
Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your DoctorIn external beam radiation therapy, a machine outside the body shoots a beam of X-rays or charged particles at a patient’s cancer site. There are many types of external beam radiation. Specialists use the most sophisticated kinds to treat pleural mesothelioma.
External beam radiation uses high-energy beams emitted from a machine to treat cancerous tumors. EBRT is the most common type of radiation treatment for pleural mesothelioma. The machine that creates the radiation is usually a linear accelerator or Linac machine.
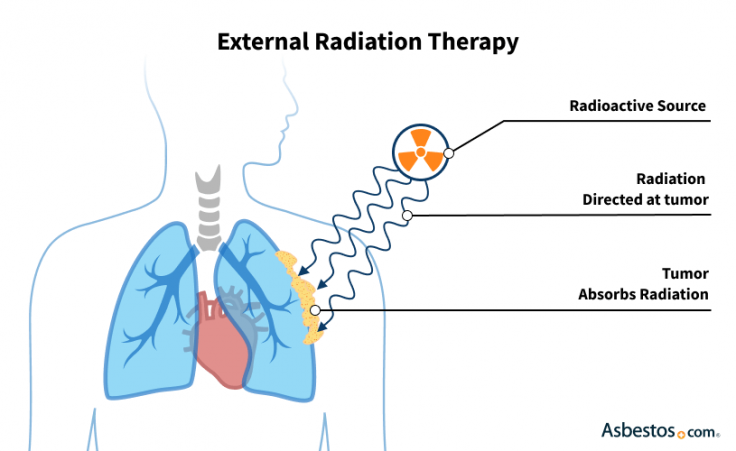
During EBRT, you lie on a table while a machine directs energy beams at your tumor. Radiation oncologists program these beams to be shaped precisely to your body and tumor, minimizing damage to healthy tissue.
EBRT is one of two main types of radiation therapy for mesothelioma and destroys mesothelioma cancer cells. The EBRT machine is set far from your body and doesn’t need to touch you to deliver radiation.
This sets EBRT apart from the second main type of radiation for mesothelioma, internal radiation therapy. IRT also destroys cancer cells, but during brachytherapy or other types of IRT, your doctor places a radioactive device inside your body near the tumor.
Types of External Beam Radiation Therapy for Mesothelioma
Pleural mesothelioma develops in the membrane on the outside of the lungs. Radiation oncologists must use unique methods to make sure they can target cancer without hurting nearby lung and heart tissue.
Radiation therapy isn’t as effective in peritoneal mesothelioma treatment. Doctors may use it to prevent surgical tools from spreading cancer cells. More substantial types of radiation treatment are too dangerous to use in the abdomen.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your DoctorProton therapy is another form of EBRT, but it isn’t yet a standard treatment for mesothelioma. Instead of using a beam of X-rays, some specialized cancer centers can use a beam of protons to kill cancer cells.
The advantage of proton therapy is that it causes much less collateral damage to healthy cells around the tumor site. Because there is less risk to the rest of the patient’s body, radiation oncologists can give the tumor site a more lethal dose of energy.

Yvette King
Survivor Overcomes Mesothelioma with Proton Therapy
After undergoing surgery in March 2016, King started radiation therapy at Maryland Proton Treatment Center. Proton therapy is one of the most specialized and precise forms of EBRT. Once she was done with her physical therapy, she began her six weeks of proton therapy at MPTC.
Yvette King
A significant benefit of EBRT is its effectiveness alongside other treatments, such as surgery, chemotherapy or immunotherapy. In aggressive multimodal treatment, doctors typically use radiation after surgery to kill cancer cells left behind.
A 2021 research study in AME Surgical Journal noted patients who received external beam radiation therapy after pleurectomy and decortication surgery had an overall survival of 13.5 months. This strategy is associated with better survival rates for patients. EBRT can also shrink tumors before surgery, which is called neoadjuvant therapy.
EBRT relieves symptoms as part of palliative care for mesothelioma. Palliative care helps mesothelioma patients manage pain and other symptoms. EBRT can shrink tumors, relieving chest pain and shortness of breath that can interfere with your daily life.
Radiation therapy has mild side effects compared to chemotherapy for pleural mesothelioma, such as nausea and skin irritation. However, doctors must be cautious when giving a patient radiation therapy in the chest, as it can easily damage the lungs and heart if doctors don’t aim it carefully.
Your health care team will work to minimize side effects, but most patients experience some adverse reactions. Side effects occur when your healthy cells receive radiation. Fatigue or tiredness is the most common side effect of EBRT. Every patient’s experience is different, and your side effects will depend on the dose and location of your treatment.
Recommended ReadingYour web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, February 9). External Beam Radiation Therapy for Mesothelioma. Asbestos.com. Retrieved May 22, 2026, from https://www.asbestos.com/treatment/radiation/external-beam-radiation-therapy/
Selby, Karen. "External Beam Radiation Therapy for Mesothelioma." Asbestos.com, 9 Feb 2026, https://www.asbestos.com/treatment/radiation/external-beam-radiation-therapy/.
Selby, Karen. "External Beam Radiation Therapy for Mesothelioma." Asbestos.com. Last modified February 9, 2026. https://www.asbestos.com/treatment/radiation/external-beam-radiation-therapy/.

Dr. William Breen is an innovative radiation oncologist in Rochester, Minnesota, at the much-acclaimed Mayo Clinic, a National Cancer Institute-designated Comprehensive Cancer Center for more than 40 years.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
