transplant may be necessary, though it’s not a common treatment for asbestosis.
ILD & Asbestosis Treatment Options
The outlook after an ILD diagnosis varies widely depending on the specific disease. Overall health and lifestyle factors, like smoking, affect how the disease progresses. Smokers exposed to asbestos have a high risk of developing ILD.
For asbestosis, the prognosis often depends on the length and severity of asbestos exposure. Many individuals live full lives for years following their diagnosis.
Recommended ReadingYour web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2026, February 13). Interstitial Lung Disease & Asbestos. Retrieved June 1, 2026, from https://www.asbestos.com/mesothelioma/interstitial-lung-disease/
"Interstitial Lung Disease & Asbestos." Asbestos.com, 13 Feb 2026, https://www.asbestos.com/mesothelioma/interstitial-lung-disease/.
Asbestos.com. "Interstitial Lung Disease & Asbestos." Last modified February 13, 2026. https://www.asbestos.com/mesothelioma/interstitial-lung-disease/.

Dr. Rupesh Kotecha is a renowned radiation oncologist in leadership roles at Miami Cancer Institute. He is an associate professor at Florida International University's college of medicine and an adjunct faculty member at Memorial Sloan Kettering.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
