
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideAscites, or peritoneal effusion, is a buildup of excess fluid in the abdomen. Cirrhosis, liver diseases, peritoneal mesothelioma or other conditions can cause fluid to build up. Doctors may use chemotherapy or drain the fluid to treat this fluid accumulation.
“The beauty of the Opdivo and Yervoy, it works in the chest. It works through the bloodstream. So anywhere that you can see so many cells hiding, they can get there. So, can I guarantee that your ascites will go away? Unfortunately, I cannot. But if you enjoy a response to the treatment, it may very well decrease the ascites.”

Sean Marchese, registered nurse and oncology medical writer
“Dr. Strocel treated Trina Reif, a 20-year peritoneal survivor, and spoke to us about her case. He said, 'Trina had unexplained ascites. We did an exploratory laparotomy. We also did multiple peritoneal biopsies. She had an angry looking peritoneum. Her diagnosis was abdominal mesothelioma.'”
Dr. Anton Strocel, retired OB/GYN
“As a woman, especially as a young woman with abdominal pain being my major symptom, I had a really hard time convincing someone that I was in pain. Like, a really hard time. I was told it was just my period. If I had given up when they first told me, 'Oh, it's just a little period pain,' I might not be here today. You have to trust yourself and you have to trust your gut, no matter what people say to you.”

Jayda Kelsall, a peritoneal mesothelioma survivor whose exploratory laparoscopy revealed more than a gallon of fluid in her abdomen
“The beauty of the Opdivo and Yervoy, it works in the chest. It works through the bloodstream. So anywhere that you can see so many cells hiding, they can get there. So, can I guarantee that your ascites will go away? Unfortunately, I cannot. But if you enjoy a response to the treatment, it may very well decrease the ascites.”

Sean Marchese, registered nurse and oncology medical writer
“Dr. Strocel treated Trina Reif, a 20-year peritoneal survivor, and spoke to us about her case. He said, 'Trina had unexplained ascites. We did an exploratory laparotomy. We also did multiple peritoneal biopsies. She had an angry looking peritoneum. Her diagnosis was abdominal mesothelioma.'”
Dr. Anton Strocel, retired OB/GYN
“As a woman, especially as a young woman with abdominal pain being my major symptom, I had a really hard time convincing someone that I was in pain. Like, a really hard time. I was told it was just my period. If I had given up when they first told me, 'Oh, it's just a little period pain,' I might not be here today. You have to trust yourself and you have to trust your gut, no matter what people say to you.”

Jayda Kelsall, a peritoneal mesothelioma survivor whose exploratory laparoscopy revealed more than a gallon of fluid in her abdomen
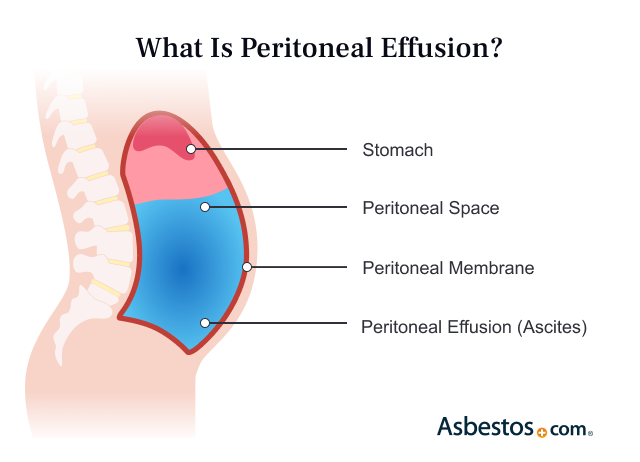
Ascites is a buildup of fluid in your peritoneal cavity (space in your belly containing your digestive organs). When fluid accumulates in this space, it can cause your belly to swell. Ascites is common in people with peritoneal mesothelioma and liver issues.
The peritoneum is a thin membrane that lines the inside of your abdominal cavity. Conditions such as cirrhosis or cancers, like peritoneal mesothelioma, can cause fluid to cross the peritoneum. When this happens, the fluid then collects in your peritoneal cavity, and you can notice swelling and other symptoms.
Protein levels in your abdominal fluid are measured and used to help classify ascites or peritoneal effusions. An exudate is peritoneal fluid with a high protein level. A transudate is peritoneal fluid with a low protein level. This can help doctors find the cause of your peritoneal effusion. Cirrhosis, or liver disease, usually causes low protein levels. Cancer and infections usually cause high levels.
Cirrhosis, or scarring of the liver, is the most common cause of ascites. Cirrhosis can cause high pressure in your liver’s veins. This can force fluid into your abdominal cavity.
Cancer, such as peritoneal mesothelioma, is the second most common cause of peritoneal effusions. Cancer cells can irritate your abdominal lining. This can cause excess fluid to build up. Peritoneal mesothelioma tumors, for example, can also cause the membrane to leak fluid. As the mesothelioma spreads, covering more of the peritoneal surface, ascites often worsens.
Causes of Peritoneal Effusions and Percentage of Cases
Infections can also cause pleural effusions. Peritonitis is a nonspecific term for irritation of the abdominal lining. Any cause of peritonitis can cause fluid to build up. Tuberculosis and pancreatitis, for example, are causes. Bacterial infections, from conditions like a perforated ulcer or perforated appendicitis can also cause ascites to develop. Irritation of the peritoneum tends to be painful.
Heart or kidney failure can also cause ascites. When there’s less blood flow to your kidneys, sometimes because your heart isn’t pumping with enough force, your kidneys will respond, reducing urine output, and fluid retention can happen. Heart failure can also affect your liver, causing the pressure in the liver veins to increase. This can lead to the development of ascites.
The most common symptom of ascites is discomfort. As abdominal fluid develops, people can feel bloated or full. Some people also report feeling nausea and losing appetite. Symptoms can vary depending on the severity of the ascites and its cause. As the ascites worsens, pain and physical limitations can develop.
Symptoms of Abdominal Ascites
Ascites is always a sign of a problem. It’s one of many signs and symptoms of mesothelioma. It occurs in more than 50% of peritoneal mesothelioma cases. It can also occur when other types of mesothelioma spread to the abdomen.
Dr. Anton Strocel, an OB/GYN who treated Trina Reif, spoke to us about her case. Trina is a 20-year peritoneal survivor. Dr. Strocel said, “Trina had unexplained ascites. We did an exploratory laparotomy. We also did multiple peritoneal biopsies. She had an angry looking peritoneum. Her diagnosis was abdominal mesothelioma.”

