Michael Cole describes how aggressive EPP treatment for mesothelioma saved his life. He also explains his personal cancer journey and his other mesothelioma treatments.
Extrapleural Pneumonectomy
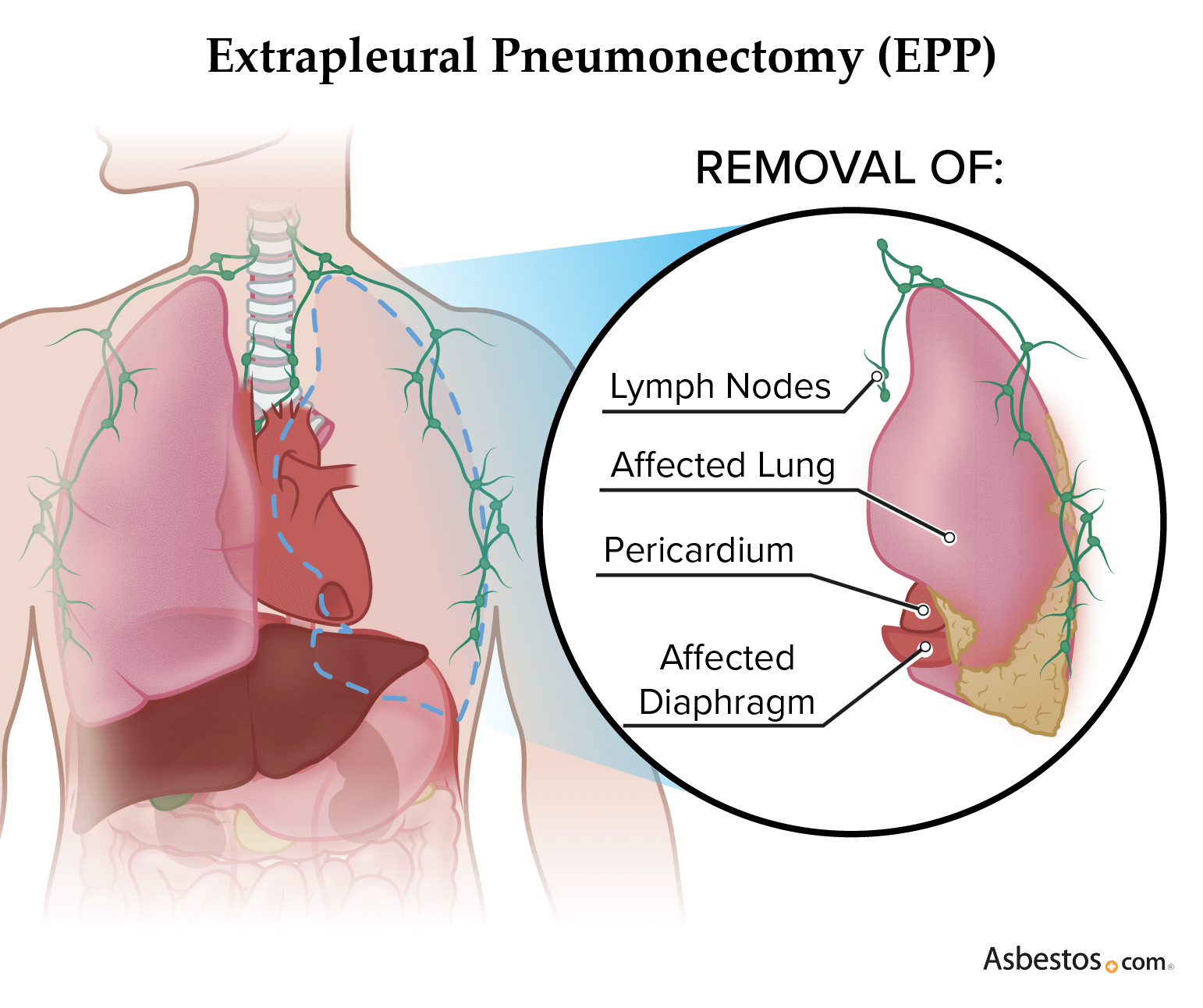
Extrapleural pneumonectomy (EPP) is a type of surgery used for treating pleural mesothelioma. During an EPP, doctors remove the lining of the lung (pleura), the lung, the sack around the heart (pericardium) and the diaphragm. Recovery takes at least six to eight weeks.
