Based on Your Reading:
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Written by Karen Selby, RN | Medically Reviewed By Dr. Jeffrey Velotta | Edited By Walter Pacheco | Last Update: July 2, 2024
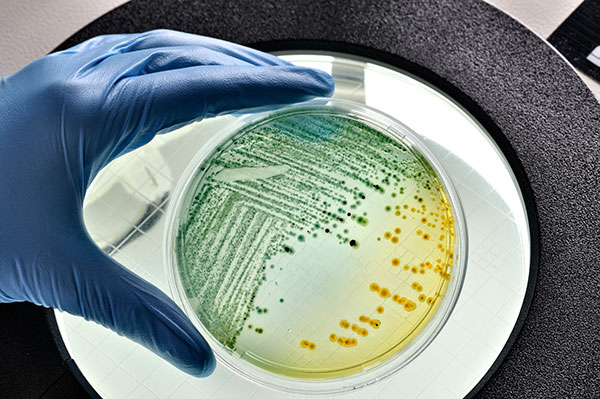
In suicide gene therapy, doctors may modify a virus or bacterium, such as E. coli. Their goal is to deliver a cancer-killing gene to mesothelioma cells.
Suicide gene therapy is one of several gene therapy techniques in development. It forces cancer cells to self-destruct. This process occurs after they are injected with modified genetic material and a particular type of drug.
Standard chemotherapy drugs damage both healthy and cancerous cells. Suicide gene therapy delivers genes that transform initially harmless drugs into highly toxic ones. The benefit is that this therapy is targeted. The toxic drugs are present only within tumor cells.
Researchers have conducted suicide gene therapy trials for several types of cancer. These include glioma, prostate cancer, ovarian cancer and mesothelioma. In theory, suicide gene therapy could be especially favorable for the treatment of pleural mesothelioma. The disease involves a thin tumor structure, limited early-stage cancer spread and easily accessible tumors.
Some early-phase clinical trials have demonstrated promising evidence of tumor regression and extended survival. The benefit is especially apparent in prostate cancer. Concerns remain about the safety and effectiveness of the technique for mesothelioma.
Improvements to suicide gene therapy are necessary. Further studies aim to maximize gene transference, increase the bystander effect and encourage antitumor immune responses. These complex biological processes will lead to more cancer cell deaths. Ongoing clinical trials have concentrated on refining these processes to boost the effectiveness of this therapy.
Suicide gene therapy ultimately uses a drug to kill cancer cells. Unlike many forms of standard chemotherapy, it is a truly targeted approach.
The most common form of chemotherapy is systemic. This means it affects all the rapidly dividing cells in the body. Systemic chemotherapy kills cancer cells but also causes collateral damage to noncancerous cells. This outcome leads to harsh side effects such as nausea and hair loss.
The goal of targeted therapy is to kill cancer cells while leaving healthy cells unharmed. Suicide gene therapy can accomplish this by ensuring the drug only becomes toxic inside tumors.
Doctors use a two-step process to prompt cancer cells to destroy themselves.
First, doctors inject a microscopic DNA-delivery vehicle called a vector into the tumor. The most widely used vector for this treatment is a genetically modified form of the herpes simplex virus. Other viruses, modified bacteria and even synthetic nanoparticles have all been tested for this purpose. The key to an effective vector is targeting mesothelioma cells.
When doctors use a virus, they alter it so it cannot reproduce or make you sick. Instead of carrying virus DNA, the virus delivers a gene into cancer cells. This gene causes the cancer cell to produce an enzyme. The genes that achieve this are herpes simplex virus thymidine kinase (HSV-tk) and cytosine deaminase (CD).
The next step occurs once the virus has implanted the suicide gene in the cancer cells. After triggering enzyme production, doctors give the patient a prodrug, a type of chemotherapy. The prodrug is normally harmless. When it comes into contact with the new enzyme, it starts a programmed cell death. Suicide gene therapy for mesothelioma typically uses ganciclovir (GCV).
The prodrug only becomes toxic in cancer cells genetically altered by the virus. This avoids the side effects associated with systemic chemotherapy. Because the virus never reproduces, only a limited number of tumor cells receive the suicide gene.
The overall effectiveness of the treatment depends on gene transference to as many cancer cells as possible as well as two other complimentary effects:
Get a Mesothelioma Treatment Guide

