
Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistPeritoneal mesothelioma is a rare cancer caused by asbestos exposure that forms in the peritoneum, the tissue lining the abdomen. It's the second most common type of mesothelioma. With today's treatments, about 65% of patients live 5 years or more.

Expert Take
Dr. Charles Conway: Differences Between Peritoneal & Pleural Mesothelioma

Expert Take
Dr. Charles Conway: Differences Between Peritoneal & Pleural Mesothelioma
“The best treatment for peritoneal mesothelioma is a combination of HIPEC and pressurized intraperitoneal aerosolized chemotherapy, also known as PIPAC, which differs from traditional chemo because it uses pressure to turn the chemo drugs into a mist to reach the abdominal area better.”

Dr. Catherine Perrault, medical officer and board-certified family physician with our Medical Outreach Team
“Peritoneal mesothelioma is different than pleural mesothelioma essentially because it's just a different site in the body. It's a cancer that comes from the same cell of origin, the mesothelium cell. You can get cancer from really any cell in your body. You can get cancer in bone cells, fat cells, muscle cells.”

Dr. W. Charles Conway, director of surgical oncology at the Ridley-Tree Cancer Center
“When I was first told I had peritoneal mesothelioma, I pictured the day when I would be cancer free. It gave me something to look forward to. According to recent studies, the average mesothelioma life expectancy is 12 to 21 months, and here I am, 14 years later. It’s very rare for a peritoneal mesothelioma patient to live this long. Therefore, getting to cancer remission for me was a goal I was well intending to reach. And I did.”

Tamron Little, peritoneal mesothelioma survivor
“The best treatment for peritoneal mesothelioma is a combination of HIPEC and pressurized intraperitoneal aerosolized chemotherapy, also known as PIPAC, which differs from traditional chemo because it uses pressure to turn the chemo drugs into a mist to reach the abdominal area better.”

Dr. Catherine Perrault, medical officer and board-certified family physician with our Medical Outreach Team
“Peritoneal mesothelioma is different than pleural mesothelioma essentially because it's just a different site in the body. It's a cancer that comes from the same cell of origin, the mesothelium cell. You can get cancer from really any cell in your body. You can get cancer in bone cells, fat cells, muscle cells.”

Dr. W. Charles Conway, director of surgical oncology at the Ridley-Tree Cancer Center
“When I was first told I had peritoneal mesothelioma, I pictured the day when I would be cancer free. It gave me something to look forward to. According to recent studies, the average mesothelioma life expectancy is 12 to 21 months, and here I am, 14 years later. It’s very rare for a peritoneal mesothelioma patient to live this long. Therefore, getting to cancer remission for me was a goal I was well intending to reach. And I did.”

