
Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your DoctorNormothermic intraperitoneal chemotherapy is a new treatment for peritoneal mesothelioma. It delivers room-temperature chemo directly into your belly after surgery. NIPEC is still being studied in clinical trials.
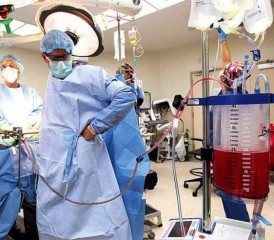
NIPEC stands for normothermic intraperitoneal chemotherapy and is used as a peritoneal mesothelioma treatment. It’s a chemo wash at room temperature that doctors put directly into the belly of people with peritoneal mesothelioma. “Normothermic” means the chemo is the same temperature as the body. NIPEC helps kill any leftover cancer cells without using the extra heat that HIPEC does.
The first dose of NIPEC is typically given 4 to 6 weeks after surgery. In rare cases or during clinical trials, NIPEC may be given before surgery. Using NIPEC before surgery is considered experimental and isn’t common.
Key Facts About NIPEC for Mesothelioma
NIPEC builds on the idea of HIPEC, which stands for hyperthermic intraperitoneal chemotherapy. HIPEC uses heated chemo during surgery and doctors give it just once. NIPEC uses chemo at normal body temperature and gives it directly into the belly over several treatments.
Some similar chemo washes include EPIC, which stands for early postoperative intraperitoneal chemotherapy. It uses chemo drugs given directly into the abdominal cavity for several hours. It’s a slightly delayed form of HIPEC. HITOC, or hyperthermic intrathoracic chemo, is also a localized chemo treatment. It’s similar to NIPEC, but it’s used in the chest cavity for people with pleural mesothelioma.
NIPEC sends chemo directly into the belly where the cancer grows to treat peritoneal mesothelioma. The chemo can reach spots where cancer cells hide between organs or in tissue folds. This direct contact given over multiple cycles allows the chemo to attack the cancer more effectively than when given through a vein.
Regular chemo doesn’t always work well for peritoneal mesothelioma because the cancer spreads across the thin lining of the belly. NIPEC lets the medicine cover a wide area inside the abdomen. This treatment targets the areas where the cancer grows the most and helps doctors fight it more directly.
You can receive NIPEC as either an inpatient or outpatient treatment. During NIPEC treatment, doctors place a small port in the belly after surgery. They use this port to send room-temperature chemo for mesothelioma straight into the belly.
The chemo spreads through the area to reach cancer cells. Doctors repeat this process every few weeks. NIPEC slows the cancer down and gives you longer breaks between treatments.
Steps to Receiving NIPEC Treatment
After your doctor removes the port, you may need to clean the wound regularly and check for signs of infection. Call your doctor right away if you see swelling, discharge or a fever that doesn’t go away.

Connect with top-rated doctors specializing in mesothelioma treatment, who will personalize treatment options based on your diagnosis.
Find Your DoctorNIPEC has several benefits for people with mesothelioma. It sends chemo straight into the belly, which helps it reach hidden cancer cells and cover a larger area than regular chemo.
Success of NIPEC for Mesothelioma
Chemo washes like NIPEC or HIPEC usually cause fewer or milder side effects than regular chemo. That’s because doctors put the medicine straight into the belly, where the cancer is. The chemo stays in that area and doesn’t have to travel through the whole body. When used after HIPEC, NIPEC may help patients live more than 30% longer.
Despite fewer issues compared to whole-body chemo, since the medicine doesn’t need to travel through the entire bloodstream, the drugs used in NIPEC still have potential side effects. This mesothelioma cancer treatment can also lead to other problems, just like any other medical procedure.
Common Side Effects of NIPEC Treatment
Most treatment centers don’t offer NIPEC. The treatment is available at Moffitt Cancer Center in Tampa, MedStar Washington Hospital Center in D.C., Memorial Sloan Kettering in New York City and Roswell Park in Buffalo. Our Patient Advocates can help you connect with these mesothelioma treatment centers and join a possible clinical trial.
Doctors are still learning how safe and effective NIPEC is before more hospitals begin using it. Dr. Paul H. Sugarbaker helped lead the way in peritoneal cancer treatment. He believes NIPEC could help patients live longer compared to HIPEC and other chemo washes.
NIPEC can cause side effects, just like any medication. Your risk of complications depends on your overall health and how far the cancer has spread.
Serious NIPEC Complications
Because NIPEC happens after surgery, people may also experience surgical complications. These can include bleeding (hemorrhages), fluid buildup (pleural effusions) and wound infections.
Serious side effects and surgical complications are rare, but it’s important to watch for any signs. If you notice anything unusual, tell your doctor right away.
You can do many things to manage side effects from NIPEC. These tips can help you feel better, stay stronger and heal faster.
Tips for Easing Side Effects
Talk to your mesothelioma doctor before you take any over-the-counter or herbal medicine. Some of these can change how your treatment works or make side effects worse.
NIPEC is for people with peritoneal mesothelioma who’ve had surgery to remove as much of the cancer as possible. Doctors look at how far the cancer has spread, how healthy the person is and if the surgeon can safely remove all visible cancer when deciding if someone can get NIPEC.
Eligibility Criteria for NIPEC
Medical doctor and Patient Advocate Dr. Snehal Smart tells us, “Peritoneal specific questions I encounter commonly are what is the NIPEC procedure, and how does a doctor determine whether that is done or not? Do they need further chemo after NIPEC?”
Meeting the eligibility requirements is important for staying safe and getting the best results from the treatment. Your doctor can help you understand the risks and benefits and decide if NIPEC is right for you. If you’re told you don’t qualify for NIPEC, you can also get a second opinion.

