
Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
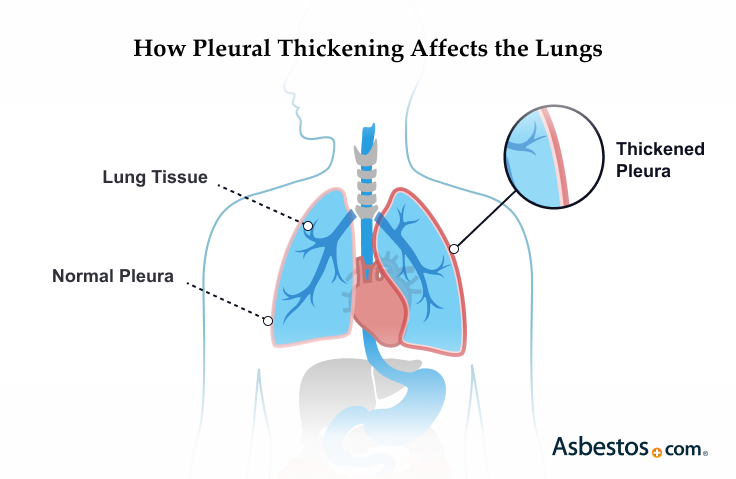
Find Your SpecialistPleural thickening is scarring of the pleura, the thin membrane that lines the lungs and chest wall. This can happen after asbestos exposure, injury or infection. It isn't cancer, but may be an early sign of mesothelioma. Treatment can't cure it, but can ease symptoms and help you feel better.
Pleural thickening isn’t cancer, but it can appear alongside conditions like pleural mesothelioma or, in some cases, before it, so doctors monitor it closely. Asbestos can cause both pleural thickening and mesothelioma. If you have pleural thickening, see your doctor often. In some people, it gets worse and leads to more serious illness.
Key Facts About Pleural Thickening
Recent studies show finding pleural thickening early can lead to better care. Registered Nurse Sean Marchese says, “It can help find mesothelioma sooner. This means more ways to treat it and feel better.”
In pleural mesothelioma, pleural thickening is usually diffuse or focal. These terms describe how much of the lining is affected. The thickening can be noncancerous, cancerous or another type.
Each type affects the lungs differently. That changes how doctors treat it and what to expect.
Main Types of Pleural Thickening
Knowing what caused the thickening helps doctors plan care. They keep a close eye on both types to protect your lungs and catch signs of cancer early.
Diffuse pleural thickening means a large area of the lungs’ lining has scarring. This can make it harder to breathe. This type is strongly linked to heavy asbestos exposure.
Diffuse Pleural Thickening Types
Doctors recommend people with diffuse thickening regularly track their lung health. Without care, this condition could lead to pleural mesothelioma.
Focal pleural thickening means scarring in one small area of the lungs’ lining. It can happen after minor asbestos exposure or past infections. While it’s usually less serious, doctors still need to watch it closely.
Focal Pleural Thickening Types
Imaging scans can help find this condition early. Early care may lower the risk of more serious lung problems like mesothelioma.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistThe main cause of pleural thickening is breathing in asbestos. Other causes include infections or chest injuries. Asbestos dust has tiny fibers that can get stuck in the lining of the lungs. Over time, these fibers cause irritation and scarring. This scar tissue can build up and lead to pleural thickening.
Causes of Pleural Thickening
Discuss your risk for pleural thickening with your doctor. If you have a history of asbestos exposure, ask about regular screenings.
A classic study in the Journal of Occupational Medicine and Toxicology looked at asbestos. Some workers were found to have pleural thickening after exposure to the mineral. It developed in 5% to 13.5% of workers, often 3 to 34 years after their first exposure.
The most common symptoms of pleural thickening are breathlessness, chest pain and coughing. Symptoms usually develop slowly and can be hard to notice at first. Catching these signs early can lead to better care and outcomes.
Common Pleural Thickening Symptoms
Anyone with lasting breathing problems or chest discomfort should talk to a doctor. Regular screenings are crucial for preventing asbestos-related diseases. This is especially critical for those with known asbestos exposure.
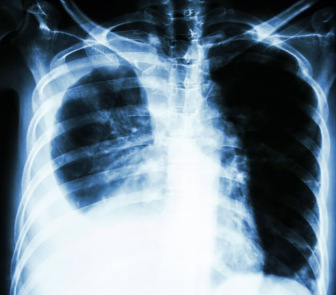
Doctors use X-rays, CT scans and MRIs to look for pleural thickening. Finding it early can help guide better treatment and improve outcomes.
They may also run tests to rule out other conditions like pleural plaques and pleural effusion. A pleural effusion is fluid buildup in the pleural space, and it can worsen shortness of breath. Pleural plaques are small, flat spots on the outside of the lungs, while pleural thickening is more widespread scarring that can make the lungs stiff. Doctors also check for signs of asbestos cancers, like pleural mesothelioma.
Telling your doctor about any asbestos exposure helps with a clear diagnosis. If you’re unsure about your diagnosis, getting a second opinion is always an option.
A biopsy removes a small piece of tissue from the lining of the lungs. Doctors look at it under a microscope to find out what’s causing the thickening.
Your doctor may use a needle or a small camera (thoracoscopy) depending on where the thickening is. The results help confirm a diagnosis and guide the best treatment plan for you. Recent research suggests CT-guided biopsies are also a safe and effective option for collecting pleural tissue.
Doctors use the same imaging scans for pleural thickening and mesothelioma. A CT scan of the chest is the most useful imaging test for showing the location and extent of pleural thickening. On chest X-rays, pleural thickening shows as a thick white line along the lung’s edge. PET scans and MRIs help tell pleural thickening apart from mesothelioma.
CT scans provide detailed images that help doctors map the thickening and plan next steps. These scans help catch problems early so treatment can start sooner.
Pam McWhorter shares with us how imaging scans that found pleural thickening eventually led to her husband’s pleural mesothelioma diagnosis. She tells us that after an X-ray, “They noted on his medical records that there was thickening on the outside of the left lung.” Then he had a CT scan. Pam tells us the CT scan report said, “‘Nodular thickening, suspect for mesothelioma, doctors should take immediate action.’”

