
Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuidePleural mesothelioma, also called malignant pleural mesothelioma, is a rare cancer of the lung lining. Asbestos is the primary cause. Symptoms may include chest pain, shortness of breath and fluid buildup in the chest. Though prognosis is often poor, new treatments may improve survival.

Expert Take
Dr. Jacques Fontaine: What is pleural mesothelioma?

Expert Take
Dr. Jacques Fontaine: What is pleural mesothelioma?
“With pleural mesothelioma, it’s critical to find a specialist who has knowledge of the disease and the treatment and expertise in this field. Finding the right specialist and a Center of Excellence will give patients access to the full array of treatment options and options for clinical trials, which will provide more treatment options.”

Dr. Catherine Perrault, medical officer and board-certified family physician with The Mesothelioma Center’s Medical Outreach Team
“Mesothelioma is a cancer that arises from exposure to asbestos. And asbestos are little fibers. And these fibers are inhaled, and they go through our nose and our windpipe and go into the lung. And then they go to the periphery of the lung. And then on the periphery of the lung, the lining of the lung called the pleura, they can start causing inflammation.”

Dr. Jacques Fontaine, director of the Mesothelioma Research and Treatment Center at Moffitt Cancer Center
“I said to Dr. Sugarbaker, ‘Doctor, I want you to get everything you can see, everywhere you think it might be hiding and everywhere you think it might go.’ …As it has turned out, the EPP with HITHOC followed by 4 rounds of chemo was not the end of my treatment journey, but rather only the beginning. However, whatever may have occurred since, I believe that the aggressive treatment I had in the beginning was absolutely necessary to give me a chance to be here now, and I am grateful for the decision that we made.”

Michael Cole, 11-year pleural mesothelioma survivor
“With pleural mesothelioma, it’s critical to find a specialist who has knowledge of the disease and the treatment and expertise in this field. Finding the right specialist and a Center of Excellence will give patients access to the full array of treatment options and options for clinical trials, which will provide more treatment options.”

Dr. Catherine Perrault, medical officer and board-certified family physician with The Mesothelioma Center’s Medical Outreach Team
“Mesothelioma is a cancer that arises from exposure to asbestos. And asbestos are little fibers. And these fibers are inhaled, and they go through our nose and our windpipe and go into the lung. And then they go to the periphery of the lung. And then on the periphery of the lung, the lining of the lung called the pleura, they can start causing inflammation.”

Dr. Jacques Fontaine, director of the Mesothelioma Research and Treatment Center at Moffitt Cancer Center
“I said to Dr. Sugarbaker, ‘Doctor, I want you to get everything you can see, everywhere you think it might be hiding and everywhere you think it might go.’ …As it has turned out, the EPP with HITHOC followed by 4 rounds of chemo was not the end of my treatment journey, but rather only the beginning. However, whatever may have occurred since, I believe that the aggressive treatment I had in the beginning was absolutely necessary to give me a chance to be here now, and I am grateful for the decision that we made.”