What Is an Extrapleural Pneumonectomy?
An extrapleural pneumonectomy is a pleural mesothelioma surgery that removes the entire cancerous lung. An EPP can improve breathing and quality of life. After recovery, patients often feel more at ease. This allows them to return to their daily activities or even resume work.
The mesothelioma procedure gets its name from the original surgery known as a pneumonectomy, which removes only the affected lung. The “extrapleural” means the surgeon goes beyond the entire removal of the lung to include the removal of its pleural lining, nearby lymph nodes, and parts of the heart lining and diaphragm.
Key Facts About Extrapleural Pneumonectomy
- Extrapleural pneumonectomy is a complex, invasive surgery that removes one diseased lung and other structures in the chest to treat pleural mesothelioma.
- EPP is for early-stage cancer confined to one side of the chest, and patients must be in good overall health to tolerate the procedure.
- Recovery from EPP is lengthy and requires significant physical rehabilitation. Fatigue, breathlessness and pain are common after the surgery.
- While it offers a chance for improved survival, EPP can lead to serious complications. Expert surgeons are critical about patient selection to limit the risk of complications.
Dr. Sameer Jhavar, a radiation oncologist at Baylor Scott & White Medical Center, believes an EPP can help certain patients. “It all depends on the patient selection,” says Dr. Jhavar. “In the right patient population, [the EPP] can be done safely and effectively and provide survival hope.”
Who Is Eligible for EPP?
You may be eligible for an extrapleural pneumonectomy for mesothelioma if your doctor believes you can recover from possible complications. You should also be in good overall health. Eligibility is limited if you have the sarcomatoid cell type, late-stage cancer or certain preexisting conditions. Talk with a mesothelioma surgeon to determine if you meet the criteria.
EPP Eligibility Criteria
- Absence of certain preexisting conditions
- Diagnosis with early-stage pleural mesothelioma between stages 1 and 3
- Epithelial or biphasic cell type
- Good overall health and adequate heart and kidney function
- Good function of the unaffected lung (known as pulmonary reserve)
The National Comprehensive Cancer Network does not recommend surgery for pleural mesothelioma cases that have progressed beyond stage 3A. Unfortunately, many patients are diagnosed after their cancer has progressed to stage 3B or 4. A late-stage diagnosis makes patients ineligible for an EPP.
Surgeons may recommend pleurectomy/decortication for certain patients who cannot tolerate the more aggressive EPP surgery. A P/D may be better for patients with symptoms like entrapped lung syndrome and recurrent pleural effusions.
How Is Extrapleural Pneumonectomy Performed?
Before performing the extrapleural pneumonectomy surgery for mesothelioma, doctors run tests to ensure a patient is a good candidate. Lung function tests check if the remaining lung will be strong enough to work well on its own. Doctors also check the patient’s heart health to confirm they are fit for major surgery.
EPP Procedure Steps
- Preparation: You’ll receive general anesthesia to ensure comfort during surgery.
- Incision: The surgeon makes a careful incision on one side of the chest to access the affected area. After this, the doctor will remove the sixth rib and use a rib spreader to look for any diseased tissue.
- Tissue Removal: The diseased lung, pleura, nearby lymph nodes and parts of the diaphragm and pericardium are carefully removed. Surgeons may remove other structures, such as ribs or parts of the peritoneum, if they see cancer elsewhere. They aim to remove as much cancerous tissue as possible.
- Reconstruction: The diaphragm and pericardium are rebuilt with synthetic materials.
- Closure: Doctors close the incision, and you’ll move to recovery. You will also be closely monitored with supportive care.
