
Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistOne in eight women in the U.S. is diagnosed with breast cancer. The cause of breast cancer is linked to a variety of external risk factors in addition to natural factors that are typically out of a person’s control.

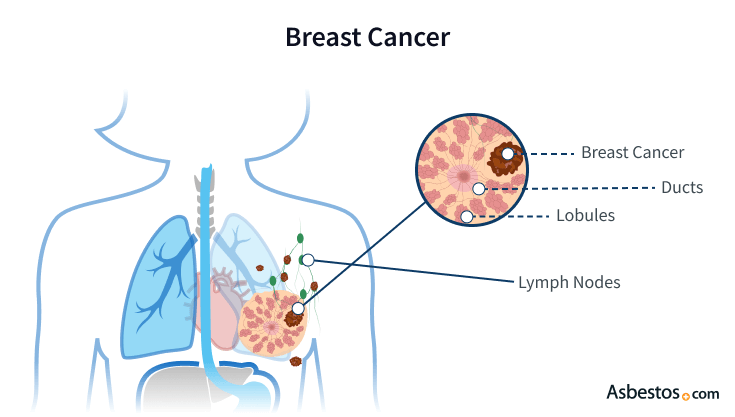
Breast cancer is a disease associated with abnormal cell growth in the breast. Invasive ductal carcinoma, invasive lobular carcinoma, Paget’s disease, medullary mucinous and inflammatory breast cancer are all types of breast cancer.
Approximately 287,850 new cases of invasive breast cancer were diagnosed in 2022. Breast cancer is the most common cancer diagnosed in women, who are 100 times more likely to be diagnosed with it than men. The five-year survival rate is 91% for all types of breast cancer combined.
Natural risk factors include gender, age, race, early onset of menstruation and family history and genetics. According to a 2016 study, environmental factors play a role in the risk of breast cancer including exposure to ionizing and nonionizing radiation, pesticides, polycyclic aromatic hydrocarbons and metals.
Some studies have found higher rates of breast cancer among women exposed to asbestos, although the link between the two appears thin. A study published in 2021 reinforced the evidence that chronic inflammation from asbestos could be a major risk factor in the development of breast cancer.
Asbestos is a carcinogen that has been linked conclusively to other health conditions such as mesothelioma cancer, but its exact correlation to breast cancer is uncertain. Although researchers have noted an elevated incidence of breast cancer in women who have been exposed to asbestos fibers, studies have not yet determined how asbestos directly affects breast tissue.
According to Dr. Debra David, many studies that have attempted to demonstrate a correlation between asbestos exposure and breast cancer fail to do so strictly because they do not achieve statistical significance, meaning there were not enough women involved in the study to make it statistically conclusive. Two international studies delivered different conclusions from each other.
One Australian study published in 2009 reviewed the potential association between exposure to blue asbestos and cervical, ovarian, uterine and breast cancers. Nearly 3,000 women from Wittenoom — the home of a large asbestos company operated until 1966 — were compared with the general Western Australian population.
Cervical and ovarian cancers were slightly more prevalent in former factory workers and town residents than the general population. Breast cancer rates remained the same.
A similar study that monitored cancer diagnoses in British asbestos factory workers was the only one of its kind to suggest an association between occupational asbestos exposure and elevated rates of breast cancer. This project found a slightly increased rate of breast cancer diagnoses in female factory workers who experienced significant exposure over two or more years. The study expected 10.48 deaths from breast cancer, yet 12 participants passed away from the illness.
Another British study, ” Prevalence of Asbestos Bodies in a Necropsy Series in East London,” examined the lungs of 178 female participants for the presence of asbestos fibers. The mineral was present in 30 percent of all women in the study, yet the majority of this percentage was found in the subgroup of women who had been diagnosed with breast cancer. Of the 82 female participants with the illness, 38 were found to have asbestos in their lungs.
Authors within the study suggested that asbestos fibers may have reached the breast tissue through retrograde lymphatic flow from the lungs to the chest wall, while another study yielded another hypothesis. The second study implied that asbestos fibers may pierce the lungs and pass through the muscles that cover the chest wall, eventually reaching the breast tissue. While the evidence to support either suggestion is limited and does not speak to a causal relationship, the potential link between asbestos and breast cancer requires continued study to warrant any factual association.
A Finnish study published in the American Journal of Industrial Medicine in 1999 reported on breast cancer risk in certain occupations. The study found women who were occupationally exposed to medium or high levels of asbestos were 1.3 times more likely to develop postmenopausal breast cancer than the general population.
The same elevated risk was found in women exposed to human-made vitreous fibers. Women exposed to silica dust and other mineral dust were 1.1 times more likely to develop postmenopausal breast cancer. These findings may suggest that microscopic fibers and mineral dust might increase the risk of developing breast cancer.
In a 2011 study, the International Agency for Research on Cancer (IARC) evaluated more than 900 different agents and determined that no agents in the workplace, including asbestos exposure, were associated with breast cancer. Only night shift work was associated with breast cancer, which is likely connected to disruption of hormones or immune function.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistSome contributing factors that increase breast cancer risk are referred to as “partial risk factors.” Some of these may be within an individual’s control, such as alcohol consumption.
Many partial risk factors, however, are not something an individual can choose without compromising their health in other areas, for example, receiving radiation therapy to the chest. And others, such as whether or not to have children, can be deeply personal choices.
According to the American Cancer Society, about 5 to 10% of breast cancer cases can be directly attributed to mutations of certain inherited genes. Many other factors, such as exposure to carcinogens, may also be out of a cancer patient’s control.
Recommended ReadingYour web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Dixon, S. (2026, February 9). Breast Cancer. Asbestos.com. Retrieved June 4, 2026, from https://www.asbestos.com/cancer/breast/
Dixon, Suzanne. "Breast Cancer." Asbestos.com, 9 Feb 2026, https://www.asbestos.com/cancer/breast/.
Dixon, Suzanne. "Breast Cancer." Asbestos.com. Last modified February 9, 2026. https://www.asbestos.com/cancer/breast/.

Dr. Andrea Wolf is the Director of the New York Mesothelioma Program at Mount Sinai in New York City. She focuses on multidisciplinary treatment, clinical research, community outreach and education.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
