Experts Discuss Unique Side Effects of Immunotherapy
Treatment & DoctorsWritten by Suzanne Dixon, MPH, MS, RDN | Edited by Walter Pacheco
If you have mesothelioma and you’ve already received standard-of-care therapies, you may be considering an immunotherapy clinical trial.
If you’re considering this option, a free immunotherapy teleconference is a great place to learn more.
CancerCare recently hosted two one-hour education workshops featuring panels of immunotherapy experts. Part I of the teleconference presented an overview of immunotherapy.
Part II of the teleconference, which is available online for free, focused exclusively on immunotherapy side effects.
Understanding these issues and the role each patient plays in managing their own side effects is critical to successful clinical trial participation.
Side Effects: Immunotherapy Vs. Chemotherapy
Dr. Susan Slovin, panelist and attending physician of genitourinary oncology at Memorial Sloan Kettering Cancer Center (MSK), explained the basics of chemotherapy and immunotherapy side effects.
“Chemotherapy gets at the DNA, or the reproductive site, of cancer cells. It also affects normal cell function and reproduction. These actions on normal cells drive general side effects like nausea and fatigue,” Slovin explained.
Immunotherapy’s mechanism of action is very different, so the side effect profile is different as well.
Unlike chemotherapy, immunotherapy does not destroy cancer directly. The goal of immunotherapy is to manipulate the immune system to kill cancer without destroying normal tissue.
“With normal immunity, our bodies produce substances to keep the immune system from attacking healthy tissue,” Slovin said. “These substances can prevent immunity against cancer, too. If we can block these substances, we can activate the immune system against the cancer.”
However, if we remove the brakes on immune function so it can attack cancer, it may attack healthy cells, too. This is why side effects resemble immune reactions rather than the general cell damage seen with chemotherapy.
“We are swapping excellent control of cancer for side effects normally under good control by regular immune function,” Slovin explained.
Slovin said the key to successful treatment, while managing side effects, is early recognition of anything out of the ordinary.
“It is critical to have constant communication with your health care team. Minor symptoms can be addressed before skyrocketing into something more serious. This leads to excellent treatment with manageable side effects,” Slovin said.
Side Effects Common but Manageable
“All immunotherapy side effects are caused by generalized overactivation of the immune system and are not specific to the cancer,” said panelist and medical oncologist Dr. Alan Bryce of the Mayo Clinic in Phoenix, Arizona.
Around 70-80 percent of patients receiving checkpoint inhibitors, which are common immunotherapy drugs, experience side effects. The immune system can attack almost any organ system, leading to side effects in any part of the body.
“Side effects are, for the most part, mild and manageable, and the drugs are well tolerated,” Bryce said. “In fact, immunotherapy drugs often are better tolerated than chemotherapy and can be more easily used in frail and elderly patients.”
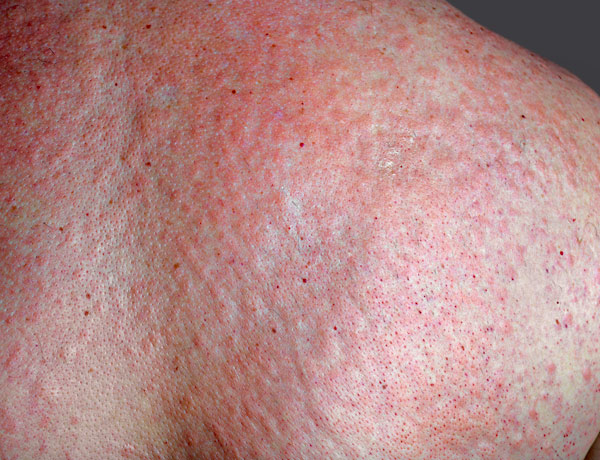
The most common side effect is a skin rash of red, raised, itchy bumps first appearing on the trunk. This is usually managed with a prescription steroid cream.
“If the rash continues to spread, a dermatologist will take a skin biopsy to rule out other, treatable causes of skin issues,” Bryce explained.
Mild cough and shortness of breath can occur but typically are not severe. If they become severe, the physician will “turn down” the immune system.
“Immunotherapy dials things up to 11. With severe side effects, we dial it back down to five or six, usually with an immunosuppressant drug,” Bryce noted. “The last thing we want is a patient needing oxygen or being hospitalized.”
One worrisome immunotherapy side effect is colitis, or inflammation of the bowel. Changes in bowel habits are always taken seriously and evaluated thoroughly to determine the cause.
“I strongly emphasize the need to be in close, almost daily contact, with your physicians,” Bryce said. This follows Slovin’s advice on the importance of regular communication with your health care team.
“I don’t want a patient to ‘tough it out’ with four or five days of diarrhea,” Bryce said. “In early clinical trials, a few patients died due to severe diarrhea because the symptoms persisted for so long before the physician was alerted, which should almost never happen with modern therapy.”
Any organ system can become inflamed, so autoimmune-like diseases, similar to rheumatoid arthritis, lupus and psoriasis, can occur. Fevers, a general sign of inflammation, tend to be minor and manageable with Tylenol or ibuprofen.
Nearly all of these symptoms are reversible, with the exception of hormone-system side effects.
Hormone abnormalities called endocrinopathies tend to be permanent. Any gland, such as the pituitary, thyroid and adrenal glands, can be affected. In these cases, the patient needs life-long therapy to manage the issue.