Imaging scans help surgeons see how far the cancer has spread to guide surgical decisions. A PET/CT scan can assess if tumors have spread to the other side of the chest or into the abdomen. An MRI can identify tumors in the chest wall and diaphragm.
What Are the Benefits of Extrapleural Pneumonectomy?
An extrapleural pneumonectomy can extend survival, reduce symptoms and improve quality of life. While there is currently no cure for mesothelioma, EPP can help control it. Many patients see improvements in their lives by living for several extra months or even years.
Benefits of Extrapleural Pneumonectomy
- Disease Control: An EPP removes the affected lung and nearby tissues to eliminate cancer. It removes a lot of cancerous tissue at once, which helps slow disease progression.
- Improved Survival: The procedure can extend life expectancy, especially in early-stage cases. In patients with stages 2 to 3A mesothelioma, EPP can remove more cancer tissue than P/D, which is important in improving the odds of survival.
- Multimodal Therapy: An EPP facilitates the effectiveness of additional treatments like chemotherapy or radiation. These can extend lifespan. Using high-dose radiation therapy after EPP, doctors can help prevent the cancer from coming back in the same area.
- Symptom Relief: EPP has the potential to reduce pain, breathlessness and other cancer-related symptoms.
Pleural mesothelioma survivor Michael Cole in 2015 sought medical advice from mesothelioma pioneer Dr. David Sugarbaker, who worked at Baylor College of Medicine in Houston. Sugarbaker recommended an aggressive treatment with EPP and chemo.
“As it has turned out, the EPP with HITHOC followed by four rounds of chemotherapy was not the end of my treatment journey, but rather only the beginning,” Cole said. “I believe the aggressive treatment I had in the beginning was absolutely necessary to give me a chance to be here now, and I am grateful for the decision we made.”

Get a free guide with the latest mesothelioma treatments and clinical trials.
Get Yours NowRisks and Drawbacks of EPP
Some mesothelioma surgeons believe the lung-sparing pleurectomy and decortication is a safer alternative to EPP. In fact, most surgeons avoid this aggressive procedure. A P/D is ideal for stage 1 pleural mesothelioma, while an EPP can remove visible tumors in patients with stages 2 through 3A. Some surgeons can offer P/D surgery and convert the procedure into an EPP if they discover more cancer than imaging detected.
An extrapleural pneumonectomy can offer hope for patients, but it’s important to understand the most serious risk is death after surgery. The mortality rate for EPP is higher compared to the less invasive P/D procedure. A 2024 review comparing mortality found a death rate of 6% for EPP and 2.2% for P/D.
Additionally, complications can arise after EPP surgery. The 2024 review reported that the complication rate ranged between 38% and 68% for EPP. The P/D complication rate ranged between 26% and 58%. Notably, nearly 10% of EPP patients required an unexpected return to the operating room, compared to just 1.5% for P/D patients.
Another important consideration is the possibility of cancer recurrence after EPP. According to a 2012 study on multimodal therapy for mesothelioma, local recurrence can occur in up to 80% of EPP patients. But this rate drops to 13% when patients receive radiation therapy after surgery. Nonetheless, recurrence at distant sites can still affect up to 55% of patients.
Short-Term EPP Risks
Other risks of EPP for mesothelioma include blood clots, heart problems and pneumonia. Understanding these risks can help patients and their families make informed decisions about their treatment options.
Common Short-Term EPP Risks
- Wound infection
- Pneumonia
- Fluid accumulation in lungs
- Blood clot in the lungs
- Pus accumulation in pleural space
- Kidney failure
- Abnormal connection between the bronchial cut and pleural space
- Heart problems (cardiac arrhythmias and heart attack)
Long-term risks can include shortness of breath. This might lead to needing an oxygen tank or a mechanical respirator for a while after surgery.
It’s important to watch for signs of serious issues that may arise after an EPP. These signs include fever, chest pain, cough and shortness of breath. If your incision becomes red, swollen, painful or starts to ooze blood, these could also be warning signs. If you notice any of these symptoms, please contact your doctor immediately.
What Is the Recovery Process Like After EPP?
