
Connect with top-rated mesothelioma specialists at a cancer center near you, who will personalize treatment options based on your diagnosis.
Find Your CenterMesothelioma imaging scans include X-rays, CT scans, MRIs and PET scans. They're a key part of diagnosing this rare cancer. Imaging scans for mesothelioma let doctors see if the cancer has spread.
Mesothelioma imaging scans help doctors spot tumors, fluid and scarring that point to cancer. Because early mesothelioma can be hard to see and symptoms overlap with other diseases, scans are often the first step to confirm a concern and decide what test should come next.
Imaging Scans for Diagnosing Mesothelioma
These tools work best together. Your specialist will choose the right scan based on where your symptoms are, your exposure history and what the care team needs to decide next.
Carla Fasolo first noticed mild back pain that quickly escalated to severe discomfort. An emergency X-ray revealed a large tumor in her chest, followed by a CT scan and biopsy that confirmed mesothelioma. Carla’s experience shows how imaging and pathology work together to detect mesothelioma early and guide treatment decisions.
Mesothelioma radiology adds expert eyes to complex pictures. Radiologists trained in asbestos diseases can catch subtle signs, rule out look-alike problems such as pneumonia, and flag the safest spot for a biopsy. Their reports guide staging and treatment plans, and they partner closely with surgeons, medical oncologists and pulmonologists throughout care.
Imaging scans are also used for mesothelioma staging. Accurate staging requires determining the tumor’s size and location, whether lymph nodes are involved and if cancer cells have spread to other parts of the body.
X-rays are mesothelioma imaging scans that offer a fast, low-dose way to look for problems in the chest. Doctors use them to spot fluid around the lungs, areas of unusual thickening or a collapsed lung that may signal pleural disease.
How X-Ray Scans Work
Doctors check for warning signs linked to mesothelioma, like pleural effusion, pleural thickening, or a partly collapsed lung. X-rays can miss small or early tumors, and they do not diagnose cancer alone. If your X-ray raises concern, your doctor will order advanced scans and, if needed, a biopsy to be sure.
Michael Cole, a survivor of pleural mesothelioma, shares his X-ray story with us. A cough and lack of energy sent him to his doctor. Michael says, “They listened to my chest, took an X-ray and told me to go straight to the hospital. They quickly drained 2 liters of foul-looking fluid out of my right lung.” He was diagnosed with mesothelioma 4 days later.
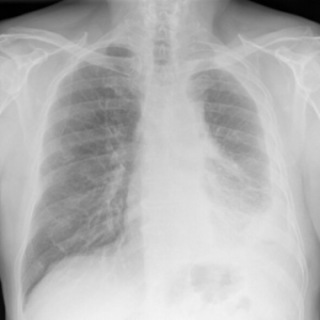
On a chest X-ray, pleural or pericardial mesothelioma tumors appear as wispy white areas around the lungs, while calcified tumors appear bright white. Bones appear white and healthy lungs are dark. Most abnormalities appear as lighter areas that are hazy or solid.
Tumors and scarring may distort chest anatomy. Compressed lungs or a raised diaphragm can be visible on an X-ray.
X-rays are 2D, making it hard to determine if a tumor is in the lung, pleura or the mediastinum around the heart. Additionally, X-rays don’t clearly show peritoneal or testicular mesothelioma. CT, MRI and PET/CT scans offer more detailed images for all mesothelioma types.

Connect with top-rated mesothelioma specialists at a cancer center near you, who will personalize treatment options based on your diagnosis.
Find Your CenterComputed tomography scans are mesothelioma imaging scans that create clear, layered images that show tumors, lymph nodes and organ spread. These CT images help doctors diagnose mesothelioma, stage the disease and pick the best treatment.
How CT Scans Work
The scan itself takes only a few minutes; the visit may take a little longer. A CT scan is painless, but it uses a small dose of radiation. CT can sometimes underestimate how far tumors invade nearby tissues, so your team may add MRI to define edges before surgery. PET/CT is also common to check for active cancer in other areas.
Joey Barna is a pleural mesothelioma survivor. He spoke with us about his mesothelioma imaging scans. He shares, “I went to the hospital, and they thought I had pneumonia because they saw fluid on my lung. A week later I had a follow-up X-ray, and they saw that the fluid was still there. My primary doctor sent me for a CT scan. Fluid had built up and was pressing against my lung. It was preventing me from breathing properly.”
