Based on Your Reading:
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Cryotherapy, also known as cryosurgery or cryoablation, kills cancer cells by exposing them to extreme cold. Certain mesothelioma specialists have had success using cryotherapy in combination with other forms of cancer treatment.
Written by Karen Selby, RN • Edited By Walter Pacheco • Medically Reviewed By Dr. Rupesh Kotecha
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, February 2). Cryotherapy. Asbestos.com. Retrieved April 25, 2024, from https://www.asbestos.com/treatment/cryotherapy/
Selby, Karen. "Cryotherapy." Asbestos.com, 2 Feb 2024, https://www.asbestos.com/treatment/cryotherapy/.
Selby, Karen. "Cryotherapy." Asbestos.com. Last modified February 2, 2024. https://www.asbestos.com/treatment/cryotherapy/.
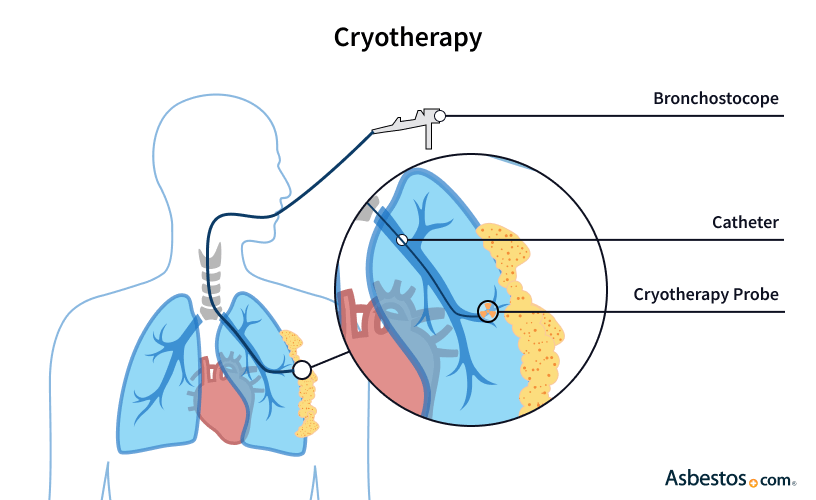
When a doctor performs cryotherapy, they will insert a special tool called a cryoprobe into the patient’s body. This helps them to pinpoint and target any solid tumors. CAT scans are used to help make sure that the tumor is targeted accurately. The needle has super-cooled nitrogen or argon flowing through it which freezes the cancer tissue around the tip of the probe.
Doctors use a special technique to get rid of cancer cells. They freeze and thaw the tissue in the area where the cancer is several times, which stops blood from flowing to it. Using CAT scans and ultrasounds, they can make sure that healthy tissue isn’t hurt while getting rid of cancer cells. Another way to do cryotherapy is by spraying super-cooled nitrogen on tumors.
Cryotherapy Facts
Once the cryotherapy kills off cancer cells, your body’s immune system will get to work breaking them down and absorbing them. This can help encourage your immune system to look for more cancer cells around your body. Healthy tissue may grow back in the area where you had treatment.
Cryotherapy is a type of treatment for cancer that has been used by doctors for over 100 years. With the help of modern technology, it’s now one of the safest ways to treat tumors in certain areas. It only takes about an hour and can be done in a special room instead of an operating room.
A 2021 clinical research study reported that cryotherapy could control thoracic tumors with a 77% success rate for two years. Future trials are aiming to increase effectiveness up to 90% for preventing local recurrence.
Doctors use cryotherapy to treat several types of cancer, and the effectiveness for mesothelioma has been tested.
In many cases, mesothelioma cells are too widely dispersed for a localized treatment such as cryotherapy to target them all. Some oncologists maintain that when mesothelioma has spread to more than two locations, it is highly likely that the patient has many other microscopic metastases that would prevent this therapy from effectively curing the cancer.
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Before doing major surgery to take away tumors, doctors usually try to make them smaller with other cancer treatments. The two most common ones are chemotherapy and radiation, but some doctors have tried cryotherapy in clinical trials.
This is the most common period during which cryotherapy is used. Though multimodal treatment plans may be used to get rid of the tumor, sometimes it can come back months or years later.
Rather than a major surgery, doctors can use cryotherapy to treat small tumors that come back. In one study from UCLA, Dr. Fereidoun Abtin was able to control up to 95% of local recurrences at one year.
Cryotherapy can relieve the pain associated with mesothelioma by shrinking tumors that press against the lungs and other organs. Cryotherapy is valuable as a palliative treatment option because it carries a very low risk of complications or side effects.
Unlike many other cancer treatments, this therapy causes very few side effects. It is less invasive than open surgery and requires a much shorter recovery time. Most patients are able to resume their normal schedules as soon as 24 hours after the procedure is completed.
Because treatment is delivered directly to the tumors, there is little risk the healthy surrounding tissues will be damaged. One 2007 study found 81% of patients with diseases such as lung cancer, mesothelioma and colorectal cancer were treated without any damage to adjacent tissues or organs.
Rare complications after cryotherapy for recurrent pleura mesothelioma patients include a hemorrhage, collapsed lung or fluid buildup near the lung.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
