
Connect with top-rated mesothelioma specialists at a cancer center near you, who will personalize treatment options based on your diagnosis.
Find Your CenterSophisticated imaging techniques allow radiologists to administer higher doses of radiation to a tumor without increasing the risk of toxicity for the patient. Image-guided radiation ensures better coverage of the tumor and less collateral damage to healthy tissue.
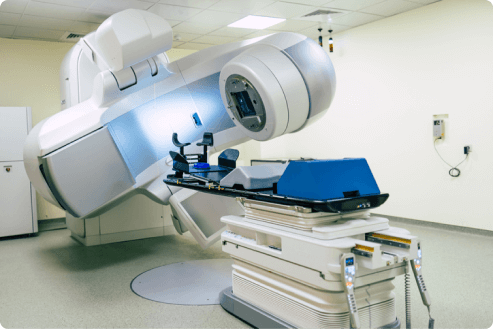
Image-guided radiation therapy is a type of cancer treatment that uses precise imaging to target beams of high-energy radiation. Mesothelioma specialists often use IGRT as a type of external beam radiation in aggressive treatment plans. However, oncologists find it challenging to administer radiation to mesothelioma patients safely.
Mesothelioma tumors form close to sensitive vital organs such as the lungs, heart, liver, intestines and kidneys. The tumors may also move when the patient breathes or their abdominal organs shift because of digestion. IGRT improves the accuracy of radiation delivery so healthy tissue isn’t damaged.
Radiation oncologists must make a trade-off between treatment effectiveness and safety. A higher dose of radiation will kill more cancer cells, but it could also cause severe complications if it accidentally hits healthy cells.
Modern technologies such as intensity-modulated radiation therapy and proton therapy can target areas in the body much more selectively. Even so, these therapy techniques are only as good as the imaging scans that guide them, and this is where the emerging methods of IGRT come in.
IGRT for mesothelioma involves performing imaging scans immediately before or during every radiation therapy session. This way, the radiologist can adjust the treatment if the tumor site’s position changes or the patient has lost or gained weight.
These types of combination devices have become more common in the past decade. And many experts expect the average IGRT session duration to shorten as technology improves. However, in many cases, cancer patients still receive imaging scans and radiation therapy on different days and in other facilities. Research has shown this isn’t ideal.
Lung cancer presents many of the same targeting problems as pleural mesothelioma. A study of 91 patients with lung cancer revealed daily imaging scans during radiation therapy were associated with a longer median survival time than weekly imaging scans.
As with all types of cancer treatment, the best hope for mesothelioma patients is to go to one of the top cancer centers in the country. Remember, only an experienced mesothelioma specialist can determine whether any radiation therapy is appropriate. Mesothelioma is a rare and complex form of cancer. Every case requires an individualized treatment plan.
Even when a doctor performs an imaging scan before radiation treatment, the static scan might not account for the tumor site’s motion and the body’s vital organs. Specialists developed four-dimensional imaging to address this problem.
In 4D imaging, the fourth dimension is time. This property allows doctors to track the cyclical path of the tumor site’s position in the body as the patient breathes.
You could think of this as a 3D video of the inside of the chest that plays on a loop. It shows doctors how organs move when the patient inhales and exhales.
A radiologist could use 4D imaging to ensure the most intense radiation stays confined to the tumor site. Or they could synchronize the aim of the radiation machine to the motion of the target in the body.

Connect with top-rated mesothelioma specialists at a cancer center near you, who will personalize treatment options based on your diagnosis.
Find Your CenterA 2021 research paper in the World Journal of Clinical Oncology stated IGRT allows for the use of more precise treatments. The authors noted IGRT also enables the delivery of “potentially curative doses” to tumors while “maintaining doses to surrounding healthy tissue at an acceptable level.”
Siemens in 2000 unveiled a computed tomography scanner that hospitals could install alongside a linear accelerator in the same room. This advancement made it possible to take a CT scan and administer radiation without moving the patient.
Two years later, Accuray introduced the TomoTherapy System, a single machine that can perform CT scans and administer intensity-modulated radiation therapy. In 2015, doctors hailed the development of the first combination of linear accelerator and magnetic resonance imaging machines.
Recommended ReadingYour web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, February 9). Image Guided Radiation Therapy (IGRT). Asbestos.com. Retrieved May 20, 2026, from https://www.asbestos.com/treatment/radiation/igrt/
Selby, Karen. "Image Guided Radiation Therapy (IGRT)." Asbestos.com, 9 Feb 2026, https://www.asbestos.com/treatment/radiation/igrt/.
Selby, Karen. "Image Guided Radiation Therapy (IGRT)." Asbestos.com. Last modified February 9, 2026. https://www.asbestos.com/treatment/radiation/igrt/.

Dr. William Breen is an innovative radiation oncologist in Rochester, Minnesota, at the much-acclaimed Mayo Clinic, a National Cancer Institute-designated Comprehensive Cancer Center for more than 40 years.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