Tamron Little, peritoneal mesothelioma survivor
Peritoneal mesothelioma, also called abdominal mesothelioma, is a rare asbestos-related cancer that forms in the peritoneum. The peritoneum is the thin tissue lining the abdominal cavity and organs in your belly. Irritation from asbestos exposure causes mesothelioma tumors to grow in this lining.
Irritation from asbestos exposure is the primary cause. The most common symptoms of peritoneal mesothelioma are stomach pain, swelling, digestive problems and weight loss. Treatments include surgery, chemotherapy or immunotherapy to help control the disease and improve quality of life. Patients can improve their symptoms and prognosis with treatments like HIPEC, a combination of surgery and heated chemotherapy.
Several cancers affect the abdominal cavity, but peritoneal mesothelioma isn’t the same as ovarian, colorectal or appendiceal cancer. Those cancers spread to the peritoneum from other parts of the body. Peritoneal mesothelioma starts in the peritoneal lining and requires a different treatment approach.
Peritoneal mesothelioma shares many symptoms with other abdominal cancers. Ascites, abdominal pain and bloating all appear in several conditions. CT scans and imaging tests can look nearly identical across these diagnoses. This overlap makes peritoneal mesothelioma one of the most commonly misdiagnosed cancers. Multiple peer-reviewed case reports confirm that peritoneal mesothelioma initially presented as ovarian cancer, where tissue biopsy later corrected the diagnosis.
Doctors may also struggle to distinguish peritoneal mesothelioma from ovarian cancer in women because both conditions affect the same region and share symptom profiles. In men, doctors sometimes mistake it for colorectal or appendiceal cancer that has spread to the peritoneum.
A tissue biopsy is the only reliable way to confirm a peritoneal mesothelioma diagnosis. Pathologists use a panel of immunohistochemical markers, specific proteins that appear in mesothelioma cells but not in other cancer cells, to distinguish peritoneal mesothelioma from ovarian, colorectal and appendiceal cancers. No single marker confirms mesothelioma on its own. Doctors use a combination of positive mesothelioma markers and negative carcinoma markers to reach an accurate diagnosis.
Getting the right diagnosis matters. Each cancer has a different treatment plan. A misdiagnosis can delay the right care and affect outcomes. If you have a history of asbestos exposure and received an abdominal cancer diagnosis, ask your doctor about getting a second opinion from a peritoneal mesothelioma specialist.
See a doctor if you have persistent abdominal pain, bloating or unexplained digestive issues. If you have a history of asbestos exposure, consider seeing a mesothelioma specialist for evaluation.
Common symptoms of peritoneal mesothelioma include abdominal pain, bloating and fluid buildup. Fluid in the belly puts pressure on internal organs, causing pain and discomfort. Early-stage mesothelioma affects the digestive system, including changes in bowel habits. Other signs of mesothelioma are weight loss or fever. Most symptoms appear in later stages of the disease.
Epifanio Figueroa tells us his first sign of peritoneal mesothelioma was abdominal swelling. He shares, “It started with my stomach growing, and it didn’t stop getting bigger. It was liquid that was being accumulated. It was from mesothelioma, but we didn’t know that at the time.”
Early Symptoms (most common at presentation):
Late-Stage Symptoms (appear as disease progresses):
Late-stage mesothelioma usually includes significant abdominal pain, fluid buildup, weight loss, fatigue, nausea and vomiting. A 2023 report in Radiology Case Reports also discussed the risk of bowel obstruction with peritoneal mesothelioma. Rare and severe symptoms include, blood clots and fluid buildup in other places such as around the lungs (pleural effusion) or sac around the heart (pericardial effusion).
Our annual and exclusive 2025 State of Mesothelioma report reflected the same common peritoneal symptoms among more than 200 patients, doctors, survivors and caregivers surveyed. Fatigue and weight loss were the most common peritoneal symptoms reported among men and women with mesothelioma.
| Symptom | Percentage of Males | Percentage of Females |
|---|---|---|
| Abdominal Pain | 68% | 74% |
| Fatigue | 75% | 80% |
| Weakness | 62% | 66% |
| Loss of appetite | 54% | 60% |
| Unexplained weight loss | 60% | 65% |
| Bowel obstruction | 38% | 42% |
| Fever | 27% | 33% |
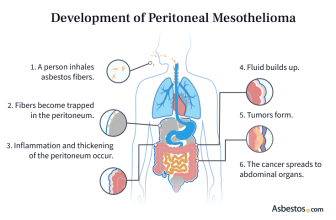
The main cause of peritoneal mesothelioma is breathing in or swallowing asbestos fibers.
These tiny fibers can travel into the belly and get stuck in the peritoneum. After 20 to 60 years, they can cause irritation and damage that may lead to cancer. This slow process is called the latency period, and it can take many years to happen.
If you have a history of asbestos exposure, let your doctor know, as you could be at a higher risk of developing peritoneal or pleural mesothelioma. Your doctor may recommend regular mesothelioma screenings for you.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistExposure to asbestos is the largest risk factor for peritoneal mesothelioma. Most people are exposed to asbestos at work. Duration and intensity of the exposure play a key role in the likelihood of the disease developing. There is no safe level of asbestos exposure. Even short-term exposure isn’t safe.
Common Risk Factors for Peritoneal Mesothelioma
Asbestos exposure can also occur from contaminated talcum powder. Talc is often mined next to naturally occurring asbestos, which can lead to contaminated talc products such as baby powder, a cause of increased mesothelioma rates in women.
We spoke to mesothelioma survivor James D. about his peritoneal mesothelioma. He told us the exposure happened while working as a mechanic in Chicago. Many survivors also tell us they were exposed to asbestos while serving in the U.S. Armed Forces.
Family members of workers can face secondary asbestos exposure when fibers are brought home on clothing, hair, or skin. Everyday activities such as doing laundry, hugging a loved one, or handling contaminated gear can release asbestos fibers and increase risk.
A biopsy is the only test that can confirm a peritoneal mesothelioma diagnosis. Imaging and blood tests may suggest disease, but diagnosis always requires a tissue sample examined by a pathologist. The diagnostic process usually begins with a physical exam where your doctor will feel for any abnormalities in your belly. Imaging tests like X-rays and blood tests may then be ordered.
A small sample of tissue from your biopsy is sent to a pathologist. The pathologist will then look at the tissue under a microscope to see if mesothelioma cells are present and to confirm your mesothelioma diagnosis. The specific type of mesothelioma cells found will also be included in your pathology report. Mesothelioma cells include: epithelioid, sarcomatoid or biphasic (a mix of both). Each cell type grows and spreads differently, so knowing this helps your doctor choose treatments most likely to work best for you.
Diagnostic Tests for Peritoneal Mesothelioma
Dr. Anton Strocel, who treated Trina Reif, a 20-year survivor of peritoneal mesothelioma, tells us, “She presented to me with unexplained ascites.” Ascites is the buildup of excess fluid in the belly. Trina then had an exploratory laparotomy and peritoneal biopsies before her diagnosis was confirmed.
Finding peritoneal mesothelioma early is important but often hard. Symptoms can take 20 to 60 years after exposure to appear and when they do, they can look like signs of other common illnesses.