Recovering from an extrapleural pneumonectomy can take some time. Healing happens in phases. It also gets easier with time when you follow the guidance of your medical team.
- Immediate Postsurgery: In some cases, patients may need a respirator to help with breathing for the first few days after surgery. Additionally, drainage tubes will be in place for 1 to 2 days to help monitor for any bleeding or air leaks. Most patients stay in the hospital for at least 2 weeks following the operation. During this time, the medical team will closely monitor you because it’s common to experience some complications.
- First 6-8 Weeks: The recovery period lasts at least 6 to 8 weeks. It may extend longer for some patients. It’s important to start moving and taking deep breaths. This helps maintain good lung function.
- Long-Term Recovery: Even 6 months after surgery, you might notice that exercise can still feel challenging because of shortness of breath. Remember, this is all part of the healing journey, and in time, you will likely feel stronger.
Pleural mesothelioma survivor Cole says recovery from an EPP is challenging. But he credits the surgery with his long-term survival.
“When I woke up, I felt like I had been run over by a truck, and I’m pretty sure I looked worse. My whole body was out of whack, including my remaining lung,” Cole told Asbestos.com. “It hasn’t been easy, and we have been through hard times and uncertainty since that day, but don’t misunderstand. We have not been in despair.”
Prognosis After Surgery
The prognosis after extrapleural pneumonectomy surgery depends on several factors, including the patient’s age and overall health, the cancer’s stage and cell type, and whether the surgeon could remove the tumors completely. A 2024 review of EPP for pleural mesothelioma reported a median survival of 18 months with the longest survival recorded at 35 months.
Among the most important factors affecting surgical outcomes: Extent of lymph node involvement. When more lymph nodes have cancer, the success of an EPP is diminished. Expert surgeons specializing in EPP for mesothelioma should perform the procedure to ensure the best results.
Other therapies can improve prognosis after EPP. The National Comprehensive Cancer Network recommends chemotherapy before surgery based on clinical trial results. It also recommends postoperative chemotherapy in patients who did not receive chemo before surgery.
How Does Extrapleural Pneumonectomy Compare to Other Treatments?
Medical experts in the mesothelioma community have conflicting opinions about the value of extrapleural pneumonectomy compared to other procedures. Some experts believe it benefits certain patients. Others believe the pleurectomy and decortication surgery is a safer and equally effective option.
A 2022 study found that EPP had similar long-term outcomes to pleurectomy and decortication when used as part of a broader. However, it is important to note that EPP had higher mortality rates after surgery. The study encourages patients to choose the safest treatment option that they can handle.
The National Comprehensive Cancer Network says factors like cell type, staging, patient health and their surgical risk tolerance can help decide whether to perform an EPP or P/D. A patient’s pulmonary reserve and the surgeon’s experience and expertise are important as well.
Common Questions About Extrapleural Pneumonectomy
- How much does extrapleural pneumonectomy cost?
-
The potential cost of an extrapleural pneumonectomy is around $82,000. This estimate can vary greatly throughout the U.S. It’s based on a 2019 report about the cost of mesothelioma treatment, and it accounts for inflation.
- How can patients prepare mentally and physically for EPP?
-
EPP patients can prepare for the procedure by improving their overall health. A balanced diet, gentle exercise and good sleep prepare the body for aggressive surgery. Preoperative pulmonary rehabilitation may be recommended. Quitting smoking will improve the function of the remaining lung after the procedure. Mental preparation may include counseling, joining support groups and learning about the procedure and recovery process.
- What kind of support resources are available for EPP patients?
-
EPP patients can benefit from postsurgical follow-up care, physical therapy and pain management programs. A dietitian can recommend a diet plan to optimize recovery and maintain strength. Medical grants and other forms of financial assistance can help patients afford treatment.
- Are there non-surgical alternatives to EPP for mesothelioma?
-
Other treatments for mesothelioma include immunotherapy, chemotherapy and radiation. Oncologists also use targeted therapies and Tumor Treating Fields therapy to treat mesothelioma.