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideDoctors use a mix of tests to diagnose ascites. A physical exam and imaging scans are performed. Tests such as ultrasound and CT scans can show excess fluid in your abdominal space. A doctor will likely think of ascites if there is severe abdominal swelling.
If fluid is present, doctors need to collect a sample of the fluid (a liquid biopsy). The key to a diagnosis is the laboratory analysis of your peritoneal fluid. The fluid is often collected during a procedure known as a paracentesis. This procedure places a needle into your abdominal fluid to drain and collect it for analysis.
The sample is analyzed in a pathology lab. The type of ascites you have is determined. Pathologists look for potential cancer cells. This process is known as cytology.
A 2022 study in the journal Cytopathology looked at cytology testing of ascites fluid. It was able to detect malignant mesothelioma about 34% of the time. This underscores why doctors rely on tissue biopsies most of the time for the diagnosis of peritoneal mesothelioma.

Jayda K.
Recurrent Ascites Leads to Peritoneal Mesothelioma Diagnosis
“As a young woman with abdominal pain, I had a really hard time convincing someone I was in pain. A really hard time. I was told it was just my period,” Jayda said. Her doctors finally did a laparoscopy. Her peritoneal effusion turned out to be more than a gallon of fluid and the surgeon saw growths on her peritoneum. A biopsy confirmed her peritoneal mesothelioma diagnosis.
Jayda K.
Treatments for abdominal ascites depend on its cause. Treatments for cancer-related ascites typically involve a combination of fluid drainage, chemo, surgical procedures and possibly emerging therapies. These approaches aim to relieve symptoms while controlling the underlying condition. A multidisciplinary approach, involving input from medical doctors, surgeons and oncologists is warranted to evaluate and treat abdominal ascites.
Treatment Options for Peritoneal Effusions
Important in mesothelioma treatment, customizing treatment for each person with ascites supports better symptom management and improves quality of life. Abdominal ascites results from benign or malignant diseases. Management varies accordingly, focusing on symptom relief in benign cases and combining multiple treatments when cancer like mesothelioma is involved.
Ongoing clinical studies continue to enhance treatment strategies. For instance, a 2023 study in the Journal of Surgical Oncology found combining fluid drainage with chemo and nutritional support provides superior patient outcomes.
Some measures can reduce the risk of liver disease and certain cancers, but they can’t guarantee prevention. Adopting a healthy lifestyle may lower the chance of developing cirrhosis. Key steps include avoiding alcohol and tobacco use, maintaining regular exercise and following a balanced diet. Reducing salt intake can also help limit fluid retention in the body.
Ascites can exert pressure on abdominal organs and the chest, causing discomfort. Persistent fluid accumulation increases the risk of infection, such as spontaneous bacterial peritonitis. Additional complications may include abdominal hernias, abdominal pain, difficulty breathing, fluid buildup in the lungs and a heightened risk of further infections. Loss of appetite can lead to nutritional issues.
Several factors increase the likelihood of developing ascites. These include: abdominal infections, abdominal or pelvic cancers, alcohol abuse, congestive heart failure, genetic liver diseases, hepatitis B or C and nonalcoholic fatty liver disease.
Conditions that lead to cirrhosis represent the most significant risk. Certain cancers and infections markedly raise the risk as well. Heart or kidney failure can also contribute to fluid accumulation in the abdomen.
Peritoneal effusions often recur after treatment, depending on their cause. Fluid buildup may return within days or months. In malignant ascites, recurrent ascites can indicate advancing cancer. Persistent or recurrent ascites may be a sign of cancers such as mesothelioma. In such cases, seeking a second medical opinion and consulting a mesothelioma specialist can be beneficial.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2026, May 29). Ascites. Retrieved June 4, 2026, from https://www.asbestos.com/mesothelioma/peritoneal-effusion/
"Ascites." Asbestos.com, 29 May 2026, https://www.asbestos.com/mesothelioma/peritoneal-effusion/.
Asbestos.com. "Ascites." Last modified May 29, 2026. https://www.asbestos.com/mesothelioma/peritoneal-effusion/.

Dr. Rupesh Kotecha is a renowned radiation oncologist in leadership roles at Miami Cancer Institute. He is an associate professor at Florida International University's college of medicine and an adjunct faculty member at Memorial Sloan Kettering.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