“We expect autoimmune-like side effects. If someone has an underlying autoimmune condition, they can receive immunotherapy. Symptoms will flare up when we begin treatment, but this can be managed,” Bryce said.
Fatigue and Diarrhea Must Be Addressed
Dr. Stewart Fleishman, a panelist, oncology researcher and former founding director of cancer supportive services for Continuum Cancer Centers, addressed immunotherapy-related fatigue and diarrhea.
“Fatigue is a common side effect but can be much more severe and harder to get through than many side effects. It’s not a matter of mental toughness. You want to do things, but your body simply cannot follow through,” Fleishman said.
There are many reversible causes of fatigue such as anemia, kidney or liver problems, adrenal or thyroid gland issues, new onset diabetes or other metabolic problems. Letting your doctor and nurse know about fatigue will help them help you.
Once reversible causes are addressed or ruled out, Fleishman urges a focus on the “four pillars” of managing fatigue.
“Take a practical look at good nutrition, activity and movement, rest and sleep. These four pillars need to be in balance to have the most energy possible, and more energy equals less fatigue,” Fleishman explained.
For sleep, make sure you have a quiet, cool, dark, undisturbed bedroom, a good mattress, a comfortable pillow and as many regular sleep hours as possible.
Activity may seem counterintuitive because it can make you more tired in the short run. But it improves appetite, which can help with good nutrition. It also improves our ability to rest when needed and get good sleep each night.
“The other thing that can impact fatigue is diarrhea because it can account for a significant loss of fluids and important salts called electrolytes. Sodium and potassium are key salts, and loss of potassium can lead to severe fatigue,” Fleishman said.
As explained by other panelists, colitis is a serious concern, and you need to give accurate estimates to your doctor regarding the number of bowel movements per day. If colitis is suspected, you may need a scope of your lower GI tract to confirm this.
“Mild diarrhea is defined as less than four bowel movements per day, while moderate is seven or fewer. If diarrhea is moving from mild to severe, getting a scope to determine the cause is very important for your care,” Fleishman advised.
To manage diarrhea, Fleishman suggested:
-
Taking a fiber supplement with much less water than typical to allow the fiber to absorb extra fluid and minimize diarrhea.
-
Ruling out other causes such as food poisoning.
-
Replacing fluids and electrolytes with products designed to address diarrhea.
-
Considering anti-diarrheal drugs, such as tincture of opium, for severe diarrhea.
-
Discussing anti-inflammatory medications, such as sulfasalazine, with your doctor.
Skin Precautions Are a Must
Dr. Mario Lacouture, panelist and director of oncodermatology at MSK, focused on the importance of understanding and managing common immunotherapy-related skin reactions.
“Dermatologic side effects are common and often the first manifestation of immunotherapy side effects. About 40-60 percent of patients treated will be affected with a skin rash or similar skin issue,” Lacouture explained.
Rashes often start on the trunk and back and can be very itchy. Fortunately, they tend to be benign in most cases. Doctors follow rashes closely, because if they extend to the rest of the body, this can interrupt immunotherapy.
In addition to rashes, some people lose normal skin color in patches. This is not dangerous but can be very distressing to patients. “Skin side effects seem to be associated with a better response to immunotherapy,” Lacouture said. “This may help patients find some acceptance of these changes.”
As noted by other panelists, the majority of skin reactions are treated with topical, prescription steroid creams, and occasionally oral medications that suppress the immune system.
“Itching can be very intense and in some cases severely compromise quality of life. Drugs used for chronic pain, such as gabapentin and pregabalin, seem to be very effective for managing itching,” Lacouture advised.
While uncommon, hair loss can occur and is difficult to treat. Lacouture recommends consulting a dermatologist familiar with immunotherapies because new management options for hair loss are emerging.
Consistent skin care is critical with immunotherapy, too. This includes:
-
Avoiding scented detergents and soaps
-
Protecting against sunburn by minimizing time outdoors between 10 a.m. and 4 p.m.
-
Using sunscreen with a minimum SPF of 30, and reapplying every two hours, or every hour if sweating or swimming
-
Wearing sun protective clothing and gear (broad brimmed hat, long sleeves, large sunglasses)
“Skin issues often are the first side effects to occur with immunotherapy, but these effects mean the therapy is working. On the other hand, if you don’t have skin issues, don’t assume your treatment isn’t working,” Lacoutoure said.
Food Is Good Medicine
Diana Bearden, panelist and dietitian at the Michael E. DeBakey VA Medical Center stressed nutrition and hydration are key components of good immunotherapy outcomes.
Side effects can be worsened if nutrition is poor or inadequate to meet needs.
“Protein is a key building block for healing. Also focus on calories. If you don’t have enough calories to meet needs, you can burn protein for energy, leading to depletion of healthy tissues,” Bearden explained.
A plant-based diet, with vegetables, fruit, whole grains and beans covering two-thirds of the plate, is ideal for cancer prevention and survivorship. These foods provide antioxidants and phytochemicals.
“Focus on lean protein for the other third of your plate. Include wild caught fish such as salmon, tuna, halibut and sardines, plus poultry or beans,” Bearden advised.
For fluids to address dehydration, make sure you use one designed to meet the needs of someone with diarrhea. It should contain sodium and potassium to replenish lost electrolytes.
If you have trouble meeting nutrition needs, keep a daily record of what you’re eating. A dietitian on your team can help you determine what foods might be aggravating a symptom or side affect and make suggestions to fix that problem.
As with all other team members, regular communication, in this case with a registered dietitian, is the best way to address issues before they become serious.