Jim McWhorter
Pleural Thickening Was a Sign of Survivor’s Mesothelioma Journey to Come
Jim McWhorter was told an injury-prompted X-ray was clear, but pleural thickening was noted in his record. A later surgery found tumors. It turns out that the pleural thickening led to his pleural mesothelioma diagnosis.
Jim McWhorter
There is no cure for pleural thickening. But supportive treatment can help manage it. The best options are to quit smoking, stay active and do rehab.
Treatments That Ease Pleural Thickening
In severe cases, surgery such as P/D may remove scar tissue to help the lung expand more easily. People with severe breathing issues may use portable oxygen tanks.
Pulmonologists and pleural specialists have the expertise to diagnose and treat pleural thickening. They can recommend follow-up care and watch your condition for signs of progression.
Our Patient Advocates can match you with a top specialist near you. Our team has been helping people find doctors since 2006.

Wickii Thambiah Vigneswaran
Pleural Specialist | Thoracic Surgery
Dr. Wickii Vigneswaran is an internationally renowned thoracic surgeon who specializes in pleural mesothelioma and other diseases of the chest. He is double board certified in thoracic and cardiac surgery, an expert in robotic surgery and has more than 30 years of experience treating mesothelioma.
Read Bio
Jeffrey Velotta
Pleural Specialist | Thoracic Surgery
Dr. Jeffrey Velotta is a thoracic surgeon at Kaiser Permanente Oakland Medical Center, serving pleural mesothelioma patients on the West Coast. He is board certified in general, thoracic and cardiac surgery, and he trained under renowned mesothelioma specialist Dr. David Sugarbaker.
Read Bio
Raja Michael Flores
Pleural Specialist | Thoracic Surgery
Dr. Raja Michael Flores is a professor and chairman of the Department of Thoracic Surgery at Mount Sinai Medical Center in New York City. Flores is a widely respected expert in pleural mesothelioma and is a recognized leader in the field of thoracic surgery for pioneering video-assisted surgical techniques for lung cancer and mesothelioma.
Read Bio
Jacques Fontaine
Pleural Specialist | Thoracic Surgery
Dr. Jacques Fontaine is the Director of the Mesothelioma Research and Treatment Center at Moffitt Cancer Center in Tampa, Florida. He specializes in minimally invasive thoracic surgery including robotic surgery. Fontaine became a pleural mesothelioma specialist while studying under Dr. Sugarbaker at the International Mesothelioma Program at Brigham & Women’s Hospital.
Read BioIf you need assistance finding a pleural specialist, our Patient Advocates at The Mesothelioma Center can match you with a top doctor near you. Our team of Patient Advocates has been helping patients find doctors since 2006.
Asbestos is the primary cause of pleural thickening. Some data indicates a correlation between smoking and the progression of pleural thickening. Smoking limits lung function. It’s also proven to be a cause of other respiratory diseases, such as lung cancer.
In most cases, pleural thickening won’t affect lifespan. But this condition may be a sign of more serious underlying conditions. These include malignant pleural mesothelioma or other cancer. Your doctor will determine how serious your pleural thickening is with diagnostic tests.
Yes, Miller v. Armstrong World Industries, Inc. in 1991 was a precedent-setting court case. Raymond Miller was an insulator who worked with asbestos products. He eventually developed pleural thickening. There is now an asbestos trust fund, the Armstrong World Industries Asbestos Trust. It accepts claims from people who were exposed to the company’s asbestos products. and became ill.
Pleural thickening is not always a serious condition. But if it’s left untreated, it can advance into other, more dangerous stages such as encasement of the lung. This condition causes restrictive lung disease. Pleural thickening is also a sign of significant asbestos exposure. Pleural mesothelioma’s main cause is asbestos exposure.
Benign pleural thickening means cancer tumors did not lead to the thickened tissue. Fibrous tissue that builds on top of itself is the cause. Pleural mesothelioma or cancer that spreads from another location causes malignant pleural thickening
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, February 13). Pleural Thickening and Asbestos. Asbestos.com. Retrieved May 6, 2026, from https://www.asbestos.com/mesothelioma/pleural-thickening/
Selby, Karen. "Pleural Thickening and Asbestos." Asbestos.com, 13 Feb 2026, https://www.asbestos.com/mesothelioma/pleural-thickening/.
Selby, Karen. "Pleural Thickening and Asbestos." Asbestos.com. Last modified February 13, 2026. https://www.asbestos.com/mesothelioma/pleural-thickening/.

Dr. Wickii Vigneswaran is a thoracic surgeon at James A. Haley Veterans' Hospital in Tampa, Florida. He is also a professor at the University of South Florida Morsani College of Medicine. Vigneswaran is an internationally recognized expert in the surgical management of diseases affecting the lungs, mediastinum and pleura. He is the former director of the Lung and Lung-Heart Transplantation team at the University of Chicago Medical Center.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