Survivor Story
Epifanio Figueroa: Walk us through your peritoneal mesothelioma diagnosis and treatment
Peritoneal mesothelioma staging shows how far the disease has spread. The Peritoneal Cancer Index is the system most used to stage peritoneal mesothelioma. PCI measures the size and spread of tumors in the abdomen. This information can help determine treatment options.
In stage 1, or early-stage peritoneal mesothelioma, the cancerous tissue is small. Tumors are only within the abdominal lining, and lymph nodes are free of cancer. In stage 2, or mid-stage peritoneal mesothelioma, cancerous tissue is moderate. Tumors haven’t spread outside the lining or into lymph nodes. The cancerous tissue spreads more widely during stages 3 and 4, or late-stage mesothelioma.
Peritoneal surgeon Dr. Mohamed Abdelgadir Adam at the University of California San Francisco and other researchers announced in 2026 that they are proposing a new way of staging peritoneal mesothelioma. The new approach uses a “survival tree” model. It analyzes which combinations of tumor characteristics most strongly predict patient survival. Patients within each stage have more similar outcomes, making it easier for doctors to explain what to expect and how to plan appropriate treatment.
Common peritoneal mesothelioma treatment options include surgery, chemotherapy (often HIPEC) and emerging therapies like immunotherapy. Your doctor might suggest a treatment plan that combines several therapies.
Common Peritoneal Mesothelioma Treatments
Talk to your doctor about which treatments fit your diagnosis and overall health. A specialist at a high-volume peritoneal mesothelioma center can help you understand all your options.
This study examines whether intraperitoneal or intravenous chemotherapy given after cytoreductive surgery and HIPEC are effective treatments for peritoneal mesothelioma.
This phase 2 trial compares the usual treatment alone to using immunotherapy plus the usual treatment in treating patients with peritoneal mesothelioma.
Cytoreductive surgery combined with HIPEC is the most effective treatment for eligible patients with peritoneal mesothelioma. The procedure works in 2 steps. First, surgeons remove as much visible tumor as possible. Then, they circulate heated chemo drugs directly inside the abdomen for 1 to 2 hours to destroy any remaining cancer cells.
Multiple studies show that patients who receive CRS+HIPEC live significantly longer than those who receive chemo alone. Patients who don’t qualify for surgery live an average of 13 months with chemo. Research consistently shows that patients who achieve complete tumor removal during CRS have significantly better outcomes.
Not every person with peritoneal mesothelioma qualifies for CRS+HIPEC. Doctors consider several factors when evaluating eligibility.
Factors to Consider for CRS + HIPEC
A specialist at a high-volume peritoneal mesothelioma center will assess these factors. If you don’t qualify for surgery right away, neoadjuvant therapy (treatment before surgery) may help reduce tumor size enough to make CRS+HIPEC possible.