Positron emission tomography, or PET scans, is a type of mesothelioma imaging scan that tracks a small amount of tracer that collects in active cancer cells. Many centers combine this mesothelioma imaging scan with CT (PET/CT) to match hot spots to exact anatomy.
For mesothelioma, PET/CT helps stage the disease, find hidden spread and measure how well treatment is working over time. A 2025 study in Neuroscience Informatics noted new patterns in PET/CT analysis that could soon improve the tracking of brain metastasis in mesothelioma.
How PET Scans Work
These scans can assess tumors’ sizes and locations. This provides vital information for treatment planning. Research suggests PET/CT scans may be better than CT and MRI for staging mesothelioma. They give key insights into the disease’s progression and outlook.
PET scans are also key for tracking treatment response. Doctors can compare PET scans over time. They show if cancer is responding to therapy, stable or progressing. It’s crucial for adjusting treatment. PET are expensive and there’s limited availability. However, scans remain a vital tool in managing mesothelioma.

Karen R.
Mesothelioma Survivor First Diagnosed Thanks to Optional Scan
During a regular annual checkup, Karen R. chose to have an optional heart scan even though her insurance didn’t cover it. It detected fluid around her lungs that led to a pleural mesothelioma diagnosis. She tells us, “If I had not chosen to get this optional scan the cancer would have gone undetected for much longer.”
Karen R.
Magnetic resonance mesothelioma imaging scans, or MRI, use magnets (not radiation) to show soft tissues in great detail. For mesothelioma, MRI can better define how a tumor touches the chest wall, diaphragm or vessels, which matters for surgery planning. A 2025 study in JTCVS Open noted it detected chest wall infiltration with more than 80% greater sensitivity than CT.
MRI scans provide detailed images of soft tissues. These images are key for detecting, diagnosing and staging mesothelioma. MRI is good at identifying changes in soft tissue. MRIs can show how much a tumor has invaded nearby tissues and organs. This information is vital for staging the disease.
How MRI Scans Work
MRI isn’t needed for everyone, but it can be helpful when doctors must know a tumor’s exact edges. Your team may use MRI before surgery or to reassess after systemic therapy.
Newer MRI techniques have improved mesothelioma detection. They highlight small changes the magnetic field causes at the atomic level. These advanced imaging techniques provide additional detail. MRIs are invaluable for a complete assessment of the disease.
Because different mesothelioma types start in different locations, not all patients benefit from all scans. There is no “best” mesothelioma imaging scan. Instead, doctors have an array of tools to fit pieces together at the right time to answer the right question.
CT and PET/CT are often used for whole-body imaging and staging. MRI and ultrasound are better for soft tissue and fluid details.
For pleural mesothelioma, an X-ray is a quick first look at pleural effusion or pneumothorax. The primary test is a CT chest with contrast to observe pleural thickening, nodules and effusions. Ultrasound enables safe thoracentesis when assessing for fluid. Each of these scans flags signs of the disease and guides to the best site for biopsy.
To see tumors better, contrast CT highlights the pleural “rind” & lymphatics. PET/CT helps in staging, illuminating areas of active cancer and metastasis potential within and beyond the chest. An MRI is advantageous if the surgical team needs to know if a tumor invades the chest wall, diaphragm or spine.
For peritoneal mesothelioma, ultrasound can see ascites or fluid in the abdominal cavity and guide paracentesis. A CT of the abdomen/pelvis with contrast shows peritoneal thickening, omental caking and involvement with adjacent organs. These images guide treatment options and determine where biopsies should occur.
For visualization of tumors, a CT is still the gold standard since it assesses the abdomen rapidly, while an MRI, with specific diffusion sequences, can show smaller masses along the liver surface, within the spleen and in peritoneal folds. A PET-CT might help see disease outside the abdomen, though small serosal lesions may be more difficult to assess.
For pericardial mesothelioma, an echocardiogram is the quickest way to see if there is fluid around the heart and its influence on cardiac output. When pericardial thickening or a mass is suspected, either CT or MRI can confirm. Together, these findings best indicate if immediate drainage is needed and where, and rule out other causes of chest pain.
