Based on Your Reading:
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Hyperthermic intrathoracic chemotherapy (HITHOC) is a way of delivering chemotherapy drugs directly to the chest cavity during surgery. Some doctors recommend this procedure for patients who undergo a pleurectomy and decortication (P/D).
Written by Karen Selby, RN | Medically Reviewed By Dr. Raja Michael Flores | Edited By Walter Pacheco | Last Update: June 27, 2024
HITHOC is a special type of chemotherapy. Pleural mesothelioma patients can receive it during a major tumor-removing surgery.
After patients recover from surgery, they can receive the usual systemic chemotherapy as well.
Systemic chemotherapy is the most common treatment for mesothelioma. Systemic chemotherapy drugs are typically delivered through an IV. The drugs travel through the bloodstream to all parts of the body, killing cancer cells and slowing tumor growth.
HITHOC is considered experimental by most doctors. First, surgeons must remove all visible cancer growth through surgery. Chemotherapy drugs are then pumped into the chest cavity to soak all the organs touched by tumors, killing any cancer cells left behind.
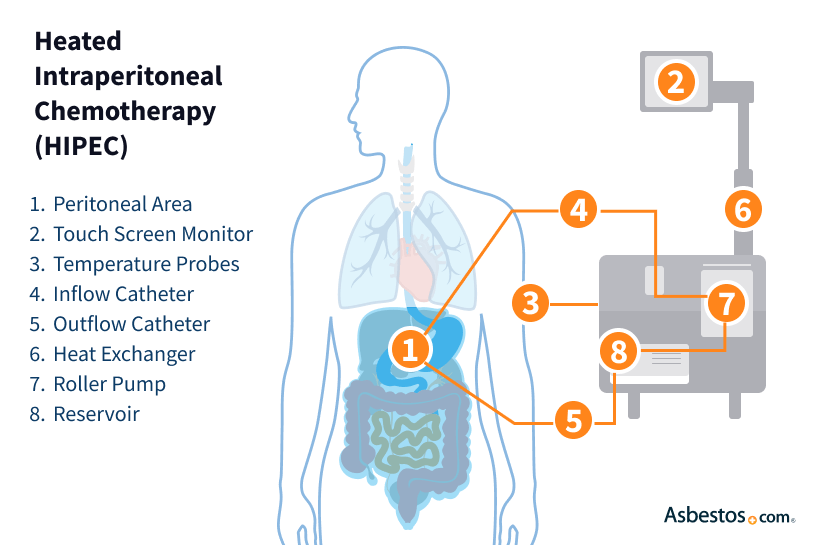
HITHOC is similar to hyperthermic intraperitoneal chemotherapy (HIPEC). It’s an established treatment option for patients who have mesothelioma in their abdomen.
So far, HITHOC has not been as successful as HIPEC. In most cases, pleural mesothelioma is harder to treat than peritoneal mesothelioma. But some doctors are hopeful the HITHOC procedure can be improved.
HITHOC is an option for patients who are strong enough to endure an aggressive treatment plan.
Some researchers suggest using HITHOC as a substitute for radiation therapy in cases where radiation is too risky.
The gold standard for extending survival with pleural mesothelioma is multimodal treatment. This usually involves a combination of invasive surgery, local radiation and systemic chemotherapy.
In some cases, surgeons must remove one lung and all the diseased tissue around it. Doctors then use radiation to kill any cancer cells left behind in the chest.
However, more often surgeons leave patients with both lungs intact.
In a pleurectomy and decortication, surgeons remove tumors around the lung and scrape cancer growth off the lung’s surface. This reduces the risk of surgical complications and leads to a better quality of life for the patient.
The problem is that it is dangerous to use radiation therapy if the lung is still in place. Lung tissue is very sensitive to radiation.
HITHOC gives doctors a safe way to potentially kill cancer cells in the chest when both lungs are present.
Patients with very little cancer spread may benefit from a combination of treatments. Lung-sparing surgery, HITHOC and systemic chemotherapy are effective for pleural patients.
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

In 2013, Dr. David Sugarbaker led a study that looked at the results for hundreds of patients who received multimodal treatment for pleural mesothelioma between 2001 and 2009.
The researchers wanted to compare patients who received HITHOC to patients who did not. In their analysis, they balanced both groups so neither group had any natural advantage outside of their treatment plan.
Based on the experience of 103 patients, the study reported a better median survival time for patients who received HITHOC.
Median Survival Time After Surgery
| Surgery | Survival Time |
|---|---|
| HITHOC Group | 35.3 months |
| Comparison Group | 22.8 months |
In a 2017 study, Italian researchers reported the results for 49 patients who received HITHOC between 2005 and 2014.
In these cases, surgeons tried to preserve lung and diaphragm function as much as possible. This way, patients would not have permanent breathing difficulty.
The researchers reported 79% of the patients were alive one year after surgery, and 45% were alive two years after surgery.
The HITHOC procedure varies depending on which mesothelioma treatment center performs it. This is a general outline.
Thank you for your feedback. Would you like to speak with a Patient Advocate?
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, June 27). HITHOC Treatment for Pleural Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/chemotherapy/hithoc/
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com, 27 Jun 2024, https://www.asbestos.com/treatment/chemotherapy/hithoc/.
Selby, Karen. "HITHOC Treatment for Pleural Mesothelioma." Asbestos.com. Last modified June 27, 2024. https://www.asbestos.com/treatment/chemotherapy/hithoc/.
A medical doctor who specializes in mesothelioma or cancer treatment reviewed the content on this page to ensure it meets current medical standards and accuracy.
Please read our editorial guidelines to learn more about our content creation and review process.
Dr. Raja Flores is chairman of the Department of Thoracic Surgery at Mount Sinai Hospital and a professor of surgery at the Icahn School of Medicine in New York City. He is a world leader in the treatment of pleural mesothelioma.
A medical doctor who specializes in mesothelioma or cancer treatment reviewed the content on this page to ensure it meets current medical standards and accuracy.
Please read our editorial guidelines to learn more about our content creation and review process.
Dr. Raja Flores is chairman of the Department of Thoracic Surgery at Mount Sinai Hospital and a professor of surgery at the Icahn School of Medicine in New York City. He is a world leader in the treatment of pleural mesothelioma.
Mesothelioma Center - Vital Services for Cancer Patients & Families doesn’t believe in selling customer information. However, as required by the new California Consumer Privacy Act (CCPA), you may record your preference to view or remove your personal information by completing the form below.