Get answers about treatment, top doctors, and clinical trials from the nation’s most trusted mesothelioma resource.
Get Your Free GuideThe most common drugs doctors use during HIPEC for peritoneal mesothelioma are cisplatin, mitomycin C (MMC) or a combination of cisplatin and doxorubicin. Your doctor will recommend the regimen that best fits your health profile and tumor characteristics.
Your treatment path depends on your health, stage and tumor characteristics. Here’s a simple overview.
Choosing Your Treatment
Dr. Joseph Skitzki, a surgical oncologist at Roswell Park Comprehensive Cancer Center, regularly performs HIPEC for his peritoneal mesothelioma patients. He tells us, “The results are quite impressive. About 80% of patients who are eligible for the treatment will be alive at 5 years, and about half of that number without any further evidence of disease.”
No matter where you fall on this list, you don’t have to make these decisions alone. Your doctor and our Patient Advocates can help you find clinical trials that are actively enrolling and may offer new options for your specific diagnosis.
Choosing a top mesothelioma treatment center can help you get better results. These centers often offer clinical trials and understand the unique challenges of this rare cancer to provide support for you and your family. Our team of Patient Advocates can also connect you with the right specialist and cancer center.

Tammy Frank
20-Year Peritoneal Mesothelioma Survivor Celebrates Life
20-Year Peritoneal Mesothelioma Survivor Celebrates Life Tammy Frank was diagnosed with peritoneal mesothelioma in 1999. After undergoing surgery, radiation and chemo, she has become a 20+ year survivor. Tammy credits her longevity to early treatment and a deep sense of purpose.
Tammy Frank
The average life expectancy for peritoneal mesothelioma is about 31 months from diagnosis with today’s treatments. Patients without treatment have a life expectancy of 6 to 8 months.
This is significantly longer than the average for pleural mesothelioma, which is the most common type of this cancer and develops in the lining of the lungs. Treatment options and prompt treatment of peritoneal mesothelioma can affect your outlook or prognosis. Early detection and HIPEC surgery boost survival rates.
Early detection significantly improves outcomes. People with peritoneal mesothelioma who don’t qualify for surgery live about 13 months with chemotherapy alone. Adopting healthy habits and new treatments may extend life expectancy.
Age, gender, genetics, stage, cell type and tumor location all affect prognosis. Women, for example, often have longer survival rates. However, statistics are based on large groups and can’t predict individual outcomes. Many factors affect your prognosis, and new breakthroughs continue to improve survival. Always discuss your specific case with a mesothelioma specialist.
| Treatment Approach | 5-Year Survival Rate | Average Life Expectancy |
|---|---|---|
| Cytoreductive surgery + chemotherapy | 75% | Varies by patient |
| Overall with treatment | 65% | 31 months |
| HIPEC surgery | More than 50% | Varies by patient |
| Chemotherapy alone (nonsurgical candidate) | Lower than with surgery | 13 months |
| No treatment | Very low | 6 to 8 months |
Living with peritoneal mesothelioma takes physical and emotional strength. A solid support system of family, friends and health care providers can make a big difference. Rest, proper nutrition and gentle movement can help you feel your best.
Peritoneal mesothelioma and its treatments can affect how your body absorbs nutrients. Working with an oncology dietitian can help you build a nutrition plan that fits your specific treatment. Asbestos.com offers a free Mesothelioma Nutrition Guide with tips from a registered nurse on what a survivor’s diet can include.
Good nutrition helps your body handle treatment and supports recovery. Protein helps preserve muscle and repair tissue after surgery, chemo or radiation. Aim for high-protein foods like chicken, fish, eggs, dairy and beans. Eat colorful fruits and vegetables to support immune function. Avoid processed meats, fried foods and alcohol, as these can increase inflammation and interfere with treatment.
Peritoneal mesothelioma patients who undergo CRS+HIPEC often face digestive challenges after surgery. Reintroduce foods slowly and work closely with your care team during recovery. Some patients need to adjust their fiber intake or follow a temporary modified diet until their digestive system heals. Always talk to your doctor before making major dietary changes.
Light activity like walking, gentle stretching or yoga can reduce fatigue, improve mood and support recovery. Start slowly and increase intensity only with your doctor’s guidance. Break exercise into shorter sessions if energy runs low. Many peritoneal mesothelioma survivors stay active through modified hobbies like swimming or cycling.