For visualization of pericardial tumors, cardiac MRI distinguishes the heart lining and reveals tumor extent. PET/CT helps stage outside the heart and into the lymphatics. For testicular mesothelioma, scrotal ultrasound is the first step to see if there’s a hydrocele or mass. Then, a CT and usually an MRI assess the spread to the abdominal or thoracic cavities.
When you arrive for your mesothelioma imaging scan, the technologists will guide you. They’ll explain the process and answer your questions. It can also help to talk with your doctor beforehand. They can help prepare you for what to expect in advance.
There are similarities in the process for each imaging type. You’ll need to lie flat on your back for most mesothelioma imaging. X-rays may involve standing or other positions. Staying very still is crucial for precise imaging. If you have limited mobility or pain, let the imaging team know. They can help ensure your comfort.
Mesothelioma Imaging Scan Processes
An MRI scan is similar to a CT, but it’s very loud. Metal coils in the scanner make booming and banging noises. People wear headphones throughout the scan. Also, the MRI scanner is more enclosed, which can cause anxiety. You will have a distress button to press if you need to stop the scan.
Before an MRI, tell your doctor and the technicians if you have any metal in your body. This includes surgical implants, pacemakers or shrapnel. An MRI’s strong magnetic field can affect metal objects. This could cause serious complications.
Many patients often undergo multiple mesothelioma imaging scans. Images are taken during diagnosis and staging. These images help to decide the proper treatment for that person. It’s also essential to do imaging scans for mesothelioma after treatment. They can help track remission and recurrence.
Survivor Tamron Little shares her scan experiences with us. She says, “The frequency of scans can depend on the patient and their progression. Before I had HIPEC surgery, I had a lot of preliminary scans.”
She adds, “After my surgery I had a follow-up CT scan a couple of weeks later. Then, after my doctor saw I was doing well with no cancer being found, it was 1 every 6 months. Then it was every 18 months up until the 5-year mark.”
Kevin Hession, a pleural survivor, says scans can pick up surgery’s effects. He tells us, “There is a lot of scar tissue around my left lung where they did a lot of work. Looking at it from the CT scans, you can see the scar tissue and it kind of surrounds the left lung.”
No, asbestos fibers are microscopic. They aren’t visible on imaging scans. A high-powered microscope can see asbestos fibers in a biopsy. The presence of these fibers can help confirm a diagnosis of an asbestos-related disease.
X-rays and CT scans use radiation. The exposure from X-rays is considered minimal and safe. CT scans involve significantly more radiation. Repeat CTs are avoided for this reason.
People who receive contrast dye during a CT or MRI may have an allergic reaction. Some people also experience nausea.
Though rare, some people can be allergic to the radioactive tracer in a PET scan. It also involves exposure to radiation. These scans aren’t usually recommended for those who are pregnant.
An MRI might cause temporary effects from the magnetic field. These include dizziness, nausea, a metallic taste or brief flashes of light.
Ultrasound can be part of a mesothelioma diagnosis. But its use isn’t common. Soundwaves create its images. These soundwaves don’t travel well through air. So, it is hard to get good images in the chest cavity and abdomen.
While ultrasound’s images aren’t as detailed as CT scans or MRIs, they can be used to look at fluid buildup. Echocardiogram, for example, is a type of ultrasound. Doctors may use it if there’s fluid around the heart. This can help indicate an issue such as pericardial mesothelioma.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2026, February 9). Mesothelioma Imaging Scans. Retrieved June 4, 2026, from https://www.asbestos.com/treatment/scans/
"Mesothelioma Imaging Scans." Asbestos.com, 9 Feb 2026, https://www.asbestos.com/treatment/scans/.
Asbestos.com. "Mesothelioma Imaging Scans." Last modified February 9, 2026. https://www.asbestos.com/treatment/scans/.

Dr. Landau is the Medical Director of Virtual Hematology at the Medical University of South Carolina, where he leads programs that expand access to cancer care through telehealth. With more than 18 years of experience in oncology and hematology, he specializes in hematologic and genitourinary cancers, including bladder, prostate and kidney cancers. He has held multiple leadership roles in cancer program development and previously served as section chief of hematology and oncology at Orlando Health UF Health Cancer Center, where he founded its telehealth program.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
