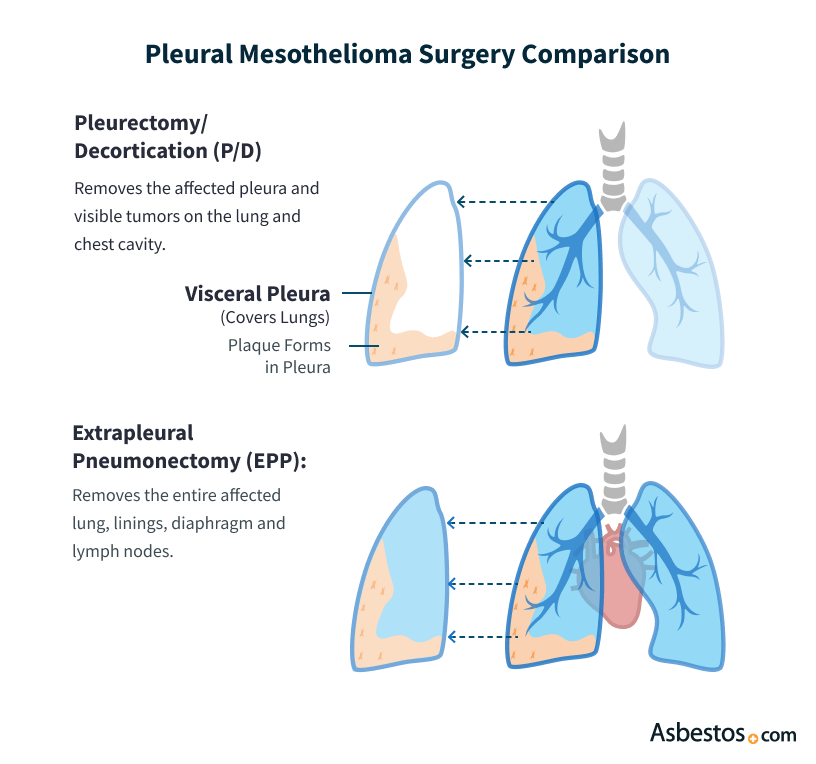
Pleurectomy Decortication (P/D) vs. Extrapleural Pneumonectomy (EPP)
Pleurectomy/decortication (P/D) and extrapleural pneumonectomy (EPP) are the two most common tumor-removing surgeries for pleural mesothelioma. P/D is associated with fewer complications and better quality of life, but surgeons may choose an EPP if cancer has spread into the lung.
Differences Between P/D and EPP Surgeries
The goal of pleurectomy/decortication (P/D) and extrapleural pneumonectomy (EPP) is to remove all pleural mesothelioma cancer growth, relieve symptoms and extend the patient’s life span. Because both surgeries are performed locally in the chest cavity, they work best when the cancer has been found as early as possible and not spread outside of the chest cavity.
If the mesothelioma has advanced to a late stage and is no longer localized, neither procedure may provide significant benefit for the patient. In addition, a patient must be in good overall health to survive and recover from any major chest surgery. Otherwise, it cannot safely be offered even in early-stage cases.
P/D may involve scraping cancer cells off the surface of a lung, but it leaves both lungs intact. Most thoracic surgeons now prefer the P/D procedure for this reason, but they will still perform an EPP if they determine it is the only way to remove as much tumor growth as possible.

Find the top cancer centers trusted by mesothelioma patients nationwide.
Get Help NowSurvival Rates
Both P/D and EPP improve survival rates for pleural mesothelioma patients, especially when combined with other treatments as part of multimodal therapy. In a 2022 study, mesothelioma patients who underwent EPP had a median overall survival of 15 months versus 22 months for those who underwent pleurectomy and decortication surgery.
Some studies have associated P/D with longer survival times than EPP, but this does not necessarily mean the survival advantage comes from the procedure. Many factors are associated with survival including the cancer stage and indications to select one procedure versus the other.
The cancer stage and cell type, the patient’s age and the types of adjuvant therapies used all affect survival times much more than the type of surgery performed.
Deciding Which Surgery Is Right
When choosing between EPP and P/D, the surgeon will consider the patient’s specific medical needs and preferences. Many thoracic surgeons are more comfortable with one procedure than the other, so the patient’s choice of cancer center and mesothelioma specialist may influence the type of surgery they receive.
| Pleurectomy/Decortication (P/D) | Extrapleural Pneumonectomy (EPP) |
|---|---|
| Less invasive: Removes the lining of the lung and other nearby tissues, but leaves lung intact | More invasive: Removes the lung and surrounding tissues, reducing patient’s quality of life |
| Lower mortality rate: 1–2% of patients die during or immediately after surgery | Higher mortality rate: 4–5% of patients die during or immediately after surgery |
| Less severe complications: May cause prolonged air leak in chest | More severe complications: May cause abnormal heart rate or arterial blockage |
If the patient is a candidate for surgery, the surgeon will consider the size and location of the tumor. If the tumor is localized to the pleural lining, P/D may suffice, but if the tumor has spread to the lung, EPP may be necessary to remove a greater portion of the tumor.
Mesothelioma specialists can use a variety of imaging scans to try to assess the extent of the cancer’s spread, but in many cases, a surgeon will not make the final judgment call until they have opened the patient’s chest cavity during surgery and seen the extent of the tumor growth directly. A surgeon may begin surgery intending to perform P/D but then realize an EPP would be better, or the other way around.
We’re finding that we’re able to remove all the tumor that’s visible even with the lung-sparing pleurectomy/decortication. That is why there has been a shift toward doing [P/D] more so than in decades past.
Choosing between the two procedures is complex, but both surgeries can give the patient a good chance to live longer with pleural mesothelioma. A mesothelioma specialist is the best doctor to help a patient and their loves ones make the decision between an EPP or the P/D surgeries.
Recommended Reading