If you need to travel for treatment, plan ahead. Bring a complete copy of your medical records and a list of your current medications. Ask your care team about managing symptoms and treatment schedules around travel. Our Patient Advocates can help you arrange care at a top mesothelioma treatment center near home.
Caregivers play a vital role in the peritoneal mesothelioma journey. The physical and emotional demands of caregiving can feel overwhelming. It’s important to ask for help and share responsibilities among family members when possible. Volunteer groups can provide meals and daily support, and your care team may know of local respite care resources.
The Mesothelioma Center hosts a private Mesothelioma Facebook Support Group. This group connects caregivers with others who understand what they’re going through. It’s a safe space to share experiences, ask questions and find practical support.
The Mesothelioma Center also hosts a monthly online support group for peritoneal mesothelioma patients and caregivers. A licensed mental health counselor and registered nurse lead each session.
Collaborating with your medical team helps you get the right care. Connecting with others who share your experience can ease the emotional weight of your diagnosis and help you find strength along the way.
There is no cure for malignant peritoneal mesothelioma. But it can go into remission. About 12% of peritoneal mesothelioma patients who get aggressive treatment have complete remission. Partial remission is also possible. Remission isn’t the same as a cure. Doctors watch patients closely. Cancer can return after remission.
Effective communication with your doctor is key. Preparing questions ahead of time helps you make the most of your appointment.
Writing down your questions also ensures you don’t forget important topics during the appointment. This approach helps you communicate effectively with care providers and gives you more control over your diagnosis and treatment.
Inherited genetics don’t account for the majority of cases. Some gene changes, like BAP1, are uncommon but increase risk in certain families. If you notice BAP1 in multiple family members with mesothelioma or related cancers, consult your doctor about genetic counseling and testing. Results may help your doctors in treatment planning.
Costs differ depending on the hospital, surgeon and whether or not you get CRS-HIPEC which requires an extended hospital stay. Insurance, travel, missed days of work and follow up care make the cumulative total even higher. It’s best to request a written price expectation from your surgical team for insurance pre-authorization. Financial counselors and Patient Advocates can help with resources like grants and lodging or travel amenities.
It generally develops in the peritoneal cavity and can involve adjacent organs, the omentum and lymph nodes. In more advanced situations, it can extend into the chest or other distant areas, but this is less frequent.
Early intervention from specialists can manage and stabilize the disease, reducing progression and increasing quality of life. Report new onset abdominal pain, abdominal swelling, respiratory difficulty and unintended weight changes to your provider as soon as possible.
About 65% of patients with peritoneal mesothelioma live 5 years or more with treatment. Among patients who qualify for CRS+HIPEC surgery, about 80% are alive at 5 years. Without treatment, life expectancy is 6 to 8 months. Individual outcomes vary based on stage, cell type, age and overall health.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Asbestos.com. (2026, May 29). Peritoneal Mesothelioma. Retrieved June 1, 2026, from https://www.asbestos.com/mesothelioma/peritoneal/
"Peritoneal Mesothelioma." Asbestos.com, 29 May 2026, https://www.asbestos.com/mesothelioma/peritoneal/.
Asbestos.com. "Peritoneal Mesothelioma." Last modified May 29, 2026. https://www.asbestos.com/mesothelioma/peritoneal/.
We Thoroughly vet individuals who are experts in their field to contribute to articles on Asbestos.com. We believe in the integrity and quality of our educational materials, and only publish information that is relevant, factual, and backed by experts.

Karen Selby is a registered nurse and Board Certified Patient Advocate at The Mesothelioma Center with more than 30 years of experience in oncology and thoracic surgery. She worked as an operating room nurse in thoracic surgery at the University of Maryland for 6 years, assisting with surgeries such as lung transplants, pneumonectomies and pleurectomies. She later served as regional director of the tissue procurement program at the University of Florida. Karen joined The Mesothelioma Center in 2009, providing patients with personalized support and resources.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
