Based on Your Reading:
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Pericardial mesothelioma is a very rare cancer that forms in the pericardium, or lining, of the heart. Tumors in the heart are very rare. Cardiac (heart) tumors are often caused by metastasis.
Written by Sean Marchese, MS, RN • Edited By Walter Pacheco
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Marchese, S. (2024, February 2). Pericardial Mesothelioma. Asbestos.com. Retrieved April 24, 2024, from https://www.asbestos.com/mesothelioma/pericardial/
Marchese, Sean. "Pericardial Mesothelioma." Asbestos.com, 2 Feb 2024, https://www.asbestos.com/mesothelioma/pericardial/.
Marchese, Sean. "Pericardial Mesothelioma." Asbestos.com. Last modified February 2, 2024. https://www.asbestos.com/mesothelioma/pericardial/.
Pericardial mesothelioma is a rare cancer affecting the heart’s lining, called the pericardium. Less than 1% of all types of mesothelioma are pericardial.
Asbestos exposure causes mesothelioma cancer. The link between asbestos and pericardial cancer is still under investigation. Researchers are working to understand how asbestos fibers reach the heart.
This cancer usually affects people between 50 and 70 years of age. It also occurs in men more often than women. Symptoms appear at a later stage and can mimic other heart disorders. These can include chest pain, fatigue and shortness of breath. Diagnosis is challenging due to these similar symptoms.
Pericardial treatment options include surgery and chemotherapy. Some patients elect no treatment. Only a few patients receive radiation therapy. This treatment carries a higher risk near the heart.
Fewer than 150 cases of pericardial mesothelioma exist in medical literature. A 2023 research report notes that median survival is about 2 to 6 months. Survival rates are low, but some patients can live years after surgery or chemotherapy.
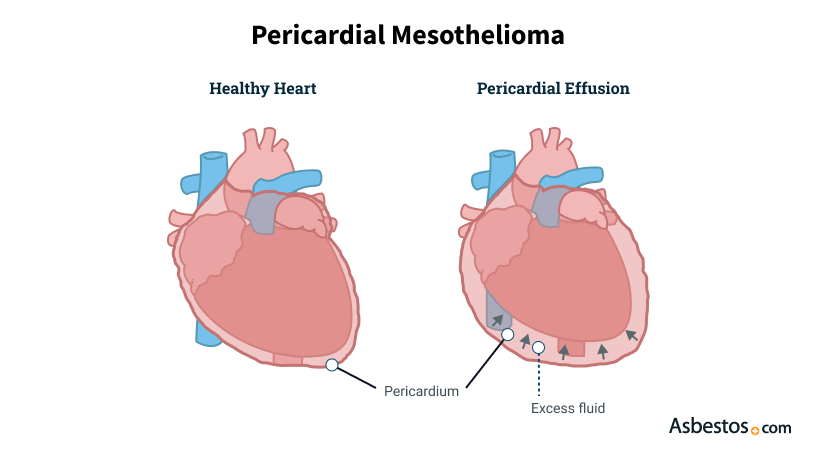
Common pericardial symptoms include difficulty breathing, chest pain and heart palpitations. Fluid buildup around the heart and thickening of the pericardial layers cause symptoms.
Most pericardial mesothelioma patients experience no symptoms at first. This fact contributes to a late-stage diagnosis. The signs of pericardial mesothelioma can also resemble those of other heart conditions. This makes it difficult to diagnose.
Recommended tests include an X-ray, CT scan or echocardiogram (heart ultrasound).
If you are experiencing symptoms, schedule an appointment with your doctor immediately. Screening tests can reveal the underlying cause of these health problems.
Get Your Free Mesothelioma Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

A physical examination and imaging tests can diagnose the location of pericardial mesothelioma tumors. A biopsy can confirm whether they are cancerous.
Doctors will also assess your symptoms, medical history and current medical condition. They use this information, along with biopsy results, to determine treatment.
Pericardial tumors generally are not localized. They tend to cover most of the heart. This cancer type accounts for approximately half of all pericardial tumors.
It’s essential to meet with a specialist to confirm your diagnosis. An expert will know the intricacies of this rare cancer. They can ensure an accurate diagnosis and prompt treatment.
If you have been diagnosed with any of these conditions, always seek a specialist. They have the experience to confirm the diagnosis. These experts provide new therapies and clinical trials that may improve survival. Working with a specialist may also give you access to a broader range of treatment options.

Mesothelioma treatment for pericardial mesothelioma includes surgery and chemotherapy. The heart lining rests close to the heart and limits treatment options.
Surgery is the most effective treatment for this cancer, but more than half of patients are not eligible. In rare cases of an early diagnosis, surgery may be able to remove small, localized tumors. The primary surgical treatment options for pericardial mesothelioma are pericardiectomy and tumor removal.
Chemotherapy and palliative treatment, such as fine needle aspiration, can ease symptoms and slow growth. Radiation therapy is considered minimally beneficial for this rare cancer. It is risky to administer without harming the heart.
Patients who are good candidates for surgery may undergo a pericardiectomy or tumor removal. A pericardiectomy removes part or all of the pericardium. This surgery relieves pressure and minimizes fluid buildup.
Tumor removal, or tumor resection, removes cancer without removing the pericardium. A 2017 review reported more prolonged survival with tumor removal than a pericardiectomy.
The benefits of chemotherapy are minimal for most patients with pericardial mesothelioma. The chemotherapy drugs pemetrexed and cisplatin may improve survival. Gemcitabine has produced mixed results.
A handful of cases have responded well to chemotherapy. One woman lived longer than two years thanks to the chemo drugs cisplatin, gemcitabine and vinorelbine.
Fluid buildup in the pericardium is the primary cause of symptoms. Palliative treatment options aim to minimize pain and reduce symptoms. This type of care can improve quality of life and make patients more comfortable.
A pericardiocentesis removes excess fluid to relieve pain and pressure around the heart. Pain medication can also reduce symptoms and improve comfort.
The prognosis for pericardial mesothelioma is poor compared to peritoneal or pleural mesothelioma. Nearly 50% to 60% of pericardial patients die within six months of diagnosis. However, this is not the case for everyone. Over 20% of patients live for one year or more. The 5-year survival rate for pericardial mesothelioma is 9%.
Hope exists for some patients because researchers have cited positive results from surgery. Smaller, less impactful benefits have been demonstrated from chemotherapy, except for one case. A 47-year-old woman lived two years after chemotherapy with cisplatin, gemcitabine and vinorelbine.
A 1995 case report of a 27-year-old woman who underwent surgery and radiation therapy for pericardial mesothelioma states that she had no evidence of recurrence during 28 years of follow-up.
Surgery to remove part of the heart’s lining combined with radiation therapy improved survival in two patients in the late 1960s and early 1970s. One patient lived a year after treatment, and another was alive five years after treatment.
Several informational resources are available for patients diagnosed with pericardial mesothelioma. These resources can help patients better understand their condition and treatment options. They can also help them cope with the disease’s physical and emotional challenges. Available support resources include:
Coping with pericardial mesothelioma can be challenging. Effective coping strategies can manage symptoms and improve quality of life. Some helpful tips include:
Pericardial mesothelioma can be challenging, but many resources are available. Take advantage of these resources. Practice self-care, stay organized and seek emotional support as needed.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