Discover financial assistance programs, insurance guidance, and veteran benefits to help cover your mesothelioma treatment expenses.
Get Financial HelpEach type of chemotherapy used to treat peritoneal mesothelioma works differently. NIPEC, HIPEC and EPIC all have their own pros and cons.
Undergoing NIPEC or EPIC treatments after surgery and HIPEC can lead to better survival rates compared to using chemo alone. Remember, not everyone is eligible for all types of treatment.
Most mesothelioma treatment centers don’t offer NIPEC as a standard treatment yet. You can receive NIPEC at Moffitt Cancer Center in Tampa, MedStar Washington Hospital Center in D.C., Memorial Sloan Kettering in New York City and Roswell Park in Buffalo. As doctors learn more about NIPEC, more hospitals are starting to offer it along with other treatments like HIPEC. Some people may also get NIPEC in a clinical trial.
NIPEC for mesothelioma can cause pain, but it usually happens less often and is milder than with regular chemo. Since doctors give NIPEC after surgery, you might already feel sore from the operation. Your doctor can give you medicine to help with pain or discomfort. Everyone feels different during treatment, so make sure to tell your care team how you feel. They can change your treatment to help you feel better.
Insurance coverage for NIPEC can be different for each person. Since NIPEC isn’t offered at most hospitals yet, coverage depends on your insurance plan and company. Most insurance plans cover common treatments for mesothelioma, but they may not cover treatments that are new or not yet FDA-approved. Some insurance companies might only cover part of NIPEC or may ask for special approval first. Be sure to check with your insurance provider to find out if NIPEC is covered under your plan.
Doctors are testing new treatments for peritoneal mesothelioma in clinical trials. Some of these include photodynamic therapy, gene therapy and virotherapy. New types of immunotherapy are also being studied, like CAR T-cell therapy, checkpoint inhibitors, lab-made cytokines and mesothelioma vaccines. Researchers are also trying new mixes of chemo drugs, targeted treatments that focus on mesothelioma cells and even electric current therapy to kill cancer cells.
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2026, February 11). NIPEC Treatment for Peritoneal Mesothelioma. Asbestos.com. Retrieved June 8, 2026, from https://www.asbestos.com/treatment/chemotherapy/nipec/
Selby, Karen. "NIPEC Treatment for Peritoneal Mesothelioma." Asbestos.com, 11 Feb 2026, https://www.asbestos.com/treatment/chemotherapy/nipec/.
Selby, Karen. "NIPEC Treatment for Peritoneal Mesothelioma." Asbestos.com. Last modified February 11, 2026. https://www.asbestos.com/treatment/chemotherapy/nipec/.

Karen Selby is a registered nurse and Board Certified Patient Advocate at The Mesothelioma Center with more than 30 years of experience in oncology and thoracic surgery. She worked as an operating room nurse in thoracic surgery at the University of Maryland for 6 years, assisting with surgeries such as lung transplants, pneumonectomies and pleurectomies. She later served as regional director of the tissue procurement program at the University of Florida. Karen joined The Mesothelioma Center in 2009, providing patients with personalized support and resources.
Our fact-checking process begins with a thorough review of all sources to ensure they are high quality. Then we cross-check the facts with original medical or scientific reports published by those sources, or we validate the facts with reputable news organizations, medical and scientific experts and other health experts. Each page includes all sources for full transparency.
Please read our editorial guidelines to learn more about our content creation and review process.