Michael Cole, 11-year pleural mesothelioma survivor
Pleural mesothelioma is a rare and aggressive type of cancer that grows in the pleura. The pleural membrane covers your lungs and lines your chest cavity. Its tumors can look like plaques or nodules at first. But as pleural mesothelioma progresses, tumors can merge to form a sheet-like mass. Because tumors can resemble other cancers, making an accurate diagnosis is challenging.
Doctors in the U.S. diagnose under 3,000 new cases of pleural mesothelioma each year. It’s the most common of the 4 different types of mesothelioma, making up about 75% of all cases. Pleural mesothelioma makes up 70% to 79% of all cases of mesothelioma. Doctors often call this cancer malignant pleural mesothelioma or MPM.
Given its rarity, most people diagnosed with pleural mesothelioma have never heard of it. Jeanne Niemiec, whose husband Bob received a pleural mesothelioma diagnosis in 2019, tells us how they felt when they first heard about his diagnosis. “We had no idea what it was,” Jeanne Niemiec tells us. Her husband, Bob, received a pleural mesothelioma diagnosis in 2019. “I’d never even heard of it before, and neither had Bob or our kids.”
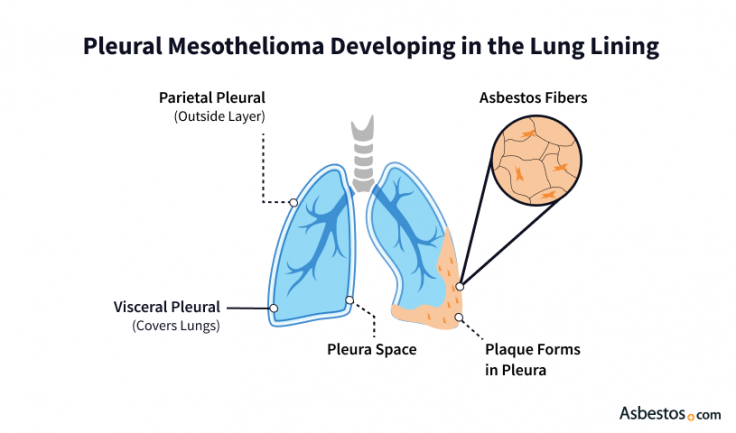
The primary cause of pleural mesothelioma is asbestos exposure. When inhaled, asbestos fibers lodge in the pleura, the thin lining made of parietal and visceral layers, where they irritate tissues, create scar buildup and may trigger cancer over decades.
Over many decades, this irritation from asbestos fibers can change cell DNA. These DNA mutations can lead to cancer. Some researchers say other factors may play a role. Radiation and genetic mutations, such as BAP1 mutations, can also contribute to the development of mesothelioma. But asbestos exposure remains the main cause.
Occupational asbestos exposure is the No. 1 cause of pleural mesothelioma. Many jobs put workers at risk of asbestos exposure. Construction, manufacturing, the military and shipbuilding industries used asbestos. While most companies phased out asbestos in the 1980s and 1990s, workers today may come into contact with older or legacy asbestos products.
Who Is at Risk of Asbestos Exposure?
People living with those who come into contact with asbestos at work can also be at risk of developing pleural mesothelioma. Asbestos fibers can be brought home on clothing, shoes, gear, skin and hair. This is called secondary asbestos exposure.
Secondary exposure led to Shaun Bigbie’s pleural mesothelioma diagnosis. His father and uncle encountered asbestos while working at the Ford Motor Company. Shaun tells us, “They think somewhere along the line, my father brought asbestos on his clothing home to me. My uncle said there were days you would just see fibers everywhere in the air.”