Find a Top Mesothelioma Doctor

Access Help Paying for Treatment

Two prominent researchers paved the way for mesothelioma suicide gene therapy: Dr. Steven Albelda and Dr. Daniel Sterman.
Albelda currently serves as the director of lung research at the University of Pennsylvania School of Medicine. Sterman is the director of the multidisciplinary pulmonary oncology program at the New York University Langone Medical Center.
Along with several associates, Albeda created a model demonstrating HSV-tk could be used as an effective treatment for peritoneal mesothelioma in 1995. Their study led to the approval of gene therapy clinical trials. Four years later, Albelda and Sterman collaborated on the first gene therapy report for mesothelioma patients.
In 1998, Sterman and colleagues evaluated patient tolerance of the HSV-tk gene and the prodrug GCV. The study was a phase I clinical trial of 21 pleural mesothelioma patients. An adenovirus delivered the gene. It was given to the patients in an intrapleural injection. The trial confirmed the safety of the treatment. Eleven patients experienced successful gene transfer.
Researchers are also experimenting with suicide genes to improve the safety of gene therapies such as anti-mesothelin CAR T-cell therapy. In 2021, scientists outlined the benefits of including a suicide gene “kill switch” in their therapy. This switch would deactivate the gene if toxicity became too high.
Researchers are determined to overcome the current weaknesses of suicide gene therapy. The central challenge is low transduction efficiency. This means cancer cells do not absorb the virus-delivered genes efficiently enough.
Improvements to the bystander effect may be propelled by integrating proteins known as cytokines. Sterman and Albelda found a way to use one cytokine, interferon (IFN)-beta. They used it to activate the immune system and prolong survival in animal test subjects. It has provided a foundation for future testing.
Researchers also theorize suicide gene therapy patients may benefit from receiving the HSV-tk gene after tumor-removing surgery. This approach is known as a multimodal treatment approach.
While clinical trials have documented safe and nontoxic patient responses to suicide gene therapy, there have also been side effects. In one study, patients undergoing chemotherapy with GCV after doses of HSV-tk experienced several reactions. These included anemia, fever, transient liver enzyme elevation, temporary inflammatory responses and bullous skin disorders. Controlling negative responses such as these is a primary goal of ongoing gene therapy research.
The U.S. Food and Drug Administration (FDA) hasn’t yet approved suicide gene therapy for widespread use, but clinical trials continue to explore ways to improve the safety and efficacy of the treatment.
Recommended ReadingThank you for your feedback. Would you like to speak with a Patient Advocate?
Your web browser is no longer supported by Microsoft. Update your browser for more security, speed and compatibility.
If you are looking for mesothelioma support, please contact our Patient Advocates at (855) 404-4592
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
The Mesothelioma Center at Asbestos.com has provided patients and their loved ones the most updated and reliable information on mesothelioma and asbestos exposure since 2006.
Our team of Patient Advocates includes a medical doctor, a registered nurse, health services administrators, veterans, VA-accredited Claims Agents, an oncology patient navigator and hospice care expert. Their combined expertise means we help any mesothelioma patient or loved one through every step of their cancer journey.
More than 30 contributors, including mesothelioma doctors, survivors, health care professionals and other experts, have peer-reviewed our website and written unique research-driven articles to ensure you get the highest-quality medical and health information.
My family has only the highest compliment for the assistance and support that we received from The Mesothelioma Center. This is a staff of compassionate and knowledgeable individuals who respect what your family is experiencing and who go the extra mile to make an unfortunate diagnosis less stressful. Information and assistance were provided by The Mesothelioma Center at no cost to our family.LashawnMesothelioma patient’s daughter


Selby, K. (2024, July 2). Suicide Gene Therapy for Mesothelioma. Asbestos.com. Retrieved July 26, 2024, from https://www.asbestos.com/treatment/suicide-gene-therapy/
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com, 2 Jul 2024, https://www.asbestos.com/treatment/suicide-gene-therapy/.
Selby, Karen. "Suicide Gene Therapy for Mesothelioma." Asbestos.com. Last modified July 2, 2024. https://www.asbestos.com/treatment/suicide-gene-therapy/.
A medical doctor who specializes in mesothelioma or cancer treatment reviewed the content on this page to ensure it meets current medical standards and accuracy.
Please read our editorial guidelines to learn more about our content creation and review process.
Dr. Jeffrey Velotta is an experienced thoracic surgeon and pleural mesothelioma specialist at Kaiser Permanente Oakland Medical Center in California. Velotta also serves as an assistant professor at the University of California, San Francisco.
A medical doctor who specializes in mesothelioma or cancer treatment reviewed the content on this page to ensure it meets current medical standards and accuracy.
Please read our editorial guidelines to learn more about our content creation and review process.
Dr. Jeffrey Velotta is an experienced thoracic surgeon and pleural mesothelioma specialist at Kaiser Permanente Oakland Medical Center in California. Velotta also serves as an assistant professor at the University of California, San Francisco.
Mesothelioma Center - Vital Services for Cancer Patients & Families doesn’t believe in selling customer information. However, as required by the new California Consumer Privacy Act (CCPA), you may record your preference to view or remove your personal information by completing the form below.