Get answers about treatment, top doctors, and financial support from the nation’s most trusted mesothelioma resource.
Get Your Free GuideThe most common symptoms of pleural mesothelioma are shortness of breath, back and chest pain and fatigue. Pleural effusions, or fluid around your lungs, can be one of the first signs of this disease. Pleural thickening and pleural plaques can also be signs.
Because pleural mesothelioma symptoms often mimic pneumonia or lung cancer, diagnosis is frequently delayed. Doctors diagnosed Joey Barna with pleural mesothelioma after he felt fluid in his lungs. His symptoms were first mistaken for pneumonia. Our Patient Advocates helped him get a proper diagnosis and treatment. Joey tells us he’s feeling great today and living life to the fullest.
Common Pleural Mesothelioma Symptoms
Early signs of pleural mesothelioma are mild and easy to ignore. Some people wait to see a doctor until symptoms worsen, which lessens treatment options. It’s important to talk to your doctor if you have a history of asbestos exposure, feel sick or something doesn’t feel right. Finding mesothelioma early can get better care.
Early symptoms like persistent cough, mild chest pain, and shortness of breath often appear 20-50 years after asbestos exposure and are easily mistaken for pneumonia or other respiratory conditions. Average time from first symptoms to diagnosis: 3-6 months. If you have an asbestos exposure history and persistent symptoms lasting more than 2 weeks, see a specialist immediately.
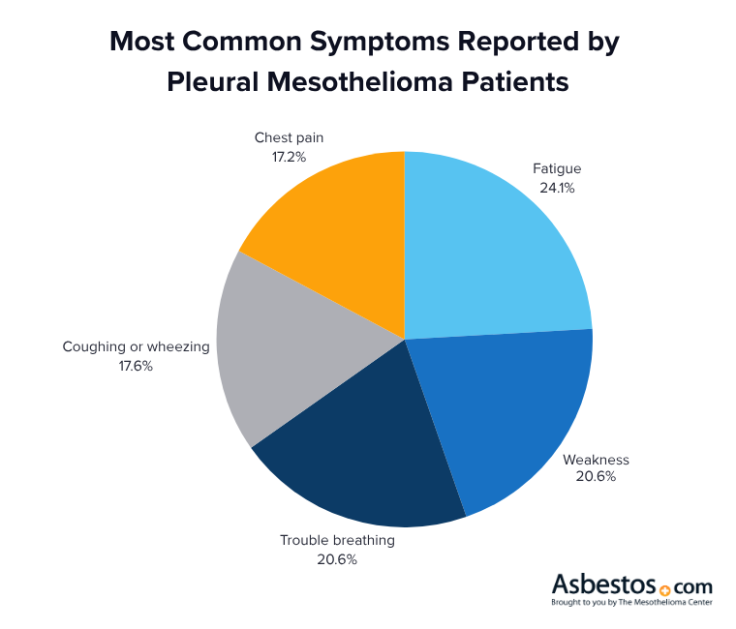
In 2025, we surveyed more than 170 people with pleural mesothelioma, caregivers and their loved ones about which symptoms they most experience. Results showed fatigue was most common. Because the symptoms of pleural mesothelioma are often mistaken for those of other illnesses, it’s best to see a doctor who specializes in treating this cancer.
A pleural mesothelioma diagnosis typically begins with a physical exam and imaging scans like chest X-rays and CT scans. If your scans show fluid buildup or pleural thickening, your doctor will order a biopsy to analyze a tissue sample. Doctors may look for biomarkers such as soluble mesothelin-related peptides (SMRP) or genetic changes like BAP1 mutations to aid in diagnosis. A biopsy is necessary to confirm a pleural mesothelioma diagnosis.
Tests Used to Diagnose Pleural Mesothelioma
Getting a second opinion from a pleural mesothelioma expert can ensure your diagnosis is correct. Seeing a specialist can get the right care. It’s OK to ask for another doctor’s opinion.
If you or a loved one is facing the uncertainty of mesothelioma, understanding the steps in the diagnosis process can help ease some of the anxiety. Here’s a simple guide to show you what to expect as you move through each stage of diagnosis. We’re here to support you every step of the way.
Initial Consultation with Doctor
Chest X-Ray
CT Scan
Biopsy
Mesothelioma Diagnosis Confirmed
Your pathology report will likely tell you the stage of your pleural mesothelioma. Stages show how far your cancer has progressed. Early mesothelioma stages mean tumors are close to the area where they first developed. Later stages mean cancer has spread further.
Pleural Mesothelioma Stages
Doctors use what’s called the TNM staging system when diagnosing pleural mesothelioma. TNM stands for tumor, node and metastasis. The system identifies the cancerous growths, their effect on lymph nodes and extent of cancer spread.
Dr. Jeffrey Velotta, a pleural mesothelioma expert at Kaiser Permanente Oakland Medical Center in California, told us about new updates to the TNM staging system for pleural mesothelioma. Dr. Velotta explains, “Standardizing measurements of tumors can help improve treatment guidelines and prognostic information.” The American Joint Committee on Cancer included more details to refine the staging process in January 2025.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your SpecialistDoctors treat pleural mesothelioma with surgery, medicine and other therapies. Sometimes, they combine more than one kind of treatment to help you feel better or live longer. Doctors call this multimodal therapy. Other care, like pain relief, also helps improve daily life.
Among mesothelioma surgeons we surveyed, nearly 67% of them reported extrapleural pneumonectomy produces the best overall outcomes for eligible pleural mesothelioma patients, highlighting its role as a leading surgical approach
In January 2025, the American Society of Clinical Oncology shared new guidelines for treating pleural mesothelioma. They now suggest using treatments that keep the lung instead of removing it. Immunotherapy is often preferred over chemo because it may help people live longer. A new drug mix, including Keytruda and chemo, was also approved to treat advanced cases.
Reflections from a Mesothelioma Survivor
Mesothelioma treatments can be tough, and things may look bad, but there is hope. Don’t give up too soon!
The Mesothelioma Center at Asbestos.com surveyed doctors and nurses in 2025 about the best treatment approaches for people with pleural mesothelioma. Respondents said the preferred treatment is chemotherapy with immunotherapy, which aligns with the newest treatment options for pleural mesothelioma.
| Treatment Approach | % of Respondents |
|---|---|
| Chemotherapy + Immunotherapy | 39% |
| Surgery (e.g., P/D or extrapleural pneumonectomy) | 18% |
| Multimodal (combination of surgery, chemo, immunotherapy, radiation) | 17% |
| Chemotherapy (e.g., pemetrexed + cisplatin/carboplatin) | 16% |
| Palliative/supportive care | 10% |
Pleural mesothelioma specialists include oncologists, surgeons and radiologists. They work at mesothelioma treatment centers across the country. Finding the right specialist for you can depend on the stage of your cancer, treatment goals and personal preferences.
Your doctor can refer you to a specialist. Patient Advocates can also match you with a specialist. They’ll find one with a lot of experience treating similar cases as yours.
“With this disease, finding a specialist is critical,” Dr. Jacques Fontaine tells us. Dr. Fontaine heads the Mesothelioma Research and Treatment Center at Moffitt Cancer Center in Tampa. “You need someone who truly understands it. They must know how to treat it aggressively for the best outcome.”

Survivor Story
Carla Fasolo: Pleural mesothelioma survivor discusses her experience receiving treatment
Pleural mesothelioma prognosis is usually poor, but outcomes are individual, and some factors can improve it. Survival rates measure the percentage of people with pleural mesothelioma who are still alive after a certain period of time. They don’t predict exactly what will happen to you. Everyone is different, and your doctor can explain what these numbers mean for you.
Life expectancy is the average amount of time a person may live with pleural mesothelioma. Life expectancy for pleural mesothelioma is often less than 18 months. The median survival ranges from 8 to 14 months. An early-stage diagnosis at a younger age increases treatment options. Aggressive treatment and good overall health are other factors that improve life expectancy.
| Pleural Mesothelioma Stage | Average Life Expectancy | 5-Year Survival Rate |
|---|---|---|
| Stage I | 21 months or more | 22.5% |
| Stage II | 19 months to 5 years | 11% |
| Stage III | 16 months to 4.5 years | 16% |
| Stage IV | 12 months to 2 years | 7% |
Predicting someone’s prognosis is complex and challenging. A number of factors play a role. Some survivors have lived with pleural mesothelioma for many years.
No doctor can determine your life expectancy based only on a diagnosis of pleural mesothelioma. This cancer advances at a rapid pace, but treatment can control it. People with pleural mesothelioma are living longer and enjoying a better quality of life thanks to treatment advances.

Exclusive Content: A Caregiver’s Perspective
Jeanette Mednicoff: Advice for someone who has a loved one diagnosed with mesothelioma
Long-time survivor Michael Cole shares his tips for living with pleural mesothelioma. He recommends staying hydrated, eating a healthy diet and staying active. He also says, “It is crucial to maintain good mental health.”
5 Tips for Living With Pleural Mesothelioma
Sissy Hoffman has lived with pleural mesothelioma for nearly 30 years since her diagnosis in 1996. She credits Dr. David Sugarbaker for her success. “Dr. Sugarbaker not only extended my life, but he forced me to live a fuller life,” Hoffman tells us. She has returned to teaching, travelling and volunteering.
We asked our team of Patient Advocates here at The Mesothelioma Center what pleural patients ask when they call us. They’ve shared these questions along with their helpful answers.
There is no sure cure for pleural mesothelioma, but treatment can help people live longer and feel better. Doctors can use medicine, surgery or other methods to slow the cancer. If the cancer is found early and removed with surgery, some people can live for years. Care teams work to give the best help possible.
Getting a second opinion from a pleural mesothelioma expert can help make sure your diagnosis is right. This rare cancer is sometimes misdiagnosed. If you were around asbestos, it’s important to talk to a doctor who knows about this disease. We can help connect you with experts and make the process easier.
If you’re not sure about your treatment choices, talking to a specialist helps. Different doctors may suggest different options, and it’s OK to ask questions. Some people choose aggressive surgery that may be hard but could extend their lives. Others may decide not to get treatment at all. It’s a personal choice.
Some families have more than one person get sick with asbestos-related diseases. This can happen when family members are exposed at work, at home or in the environment. Some people may also have higher risks because of their genes. Talk to your doctor about your risk and if you should get checked regularly.
Life expectancy for pleural mesothelioma typically ranges from 12-21 months with treatment, though this varies significantly by stage. Stage 1 patients may survive 21+ months, while stage 4 patients typically survive less than 12 months. Factors that improve life expectancy include early diagnosis, epithelioid cell type, younger age, good overall health and aggressive multimodal treatment. About 10% of patients survive 5 years or longer.
Pleural mesothelioma typically develops 20-50 years after initial asbestos exposure. This long delay occurs because asbestos fibers cause slow, cumulative damage to cells over decades. During this latency period, there are no symptoms or detectable signs. This is why most patients are diagnosed at age 65 or older, even if their exposure occurred in their 20s, 30s or 40s.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, May 29). Pleural Mesothelioma. Asbestos.com. Retrieved June 8, 2026, from https://www.asbestos.com/mesothelioma/pleural/
Selby, Karen. "Pleural Mesothelioma." Asbestos.com, 29 May 2026, https://www.asbestos.com/mesothelioma/pleural/.
Selby, Karen. "Pleural Mesothelioma." Asbestos.com. Last modified May 29, 2026. https://www.asbestos.com/mesothelioma/pleural/.

Dr. Jacques Fontaine is a thoracic surgeon at Moffitt Cancer Center in Tampa, Florida, where he heads up the Mesothelioma Research and Treatment Center. He specializes in minimally invasive robotic surgery and aggressive surgeries for mesothelioma.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
